By Marc Sorenson, EdD, Sunlight Institute
A good, sound sleep is important to human health, both physical and mental. According to Dr. Diana Grigsby-Toussaint, “Studies show that inadequate sleep is associated with declines in mental and physical health, reduced cognitive function, and increased obesity.” She and her colleagues at the University of Illinois recently published a new study demonstrating that a natural environment may help people get the sleep they need.[1] The study showed that exposure to nature, which they dubbed “greenspace,” was associated with a more restful sleep. Other surroundings such as a sandy beach with an ocean view were also conducive to better sleep. One of the measurements used to qualify an area as greenspace was the availability of sunlight.[2]
I can attest to the fact that when I regularly walk through the pines and aspens located in the high mountains near my Nevada ranch, I sleep better at night. When I don’t get enough outdoor time in the trees and sunlight, I begin to suffer from what my friend, Dr. William Grant, calls nature-deficit disorder, or NDD. My whole mood is altered, and not for the better. Dr. Grant is not only a great sunlight scientist, but an avid birdwatcher, which takes him out daily do get his dose of nature.
We have a primal need for sunlight and natural surroundings, and too many city dwellers do not connect with sunlight and nature. Don’t fall into that trap. There is an adage that says, “What gets scheduled gets done.” Plan to be outside as often as possible and soak up some sun when it is available. Natural surroundings with sunlight are better than any psychiatrist or physician for maintaining mental and physical health.
[1] Grigsby-Toussaint DS, Turi KN, Krupa M, Williams NJ, Pandi-Perumal SR, Jean-Louis G. Sleep insufficiency and the natural environment: Results from the US Behavioral Risk Factor Surveillance System survey. Prev Med. 2015 Sep;78:78-84.
[2] http://news.aces.illinois.edu/news/u-i-study-men-people-over-65-sleep-better-when-they-have-access-nature.
By Marc Sorenson, EdD, Sunlight Institute
Are you suffering from anxiety disorder, but fear taking drugs? Your fear is well-founded. It has been shown that a class of drugs called anti-anxiety drugs, i.e. valium and Xanax, and sleep aids like Ambien, Sonata and Lunesta lead to increased risk of death.[i] During 7.6 years, and after controlling for other factors such as sleep disorders, anxiety disorders and other psychiatric illnesses, it was found that the risk of dying was 3.46 times higher in those who took the drugs compared to those who did not. Considering the material we have posted on this site regarding brain disorders, insomnia, and sunlight, it seems reasonable to believe that a better and less dangerous anxiety-treatment option would be regular sunlight exposure.
Research from Denmark has shown that morning light, made to mimic daylight, relieves anxiety by reducing the activity of the brain’s fear center.[ii] The efficacy of the light treatment was based on the intensity of the light: the greater intensity, the greater the effect.
Another scientist, Dr Klaus Martiny, commented on the above study and noted that morning light improves sleep. “A lack of daylight disrupts some hormonal processes in our body that regulate our circadian rhythm. This can result in a shift in circadian rhythm, so that people go to sleep later and later in the evenings, and this shift is associated with an increased risk of depression.”[iii]
Martiny suggested that a good rule of thumb is to go to sleep before midnight and awaken before 8:00 AM. However, we discussed in the post on obesity that the earliest morning sunlight was associated with a remarkably lessened risk of obesity, which was also attributed to resetting the circadian rhythm. We therefore suggest that a better rule of thumb is to be outside for a half-hour when the sun rises each morning.
Get your morning sunlight, your midday sunlight and your afternoon sunlight. Sunlight is the great healer.
[i] Weich S, Pearce H, Croft P, Singh S, Crome L. et al. Effect of anxiolytic and hypnotic drug prescriptions on mortality hazards: retrospective cohort study. BMJ 2014;348:g1996.
[ii] Christensen B. Morning light relieves anxiety. Science Nordic 2014. http://sciencenordic.com/morning-light-relieves-anxiety Accessed August 8, 2015.
[iii] http://sciencenordic.com/morning-light-relieves-anxiety. Accessed August 8, 2015
By Marc Sorenson, EdD, Sunlight Institute
Sunlight, through regulation of the proper circadian rhythms, influences the health of nearly the entire the human body.
Circadian rhythms are variations in physiology and behavior that persist with a cycle length close to, but not exactly, 24 hours. It is necessary to synchronize the rhythms on a regular basis to maintain them, and such synchronization is achieved through regular exposure to light and darkness.[i] This is also known as “resetting the biological clock.”
Circadian rhythms include sleeping and waking in animals, flower closing and opening in angiosperms, and tissue growth and differentiation in fungi.[ii] There are other factors besides light and darkness that have an influence on either synchronization or desynchronization of the clock, but they play a small part. For the purpose of this book, we will consider the influence of light in maintaining proper circadian rhythms, and by so doing, enhance human health. Researchers have stated that “Mammalian circadian rhythms form an integral physiological system allowing for the synchronization of all metabolic processes [emphasis mine] to daily light/dark cycles, thereby optimizing their efficacy.”[iii] Anything that has a profound effect on all metabolic processes is obviously important to the proper functioning of the human organism.
When circadian rhythms are disrupted (or de-synchronized), it upsets the physiology of the human body. People who take long flights across many time zones often feel “out of sorts” and many have a difficult time in adjusting to time zones to which they are not accustomed. We call this “jet lag,” and it is a common manifestation of a desynchronized rhythm. Another is night-shift work. When the body is expecting bright light and instead is exposed to dimness or darkness, its attempts to resynchronize can cause cloudy thinking, fatigue, and even more destructive damage to the psyche and physiology.
There are innumerable research papers that demonstrate the health detriments of a desynchronized circadian rhythm. For example, research on rats shows that desynchronization leads to premature cellular aging,[iv] as measured by telomere length (a DNA marker for life span); the shorter the telomeres, the shorter the life span. Young rats that were “jet-lagged” had aging characteristics of middle-aged rats.
It also appears that circadian disruptions change the structure of important proteins that play a protective role in cancer, thereby increasing the risk of breast cancer.[v] Other research has demonstrated that disruption of circadian rhythms may lead to a profound increase in the risk of heart disease, metabolic syndrome and other cancers;[vi] [vii] even the risk of poor dental hygiene and dental caries may be increased by desynchronized circadian rhythms.[viii]
One might ask why I am making such an emphasis on circadian rhythms. Here is the answer: Sunlight can, and should, reset the circadian clock daily; it is the timing cue, also called a zeitgeber, which entrains the physiologies of humans and thereby helps to prevent critical illness.[ix] [x]
This is another positive benefit of sunlight that occurs apart from vitamin D production.
[i] Duffy J, Cziesler C, Effect of Light on Human Circadian Physiology. Sleep Med Clin. 2009 June; 4(2): 165–177.
[ii] http://dictionary.reference.com/browse/circadian%20rhythm?s=t
[iii] Mitchell MI, Engelbrecht AM. Circadian Rhythms and Breast Cancer: The Role of Per2 in Doxorubicin-Induced Cell Death. J Toxicol. 2015;2015:392360.
[iv] Grosbellet E, Zahn S, Arrivé M, Dumont S, Gourmelen S, Pévet P, Challet E, Criscuolo F. Circadian desynchronization triggers premature cellular aging in a diurnal rodent. FASEB J. 2015 Aug 10. pii: fj.14-266817. [Epub ahead of print]
[v] Mitchell MI, Engelbrecht AM. Circadian Rhythms and Breast Cancer: The Role of Per2 in Doxorubicin-Induced Cell Death. J Toxicol. 2015;2015:392360.
[vi] Vignesh Shanmugam, Amro Wafi, Nawaf Al-Taweel and Dietrich Büsselberg. Disruptions of circadian rhythm
Increase the risk of cancer, metabolic syndrome and cardiovascular disease. Journal of Local and Global Health Science, 2013:3.
[vii] Bratsun DA, Merkuriev DV, Zakharov AP, Pismen LM. Multiscale modeling of tumor growth induced by circadian rhythm disruption in epithelial tissue. J Biol Phys. 2015 Aug 21. [Epub ahead of print]
[viii] Lundgren AM, Öhrn K, Jönsson B. Do adolescents who are night owls have a higher risk of dental caries? – a case-control study. Int J Dent Hyg. 2015 Jul 22. doi: 10.1111/idh.12165. [Epub ahead of print]
[ix] Remi J. Humans Entrain to Sunlight – Impact of Social Jet Lag on Disease and Implications for Critical Illness. Curr Pharm Des. 2015;21(24):3431-7.
[x] Hasegawa Y, Arita M. Circadian clocks optimally adapt to sunlight for reliable synchronization. J R Soc Interface. 2013 Dec 18;11(92):20131018
Sunlight, UVA and nitric oxide. Another answer to covid?
Sunlight is indeed another answer to profoundly reducing the risk of Covid. By Marc Sorenson, EdD.
Sunlight is associated, with lower illness and death from the Covid-19 virus.
So says new research from the British Journal of Dermatology. I opine that this research is of epochal importance, and it is something I postulated a year ago. At that time, certain people mocked and belittled me. It seems like the “experts” of the world had a laser focus on producing a vaccine. Thus, they denigrated anything or anyone who did not follow their dictatorial rules. Consequently, I was gratified when this research appeared.
First of all, for the purposes of the Journal research into sunlight, the investigators assessed deaths from covid-19 at the county level across the USA. They then replicated the measurements in England and Italy. The researchers then measured the amount of sunlight in each county in Kilojoules, a unit of heat equal to .239 calories.
Furthermore, after measuring the sunlight and death from Covid-19, they adjusted their data for demographic, socioeconomic and environmental variables.
This part of the sunlight research is especially relevant:
“Only areas where UVB was too low to be inducing significant cutaneous vitamin D3 synthesis were modelled.” This took vitamin D out of the equation.
UVB light stimulates vitamin D production when it makes contact with the skin. Therefore, ensuring no vitamin D production (by eliminating UVB light), they eliminated a potential misconception. There was no way vitamin D could be the mechanism of action to decrease Covid-19. Thus, one might say that this was was a pure sunlight study, and the idea to eliminate vitamin D was pure genius.
Too many people believe that if sunlight exposure has a positive effect, the mechanism must be through vitamin D. This research corrects that theory.
So what is the mechanism, if it is not vitamin D? The answer is nitric oxide (NO). Sunlight exposure also produces NO in the skin. Yet, NO occurs in skin after exposure to UVA rays, not the vitamin D-producing UVB. In addition, NO has the ability to stop the replication of the Covid virus. One of the beauties of this system is that UVA rays and NO are available at any season when the sun is shining. This indicates that this healing action of sunlight is also available year-around.
The results:
The mortality risk ratio (death risk ratio) due to Covid-19, over the three countries, estimated a decline of 32% for each increase in 100 kilojoules per meter2. Thus, as sunlight intensity increased, death from Covid-19 decreased concomitantly. It seems like a great idea to increase exposure to non-burning sunlight among all areas where Covid-19 exists.
Certainly, the lockdown was a great detriment to human health.
For more information on sunlight and health, visit sunlightinstitute.org and read the book, Embrace the Sun.
Happy Sunning!
Indoor living: What is the cost in sunlight? By Marc Sorenson, EdD.
Indoor living is potentially debilitating because it creates an unnatural environment, especially when carried to extremes. It pollutes our surroundings, and because it places us in an abnormal ambience, robs us of our natural existence. Now, no one should suggest that I want the populace to be outside 24 hours per day. Nevertheless, it seems like we are relentlessly pursuing the opposite—a world of 24 hours per day inside. In the last few decades, we have moved indoors from a mostly agrarian society. Thus, we have lost our hard physical labor, our contact with the earth, and our fresh air. Another vital loss has been the loss of sunlight, our greatest healer.
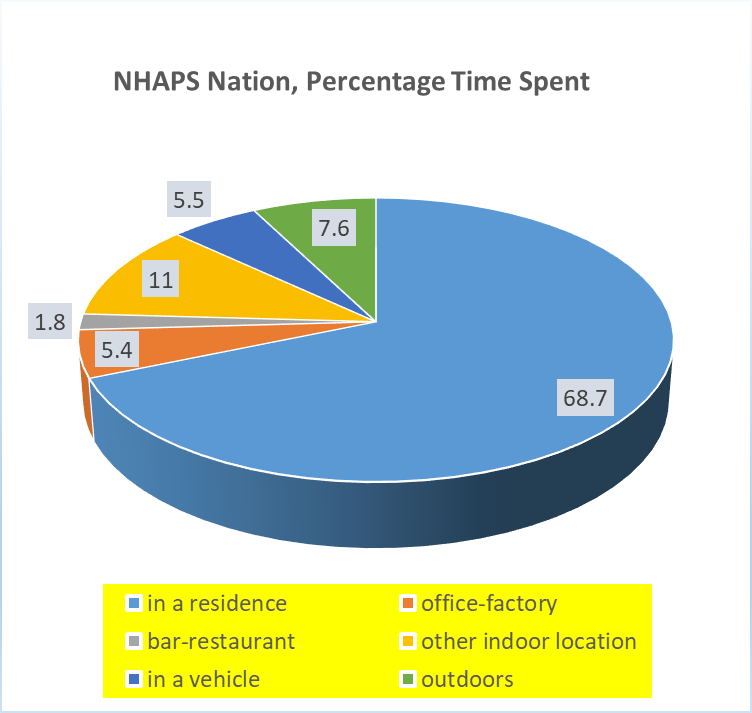
So just how much time do we spend in indoor living? The National Human Activity Pattern Survey (NHAPS) summed it up quite well with the use of a chart.
One gleans from the chart that we spend 87% of our time indoors, plus another 6% inside a car. That is almost no outdoor living at all!
To an extent, we engage in indoor living because we fear the sunlight, and especially melanoma.
Considering the chart data, it makes one wonder why we fear the sunlight so much. Yet, the media constantly bombards us with messages to avoid sunlight and further endanger ourselves by slathering ourselves with sunscreens. Sunscreens, of course, are another method to reduce the minuscule quantity of sunlight available to our sedentary, indoor lives. That sunlight might otherwise find its way to the skin and save our lives.
Fear of melanoma is one major factor that has driven us to indoor living and poor health.
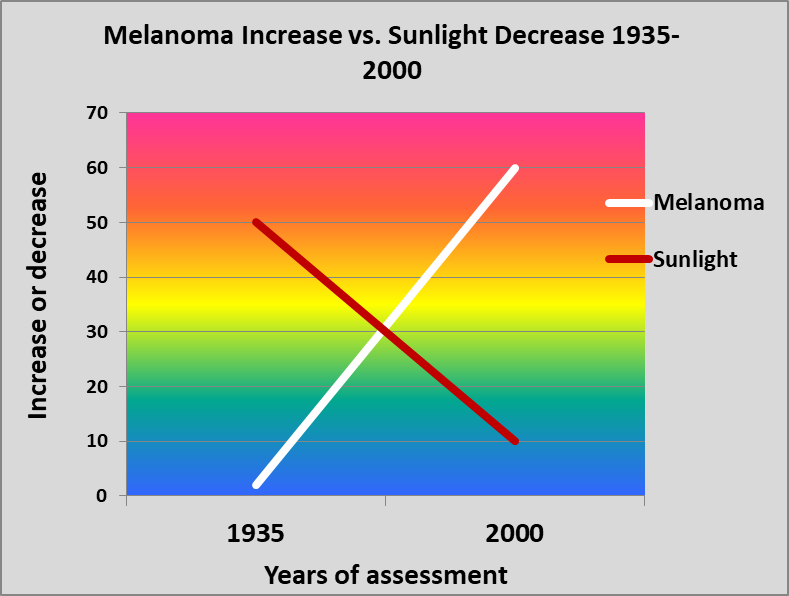
The Melanoma International Foundation stated that melanoma has increased alarmingly since 1935. They show that in that year, approximately one in 1500 people had a melanoma diagnosis. They then said that people had 30 times the risk of melanoma in 2010-2014 as they did in 1935 and blamed the increase on increasing sun exposure after 1935. Nevertheless, as melanoma increased, sun exposure decreased by about 90%! Most agrarian and other outdoor jobs nearly disappeared. For a full analysis of this counterintuitive message from the dermatologists, read the book, Embrace the Sun.
One might think that since indoor living increased so profoundly, melanoma should also decrease profoundly.
Here is another chart that I prepared for Embrace the Sun. It shows the spectacular increase in melanoma that accompanied the remarkable decrease in sun exposure.
For robust health, we must eschew a life of nearly total indoor living and return to the natural, outdoor lifestyle. We must also obtain some regular, non-burning sunlight without sunscreen.
For more about the myriad benefits of sunlight on health, visit Sunlight Institute and read the book, Embrace the Sun. Remember to avoid sunburns.
HAPPY SUNNING!
Senior citizens obtain plenty of vitamin D from sunlight. By Marc Sorenson, EdD
Senior citizens, and middle-aged citizens, according to some experts, cannot produce as much vitamin D from sun exposure as young people. Thus, to prevent vitamin D deficiency, medical professionals may recommend vitamin D supplementation to make up the gap. Nevertheless, I know first-hand there is no problem for senior citizens to optimize vitamin D levels by using sun, sans supplementation. I mentioned in a recent blog that one of my friends, Wayne, was able to achieve a level of over 100 ng/ml. This was spectacular, since an optimal level is 60-80 ng/ml. Wayne achieved his vitamin D levels due to spending much of his daily time sunbathing. Consequently, I was surprised at his result, and so was his physician, who told him to stop taking supplements immediately.
The doctor likely did not know senior citizens could achieve elevated vitamin D levels while sunbathing. He probably thought that Wayne’s results were impossible.
The doctor was amazed when Wayne told him he had never taken a D supplement and used sunlight only. While production of vitamin D in human skin decreases with age, it does not decrease to zero. In addition, Wayne was living proof that what senior citizens need is more sun exposure. Wayne was in his seventies. Thus, the extra sun exposure balances any decrease of vitamin D production due to age. Hence, it simply takes a bit longer for higher levels to result.
New, corroborating evidence confirms the efficacy of sunlight for senior citizens.
A recent study confirms sunlight is almost as effective for seniors as younger people, for vitamin D production. The study measured the response of vitamin D metabolites after a 30-minute bout of sun exposure. First of all, the investigators exposed the subjects to 30 minutes of sunlight at solar noon. In addition, the exposure was broken up into 15 minutes each on the ventral and dorsal sides of their bodies. The subjects included 30 healthy individuals. They divided into two groups according to age. Eighteen of them were 20-37 years old and 12 of them were 51 to 69 years old. The researchers assessed serum vitamin D levels at baseline and 72 hours after the sun exposure. They also assessed the older group again after 168 hours.
A synopsis of the results and conclusions
After sun exposure of 72 hours, vitamin D increased in both younger and older groups. Yet, the increase was greater in the younger group. Furthermore, Vitamin D production decreased by 13% per decade of age. In conclusion: “Serum D3 concentration increased significantly in response to outdoor sun exposure in younger and older adults. While ageing may dampen cutaneous synthesis, sunlight exposure is still a significant source of vitamin D3.”
This research, and the remarkable results of my friend Wayne, indicate that all ages can effectively use sunlight. Sunlight will stimulate the production of a bounteous harvest of vitamin D by the skin. Furthermore, the sun’s rays will produce another bounteous harvest of health benefits that have nothing to do with vitamin D. A pill will never achieve these benefits.
For more information regarding the effects of sunlight on health, visit sunlightinstitute.org and read the book, Embrace the Sun.
Pediatric multiple sclerosis. Can sun exposure prevent it? By Marc Sorenson, Ed.D
Pediatric multiple sclerosis rarely receives much study since multiple sclerosis is a disease that usually develops in young adulthood. That lack of research is a mistake and may be leading to unnecessary death and disability. Simple sun exposure may diminish or eliminate the disease. So how many children’s (and young adults’) lives have been destroyed by problems caused by this insidious disease? In addition, could proper use of heliotherapy (sun treatment) prevent the disease? I opine that this disease follows the admonition: “An ounce of prevention is worth tons of cure.”
What is pediatric multiple sclerosis?
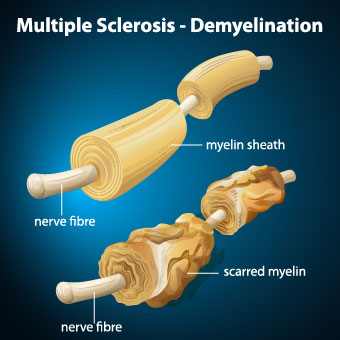
Multiple sclerosis is an autoimmune disease in which T-cells initiate an inflammatory response against myelin, the protective cover of nerves. In other words, the immune system attacks itself and leads to terrible destruction. This process, known as demyelination, leaves the nerves bare and susceptible to “short circuiting.” From 85 to 170 people per 100,000 in the USA suffer from MS. In addition, women’s risk, from 1991 through 1994, increased by 50% compared to the period from 1982 through 1986.
Multiple sclerosis affects about 400,000 Americans and about 2.5 million people worldwide. There may also be many more yet-undiagnosed cases of MS in the population. Pediatric multiple sclerosis occurs in babies and children.
What does the research show about sunlight and pediatric multiple sclerosis?
A study presented in the virtual Americas Committee for Treatment and research in Multiple Sclerosis Forum 2021, has stunning implications. The meeting, known as ACTRIMS, had many important findings. Probably, the most important finding had to do with sunlight and pediatric multiple sclerosis. A medial student at the Australian National University in Canberra, Prince Sebastian, presented investigation and results:
“Low Sun Exposure is a Risk Factor for Pediatric-Onset Multiple Sclerosis,” was the title of the research. It found that spending at least 30 minutes in outdoor sunlight daily associated to a significantly reduced risk factor for pediatric multiple sclerosis.
More information on the research.
The study used 16 pediatric centers. There were 332 children with pediatric-onset multiple sclerosis who formed the subjects. Another 534 healthy children served as controls for purposes of comparison and conclusion. Researchers analyzed associations between time spent outdoors in the summer (sun exposure) between subjects and controls. Thus, they were able to compare the risk of pediatric multiple sclerosis to amount of sun exposure.
The conclusions were remarkable. The investigators compared children who spent less than 30 minutes outside to those who spent up to more than an hour outside. Those who spent more time outside had a 2.6 times lower risk of pediatric multiple sclerosis. Most noteworthy, however, was that spending one-two hours outside predicted a 7.4 times lesser risk of the disease!
It would be difficult to argue with this study.
The message it sends is that sunlight is a gift to mankind. In addition, do not engage in child abuse by keeping children out of the sunlight!
For vital information on sunlight, multiple sclerosis and health, visit sunlightinstitute.org and read the book, Embrace the Sun.
Insufficient sunlight associates in a dose-response manner to higher risk of hypertension and earlier death. By Marc Sorenson, EdD. 
Understanding hypertension
Hypertension, or chronic high blood pressure, depends on the amount of blood the heart pumps and resistance to arterial blood. Thus, the tighter the arteries, the higher the blood pressure. The top number on a blood-pressure measurement, and stated in millimeters of mercury (mm/Hg), is systolic pressure. In addition, the lower number is diastolic pressure, another critically important measurement. Hypertension occurs when blood pressure is greater than 140/90 mm/Hg. Thirty-one percent of US adults are hypertensive. Hypertension can damage arterial walls and can eventually lead to an increased risk of death from heart disease, heart failure, and other arterial diseases. It also associates to a higher risk of kidney disease, irregular heart rhythms, osteoporosis, cognitive dysfunction, painful intercourse and stroke.
Does insufficient sunlight exposure influence hypertension?
Conventional textbook theory holds that the brain, blood vessels, and kidney regulate blood pressure. However, recent evidence suggests that the skin could also regulate hypertension, and insufficient sunlight plays a role in increasing it.
Insufficient sunlight, as mentioned, leads to a spate of diseases and disorders. In addition, some of those diseases have a dose-response relationship with sun exposure.
Hypertension is one of those diseases and can lead to disability and death. Blood pressure between 80 (diastolic pressure or lowest pressure) and 120 systolic (higher pressure), is in normal ranges. When blood pressure rises substantially above either of these figures and stays elevated, it is a danger signal.
Understanding the dose-response relationship.
So, what is a dose-response relationship (DRR)? This is where changes in one measured factor produces a predictable, consistent change in another measured factor. Thus, if I increase my exercise a certain amount weekly, I probably hope for a dose-response outcome: predictably better endurance. Consequently, if my body increases its endurance each week, my exercise produces a dose response relationship with endurance. Conversely, if someone stops exercising and loses a predictable amount of endurance, this is also a DRR (negative DRR).
An illustrative example of positive sunlight (rather than insufficient sunlight) and DRR.
My friend Wayne had severe hypertension when checking in at our former resort. After sunbathing each day for a month, hypertension decreased profoundly.
Wayne arrived with blood pressure of 157 systolic and 97 diastolic (157/97). Both of these measurements are dangerously high. Four weeks later, without medication, and while taking no vitamin D, the numbers dropped to 125/54. He had progressed from very high stroke risk to very low stroke risk. In addition, his vitamin D levels climbed to 103 ng/ml, a number I considered impossible without supplementation. I learned much, especially about sunlight, vitamin D levels and hypertension. Sufficient sunlight is a key to optimal levels of blood pressure. Many people believe that older persons cannot raise vitamin D levels. Yet, Wayne was in his seventies. Furthermore, insufficient sunlight was obviously a major cause of his hypertension. Wayne’s DRR occurred with the increased sun exposure and produced optimal blood pressure.
The latest research regarding insufficient sun exposure and hypertension
This latest research on insufficient sun exposure began by noting another important, but misleading fact. An inverse association exists between cardiovascular disease (CVD) and vitamin D levels. Yet, as the authors mentioned, trials of vitamin D supplementation seem to show no benefits for CVD. In addition, they state that benefits of high vitamin D levels for CVD might be a marker for something else. That something, of course, is probably sunlight. In their research, carried out by questionnaire, 23,593 women answered questions regarding melanoma. In addition, they also related factors of possible interest for hypertension. Those factors included detailed sun exposure habits, marital status, education, smoking, alcohol, BMI, exercise and chronic stress. Hypertension-medication use from 2005-2007 became the measurement tool used to determine hypertension incidence among members of the study group.
All subjects filled out a questionnaire to determine sun-exposure and sun-bed habits:
- Do you sunbathe during summer?
- Do you sunbathe during winter vacation?
- Do you travel south to sunbathe?
- Do you use a sun bed?
The investigators deemed that women answering ‘yes’ on one or two questions had moderate sun exposure. Those answering ‘yes’ on three or four questions had the greatest sun exposure.”
The main goal was to assess hypertension risk associated with sun exposure, after adjusting the data for any confounding factors.
Here are the results:
- When compared with women with high sun exposure, those with low sun exposure were 41% were more likely to have hypertension. For moderate sun exposure, the women were 15% more likely to have hypertension. Hence, this is another example of a dose response relationship (DRR). The lower the sunlight exposure, the greater the risk of hypertension.
- Other risk factors for hypertension were lack of exercise, darker skin, chronic high stress and lack of university education.
- The researchers concluded, “That in our observational design sun exposure was associated with a dose-dependent reduced risk of hypertension…. [This] might partly explain the fewer deaths of [from] cardiovascular disease with increasing sun exposure.”
Hypertension is serious, and a major cause of death, which is inversely associated to sun exposure. Therefore, regular, non-burning sun exposure can provide one of the best protections against this insidious disease.
For more information on sunlight and health: https://sunlightinstitute.org/ and read the book, Embrace the Sun.
Sunlight and food allergies are negatively associated. By Marc Sorenson, EdD.
Do certain foods cause you to break out in hives, or cause pain and discomfort? Then you may have an allergy and thus a hypersensitivity to the food. An allergy is a damaging immune response to a particular substance, to which the body is hypersensitive. In addition, in the case of anaphylaxis, it can be deadly. Sunlight and food allergies relate closely to each other, that is, in a good way. Hence, sunlight may have a place in stopping the allergic reactions.
A review of research on vitamin D, sunlight and food allergies makes some interesting statements. [1] First of all, the researchers state that since 2007, most epidemiologic studies have supported low sunlight, as a risk factor for food allergy. They then note that studies that looked directly at vitamin D status as measured by serum vitamin D levels are not nearly as consistent as studies on sunlight and food allergies. They state: “Although conflicting, the vitamin D studies suggest a more complicated association than a linear dose response in all individuals…”
However, sunlight exposure produces a different outcome for allergies.
Their summary is telling: “Many studies have linked sunlight with the development of food allergy. “However, whether this [directly relates] to vitamin D status or other sunlight-derived, seasonal and/or geographic factors remains uncertain. More studies are needed to investigate the role of sunlight and vitamin D status in food allergy because of their potential for primary prevention and disease modification.” Sunlight and food allergies may have a negative association. If more sunlight is available, fewer food allergies may occur.
This is another of those scientific papers that illustrates that sunlight exposure is nearly always protective against the studied disease. Yet, there is much more room for argument when vitamin D serum levels are used.
It is sunlight, not vitamin D, which makes the difference.
My takeaway? Sunlight and food allergies, since they are negatively related, speak to the importance of obtaining sufficient time in the sun. Get sufficient exposure to non-burning sunlight on a regular basis. That will provide plenty of vitamin D when one needs it. In addition, it also provides nitric oxide, endorphins, serotonin, dopamine, BDNF and other photoproducts yet unnamed. Thus, we must cease to equate sunlight exposure only with vitamin D. If vitamin D is our goal, and we neglect sunlight, we do a disservice to other healthful effects of sunlight. Furthermore, we must understand that a pill can never replicate the magnificent and essential powers of the sun.
Be sure to obtain your share of non-burning healing sunlight. For more information on the healing powers of sunlight, visit https://sunlightinstitute.org/. In addition, read the book, Embrace the Sun.
Diabetes and sunlight. Is there a connection? By Marc Sorenson, EdD.
Diabetes associates with sunlight. Yet, please understand that lack of sunlight is not the primary cause of the disease. Nevertheless, sun exposure can act as an adjunct to the primary healing methods, which are nutritional changes and more exercise. My wife and I saw first hand, the efficacy of sunlight and good nutrition. During our 15 years at our former health institute, our clients lost more than 100 tons of fat. In addition, two-thirds of diabetic guests were free of all medication in less than two weeks. If clients stayed four weeks, there was about an 85% cure rate, and the remainder profoundly lowered medication. Sunny Southern Utah furnished the sunlight; we furnished the nutrition, exercise and expertise.
What is diabetes?
Diabetes is a disorder of chronically high blood glucose and it leads to blindness. It also leads to nerve damage, heart disease, kidney disorders, neuropathy and other maladies. Furthermore, it is so deadly that some experts believe it will ultimately destroy our health care system. Due to a change to a high fat, junk-food diet, this destruction of health care presently exists in China. In addition, diabetes was the seventh leading cause of death in the United States in 2017. Thus, 83,564 death certificates listed diabetes as the cause of death. Furthermore, it is important to understand that death certificates underestimate the carnage effected by diabetes. Most noteworthy is that diabetes contributes to far more than 83,564 deaths. Therefore, when researchers listed diabetes as the underlying or contributing cause of death, the number of deaths skyrocketed to 270,702.
Two forms of the disease: Both associate with lack of sunlight.
Diabetes comes in two forms: (1) Type-one diabetes occurs due to autoimmune response, thus damaging the insulin-producing islet cells. This damage consequently reduces production of insulin, which is responsible for removing glucose from blood and storing it in tissue. Only about 5% of diabetics are type-one. (2) Type-two diabetes, in which there is sufficient insulin, yet blood glucose remains high due to insulin resistance. This discussion involves type-two.
Most noteworthy, as with heart disease, a paucity of sunlight is not the primary cause. Rather, deleterious nutrition habits are the main reasons. These habits are principally high meat consumption, sugar consumption, egg consumption, low consumption of fruits and vegetables, and too many fried foods. In the case of type-one diabetes, milk consumption is probably the most important nutritional factor. Yet, sunlight may act as a prophylactic against both types of the disease. Especially relevant is that diabetes probably does not kill someone directly. Rather, it is the diseases resulting from diabetes, which lead to death.
The influence of sunlight on this disease.
There are several studies showing a relationship between type-two and sun exposure. Hence, one paper showed that blood-sugar levels were lower during summer, indicative of a protective effect of summer sun. Another, a meta-analysis, produced moderate evidence that recreational sun exposure associates with a reduced risk of type-two . The study materialized because the researchers observed that higher vitamin D levels associated with lower diabetes risk. Yet, vitamin D supplementation did not associate with lower risk. They hypothesized sun exposure could have influences unrelated to vitamin D, and such seems to have been the case.
Perhaps the most important investigation showed that women who had “active sun exposure habits” had a 30% decrease in the risk of type-two diabetes. It seems like being a regular participant in sunny activities is a good idea, no? Therefore, enjoy regular, non-burning sun exposure, avoid junk foods and prevent or heal this disease.
For more information on sunlight and health, visit sunlightinstitute.org. In addition, read my book, Embrace the Sun.