Bone strength influenced by the body’s circadian rhythms and sunlight . By Marc Sorenson, EdD.
Bone strength and its link to circadian rhythms
Important definitions and explanations regarding bone strength:
The quantity of bone tissue that either enters the bone, or leaves the bone, determines bone mass and strength.
- Osteoclasts are multi-nucleus bone cells that break down bone tissue. Their function is critical in the maintenance, repair, and remodeling of bones of the vertebral skeleton. They remove old bone and make way for new. Thus, they are always at work breaking down bone.
- Osteoblasts are cells that make and maintain bone. They do so by producing a matrix and then mineralizing it. Therefore, osteoblasts strengthen bone and increase bone mass.
- The balance between osteoclasts and osteoblasts determine the strength of our bones. Unfortunately, many bone drugs work by stopping osteoclasts, thus preventing bone remodeling. Hence, these drugs are disastrous and may cause necrosis (death of bone within bone).
- No matter the calcium consumed, bone will weaken and diminish without something to promote the work of osteoblasts. Hence, osteoporosis results.
Understanding the circadian rhythm
Circadian rhythms are variations in physiology and behavior persisting with a cycle length close to, but not exactly, 24 hours. It is necessary to synchronize the rhythms on a regular basis to maintain them, and such synchronization occurs through regular exposure to light and darkness. Proper circadian synchronization is vitally important because myriad diseases occur without it.
Circadian rhythms include sleeping and waking in animals. In addition, they balance flower closing and opening in angiosperms and tissue growth in fungi. In addition, researchers also have stated, “Mammalian circadian rhythms form an integral physiological system allowing for the synchronization of all metabolic processes to daily light/dark cycles….” Probably, anything with a profound effect on all metabolic processes is important to the proper functioning of the human organism.
Other important actions of the Circadian rhythms, including effects on bone strength.
It also appears that circadian disruptions change the structure of important proteins, which play a protective role in cancer—thereby increasing the risk of breast cancer. Another study has demonstrated that disruption of circadian rhythms may lead to a profound increase in the risk of heart disease, metabolic syndrome, lung cancer and other cancers; even the risk of poor dental hygiene and dental caries increase with desynchronized circadian rhythms. See the entire discussion in the book Embrace the Sun.
Sunlight, circadian rhythms and bone strength
I thought I had read nearly everything written and published about circadian rhythms. Rather surprisingly, while searching other subjects, I was led to very interesting research on bone strength and circadian rhythms. Most noteworthy, I learned that light entering the eye transmits to a brain area called the superchiasmatic nucleus (SCN). The retina transports light information to the SCN, which synchronizes it, and puts out signals to other tissue including bone. Output signals of SCN regulate bone metabolism through hormones that link circadian rhythms and bone.
The importance of ghrelin, a protein that associates with circadian rhythms and bone strength.
Another interesting finding is that a peptide called ghrelin promotes proliferation and prevents apoptosis (cell death) of osteoblasts. Ghrelin is sensitive to circadian rhythms. This is important to maintaining and building strong bones.
There is much more information in this paper that delves into the intricacies of bone metabolism, circadian rhythms, and light. Suffice it to say that sunlight is essential to a properly set circadian rhythm, which in turn is essential to bone strength. This may be the reason that one of the most persuasive studies on fractures showed that women in Spain—those who regularly enjoyed sun exposure—had about one-eleventh the risk of hip fractures as women who had little exposure.
For more information on sunlight and health, visit sunlightinstitute.org and read the book Embrace the Sun.
HAPPY SUNNING!
Sunscreen chemicals strike again. This time it is breast cancer. By Marc Sorenson, EdD.
Sunscreen chemicals may be some of our most debilitating environmental poisons.
Due to the worries regarding potentially deadly sunscreen chemicals, researchers are beginning to reassess the wisdom of using them.
Oxybenzone is one of the most widely used sunscreen chemicals and probably the most dangerous. Thus, we will present a few facts about the effects of Oxybenzone:
- First of all, research more than two decades old shows Oxybenzone is absorbed systemically after skin application. That evidence continues to accumulate, yet not all researchers agree that high systemic absorption of noxious chemicals is dangerous.
- Oxybenzone and other sunscreen chemicals are endocrine disruptors. Hence, they may have deleterious effects on the breast, prostate and other endocrine glands.
- These chemicals increase the production of deadly free radicals in the skin. Free radicals are associated with tissue and DNA damage and thought to be precursors to cancer.
- Sunscreen chemicals are agonists, which are substances capable of eliciting a response in hormonally regulated processes. Mammary gland development and cancer initiation are examples of responses to agonists.
- Sunscreen chemicals may lead to sunburns.
- These chemicals harm coral reefs.
- Since 1935, outdoor work has decreased profoundly (about 90%). In addition, sunscreen use has increased profoundly, and melanoma incidence has increased by about 3,000%. Seems like there is a disconnect here, no? [Read my book, Embrace the Sun, for the analysis.]
The latest, most noteworthy and alarming research on sunscreens.
Sunscreen chemicals, according to the propaganda, should prevent melanoma yet paradoxically, they do not. In addition, they should stop sunburns, yet, they do not. Another dilemma for sunscreen promoters is evidence that sunscreen toxicity is more than skin deep. Could sunscreen chemicals also promote initiation and growth of breast cancer? Endocrine-disrupting chemicals like oxybenzone and others are agonists for hormone sensitive cancers such as breast cancer. Consequently, researchers performed enlightening research to determine the relationship between breast cancer and oxybenzone. The investigation measured urine concentrations of oxybenzone in rodents on high-fat or low-fat diets exposed to that chemical.
The connection of oxybenzone and breast cancer
Results: “Benzophenone-3 exposure to mice [on high-fat diets] yielded urine levels similar to humans subjected to heavy topical sunscreen exposure.” The high-fat diet with oxybenzone promoted increased tumor cell proliferation, decreased tumor cell apoptosis [cancer-cell death], and increased tumor vascularity. In other words, it promoted growth and development of breast cancer.
The animals on a lifetime low-fat diet appeared to receive some protection with oxybenzone. Nevertheless, the researchers made the following statement: “Although benzophenone-3 [oxybenzone] seemed protective on low-fat diet, spindle cell tumors arising in these mice showed increased proliferation growth and decreased apoptosis.” My opinion is that this would predict increased potential for breast cancer and other cancers in the future.
Nearly all humans in this day are consuming high-fat diets. For those who are consuming low-fat diets, it would still be wise to avoid sunscreens.
For more information on sunlight and health, visit sunlightinstitute.org and read the book, Embrace the Sun.
Be sure to get your share of safe, non-burning sun exposure.
HAPPY SUNNING!
Sunlight and pandemics-more interesting information about our magnificent Sun, by Marc Sorenson, EdD.
Sunlight and pandemics link together closely—more sunlight, fewer pandemics. This is because it is our “best disinfectant.” Unobstructed sunlight kills viruses and bacteria outside the body and strengthens the body internally. Sunlight has been preventing diseases throughout history. That is probably why the sun was a deity in some ancient societies. More recently, scientists have been telling us for decades how important sun exposure is, and they continue to do so.
Perhaps it is time to listen!
Thus, research early in 2020, from the DHS, showed that “simulated sunlight” rapidly decayed the Covid-19 virus. The researchers tested effects of sunlight on Covid-19 viruses in aerosols—suspensions of solid particles and liquid droplets in air. These aerosols are a potential route of disease transmission through inhalation. Consequently, when sunlight exposure accelerates the decay of these viruses, it prevents an avenue of human-to-human transmission. Thus, the breathing in of these “decayed” viruses, usually coughed, sneezed, or exhaled, ceases to be lethal. Therefore, sunlight outside the body inactivates the viruses due to rapid decay. In other words, it kills them before they can do damage.
Sunlight and pandemics also link internally through vitamin D production.
Vitamin D, produced by skin during sun exposure, also inhibits some of the powerful disease reactions and makes pandemics less deadly. The cytokine storm is one of those reactions. It may lead to death by causing inflammation and subsequent pneumonia. A cytokine is a specialized protein molecule that attacks and destroys infected tissue. These proteins can be either pro-inflammatory of anti-inflammatory. For our purposes, we will discuss pro-inflammatory cytokines.
How does the cytokine storm work?
Usually, the cytokines needed to fight the infected tissue, cease their attacks and diminish after they have won the battle. However, in the case of a disease like influenza (or Covid-19), “friendly fire” occurs. The immune system recruits millions of reinforcing cytokines, and those cytokines mount an overwhelming attack against tissue they initially protected. In other words, they cause a violent storm. Cytokine storms lead to severe inflammation that weakens or destroys blood vessel membranes in the lungs and other tissue. As a result, fluid seeps through to the air sacs, which leads to pneumonia. People thus end up drowning in their own body fluids. Dr. Angela Rasmussen describes it: “Basically you’re bleeding out of your blood vessels.” She goes on to say the problem may not end there. The storm spills into the circulatory system and can create systemic issues across multiple organs.
How does vitamin D dampen the storm?
Vitamin D leads to the production of cathelicidins and defensins, which are peptides (proteins) with antimicrobial properties. According to Dr. William Grant and colleagues, these peptides lower viral replication rates and reduce concentrations of pro-inflammatory cytokines. As already mentioned, these pro-inflammatory cytokines produce the inflammation that injures the lungs. Nevertheless, the damage does not necessarily end in the lungs. Recent research shows that the damage from Covid-19 can spread to multiple organ systems.. The report on this research suggests the cytokine storm may be responsible for that spread. The heart, liver, kidneys, neurological system and gastrointestinal tract may all be targets of Covid-19.
If what I posit is true, we would expect Covid-19 to be higher in populations with high vitamin D deficiency, and such is the case.
Henry Lahore, one of the great vitamin D scholars, has listed four racial groups with disproportionately high vitamin D deficiency: Elderly Italians, Spanish, Swedish Somalis and African Americans. Mr. Lahore furnishes invaluable information regarding race, vitamin D, sunlight and Covid. Many of you have read of the alarmingly high Covid-19 death rate in African Americans. From my previous research, I know that African Americans also have alarmingly low vitamin D levels. Lahore also cites research that shows 84% of African Americans are vitamin D deficient. In addition, in Chicago, 70% of Covid 19 deaths are among Blacks. The reason for the deficiency? Dark skins take much more time in the sun to produce vitamin D.
Unfortunately, our answer to Covid-19 has been to cocoon everyone indoors.
The lockdowns assure that no one can obtain vitamin D except by supplement. That is, unless they are fortunate enough to own sunlamps and sunbeds (tanning beds). Even more alarming is the fact that the Swedish Somali population has 40% of the deaths in Sweden. Yet, they comprise only .84% of the Swedish population. Therefore, the Dark-skinned Somalis have 4,700% greater risk of death from Covid 19! This can only be due to lack of sufficient sunlight and subsequently, low vitamin D. No such death risk exists in Africa, where sunlight is ubiquitous. Thus, the answer for all Americans is to obtain plenty of non-burning sun exposure year around, or use a sunbed.
More common sense about sunlight and pandemics from Richard Hobday, researcher and writer.
First of all, to understand this section, you must know that the flu pandemic of 1918 killed approximately 50 million people. Mr. Hobday explains this in an important paper from 2020, entitled Coronavirus and the Sun: a Lesson from the 1918 Influenza Pandemic
Here are his most impactful points regarding sunlight and the 1918 pandemic:
Medical personnel found that patients nursed outdoors recovered better than those treated indoors.
- Outdoor air is a natural disinfectant. Fresh air can kill flu viruses and other germs.
- In the 1918 pandemic, overcrowding and bad ventilation put soldiers and sailors at high risk of catching influenza.
- Most of the victims of the pandemic did not die from influenza: they died of pneumonia and other complications.
- Hospital personnel placed sick soldiers outdoors to breathe fresh air [and of course, sunlight]
- Open-air treatment reduced deaths among hospital patients from 40 percent down to about 13 per cent.
Of course, in 1918, the efficacy of sun exposure and vitamin D was unknown.
So now, we know. Low sunlight links to high pandemic risks. More sunlight and fresh air produce a better chance of surviving the pandemic we currently face.
It seems like nature knew a better way more than 100 years ago. Safely enjoy non-burning sun exposure or sunbed exposure regularly.
Happy Sunning!
To learn more about the marvelous curative powers of sunlight, visit Sunlight Institute and read the Book, Embrace the Sun.
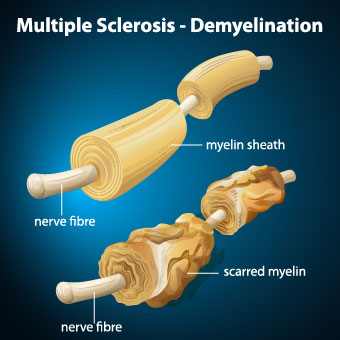
MS is associated closely with lack of sun exposure and low vitamin D levels. So what is new? By Marc Sorenson, EdD
MS is a disabling autoimmune disease.
MS is an autoimmune disease in which T-cells initiate an inflammatory response against myelin. This process, known as demyelination, leaves the nerves bare and susceptible to “short circuiting.” As a result, communications between brain and body suffer damage. Eventually, the disease causes irreparable deterioration of nerves. Some of the effects of MS include numbness and weakness in limbs. In addition, there may be lack of coordination, loss of vision, lack of mobility, slurred speech and numerous other disorders.
What do we know about the connection between sun exposure and MS?
Sunlight is an immunomodulator. In other words, it may affect the functions of the immune system. In the case of an autoimmune disease, it may stop the immune system’s attack on its own tissue. Because sunlight stimulates the production of vitamin D in skin, it may suggest that vitamin D is protective. In addition, it also suggests the incidence should diminish in areas of high sun exposure, and increases in areas of low exposure.
Thus, the risk of MS in far northern areas is 100 times greater than in equatorial areas.
In equatorial areas, sunlight is intense, and the risk of the disease approaches zero. Another interesting study of immigrants to the UK (low sunlight), but born in the sunny West Indies is enlightening. Especially relevant is that these immigrants had one-eighth the rate of MS as their own children born in the UK. It therefore appears that childhood sun exposure provides protection against the disease.
Where does vitamin D fit?
While it is tempting to chalk up the association of low MS to high vitamin D (as mentioned above), use caution. As with certain other diseases, sun exposure may have a positive influence on MS, independent of vitamin D. For example, a study on animals assessed the relative affect of sunlight and vitamin D on the diseaase. The researchers concluded, “These results suggest UVR [sun] is likely suppressing disease independent of vitamin D production.” They also stated that vitamin D supplementation alone might not replace the ability of sun (UV) to reduce MS susceptibility.
Another more recent study found similar results.
The investigators used animals that had no vitamin D receptors (VDR), and therefore could not produce vitamin D. Therapy with UV light suppressed the disease. The investigators concluded that UV light suppression of MS occurs in the absence of vitamin D production.
Another recent investigation: High sun exposure and high vitamin D both associate with lessened severity of MS.
This study investigated the severity of the disease among people who already had MS. Thus, it was a unique study, to my knowledge. The investigators used the subjects’ latitude (a marker for sun exposure and vitamin D levels) and compared it to MS severity. Interestingly, high sun exposure and high vitamin D levels associated to a reduction in MS severity. However, the investigators listed only sunlight as a sure factor in reducing MS severity.
Hence, the investigators stated three salient points in their paper.
- “Observational studies suggested vitamin D-dependent effects, but prospective supplementation studies have so far been inconclusive….”
[This is an important, and a wake up call. Those who believe that we need only swallow a handful of pills, as we avoid the sun, are sadly mistaken. There is no way we can determine if high vitamin D blood levels are the reason for a reduction in MS severity. That is, unless we produce those levels in a scientific, controlled study using supplementation.]
- “Although [low] vitamin D cannot be proven as the causal factor, we provide evidence for clinically relevant effects of sunlight exposure.
- ”Furthermore, this study suggests sunlight triggered pathways other than vitamin D could play additional and modulatory roles as well.”
There you have it.
High sunlight exposure decreases the severity of multiple sclerosis. Vitamin D, though it is a miraculous nutrient, probably has little or no effect on the disease.
HAPPY SUNNING!
 You can find much more information on sun exposure and MS at sunlightinstitute.org. Also, read the book, Embrace the Sun.
You can find much more information on sun exposure and MS at sunlightinstitute.org. Also, read the book, Embrace the Sun.
Fishermen receive skin protection through sun exposure and vitamin D, by Marc Sorenson, EdD.
Fishermen in Brazil spend plenty of time on the sea and have healthy skin. Furthermore, they soak up vast quantities of direct sun exposure. Thus, should we expect them to succumb to incredibly high rates of skin cancer? No! Does this seem like a paradox? It should not. It is the perfectly natural outcome of plenty of non-burning sun exposure. This will seem clear to you if you have read my book, Embrace the Sun.
Recent research from Brazil produced some large and fascinating surprises. In addition, it changed a few minds regarding knowledge of sunlight’s healthful qualities. First of all, it illuminated sunlight’s protective effects against skin cancer, particularly in fishermen.
So how much sunlight do fishermen in Brazil soak up daily?
Due to their profession, commercial fishermen chronically expose themselves to sunlight. So, in this research, they had soaked up Brazilian sunlight for more than 15 years. The average exposure time was 21 to 28 hours weekly! Consequently, these fishermen received a sunlight dose 6-8 times higher than indoor workers did. Therefore, you might surmise that they used lots of sunscreen. Yet they did not. It is especially relevant that 62% of this population of fishermen used none. Must we therefore conclude that they suffered exceptionally high skin cancer risk? No. The frequency of skin-cancer diagnoses was 2.7% of the study population of 174 fishermen (and fisher women). The researchers stated, “There was a low prevalence of diagnosed skin cancer among the fishermen when compared to the general population.”
So there you have it. The general population, with comparatively little sun exposure, suffers from a high skin cancer risk.
Yet, fishermen practically bake in the sun every day, and have a minuscule risk of skin cancer. This paradox should be easily understood. Sun exposure is a superb prophylactic against skin cancer and most other cancers if used regularly and safely without burning. Remember that it causes the body to produce vitamin D, which may also provide protection against skin cancer.
For more information on sunlight and health, visit sunlightinstitute.org and read the book, Embrace the Sun.
HAPPY SUNNING!
More sunlight, less covid 19 by Marc Sorenson, EdD.
More sunlight, I said at the onset of Covid-19 (also known as SARS-Cov-2), would be associated with a reduced incidence disease and death. In addition, I stated the disease would make a remarkable resurgence in fall and winter, as availability of sunlight diminished. For that statement, some praised my perspicacity, and others derided my intelligence. I lost some friends on social media and had to unfriend others.
For our purposes, it is important to understand that there are several coronaviruses, and each causes its particular disease manifestation.
In addition, with the possible exception of Covid-19, these viruses are seasonal. Thus, the incidence rates are higher in winter and lower in summer. Could sunlight exposure be the key to the seasonal relationship? Especially relevant, of course, is that Covid-19 was non-existent at the time the other viruses proved their seasonality. It now appears, however, that Covid-19 is indeed seasonal. Thus, I believe that sunlight drives that seasonality.
So what do we to obtain more sunlight now that winter has arrived?
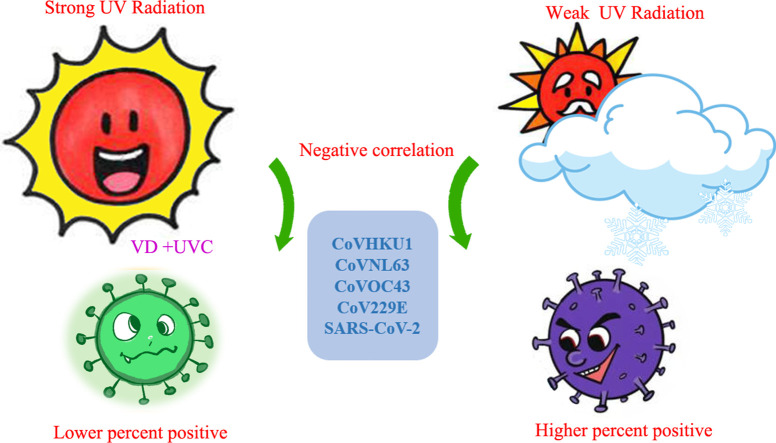
I suppose it is self-serving to say, “I told you so.” Yet indeed, I did make my prediction, and it was correct. It would have been even more correct if people were encouraged to seek the sun rather than suffer through sunless lockdowns. There is now scientific corroboration that more sunlight associates with less death and disease from Covid-19 and other coronaviruses. Recent research (already dated for 2021), substantiates my ideas on sunlight and Covid-19. In this study, the investigators assessed sunlight available from April 17-July 20, 2020 in various U.S. geographical zones. Then, they compared sunlight availability to the risk of Covid-19 and four other coronaviruses in different areas of the U.S. The graphical abstract they presented is below and makes the same point that I made months ago.
In areas of strong UV radiation (more sunlight), there was much less risk of testing positive for Covid-19 and the other coronaviruses.
Obviously, people need more sunlight to help protect themselves from Covid-19 and other viruses. Obtaining more sunlight works in at least two ways against Covid-19.
1. Research from the CDC shows that sunlight rapidly kills Covid-19 in aerosols.
Aerosols are suspensions of solid particles or liquid droplets in air. They are potential routes for disease transmission. Sunlight is also able to kill Covid-19 on surfaces.
2. More sunlight exposure causes the skin to produce more vitamin D
. Vitamin D inhibits the overproduction of cytokines, specialized protein molecules that attack and destroy infections. Usually, the cytokine needed to fight the infected tissue stops its attack after it has won the battle. However, in the case of a disease like influenza (or Covid-19), “friendly fire” occurs. The body’s immune system recruits innumerable “extra” or reinforcing cytokines, and those cytokines mount an overwhelming attack against the tissue they initially protected; in other words, they cause a cytokine storm.
Cytokine storms lead to severe inflammation that weakens or destroys blood vessel membranes in the lungs.
This causes fluid to seep through to the air sacs, which leads to pneumonia. A person then ends up drowning in his/her own body fluids. Dr. Angela Rasmussen describes it thus: “Basically you’re bleeding out of your blood vessels.” She goes on to say that the problem may not end there. The storm spills into the circulatory system and can create systemic issues across multiple organs.
Vitamin D, through various mechanisms, retards and stops cytokine storms.
Thus, sun exposure is a two-edged sword: (1) it kills Covid-19 outside the body. (2) It causes the production of vitamin D and can stop the cytokine storm.
So in winter, when there is little sunlight available, and virtually no production of vitamin D, what shall we do?
When there is insufficient sunlight, it is essential to find another source of light that will also produce vitamin D. Sunbeds are the ideal source of the light we seek. Research shows that sunbed users (tanning bed users) in Canada and the U.S. have higher vitamin D levels than any other demographic.
I own a sunbed and go to salons when traveling. This winter, I plan to use my sunbed regularly. In my opinion, it is the best protection against the sunlight deficiency experienced in winter.
For more information on the healthful benefits of sunlight, visit https://sunlightinstitute.org/ and read the book, Embrace the Sun.
Happy sunning!
Memory, learning and sunlight by Marc Sorenson, Ed.D
Memory becomes a worry as humans age, and that worry has spawned a plethora of new anti-forgetfulness products. Based on recent research, we elucidate the manner in which sunlight stimulation of skin may influence important chemical reactions. These reactions improve memory and cognition.
For the purpose of this article, it is necessary to understand the meaning of three terms:
- Urocanic acid (UCA): a crystalline acid normally present in human skin, it may play a part in skin protection.
- Histidine: a basic amino acid that acts as an intermediary between UCA and glutamate
- Glutamate: a chemical that functions as a neurotransmitter and excites cells of the central nervous system
You are probably already forming your own opinion regarding the interaction of sunlight and memory. Let us expatiate on that interaction and unravel a hitherto unknown mystery.
The authors of the aforementioned research noted that seasons of sunlight associated with moderate improvement to physical and mental states. Some conditions you may be familiar with, because we have discussed them at length in these blogs. A few of them are seasonal affective disorder (SAD), bipolar disorder, and depression. Nevertheless, what makes the research so interesting is that it sought answers regarding why sunlight seemed to enhance learning and memory. Moreover, it found a brand new answer.
Because the researchers explored brain neurons to unlock the mystery, they found that UCA existed in many brain regions. This was not something that they had encountered previously, and thus it piqued their curiosity. No other investigators had reported finding UCA in the central nervous system. Yet, they knew UCA was prevalent in skin. Therefore, knowing that sun exposure to the skin produced many photoproducts, they tested a new hypothesis. That hypothesis was that UCA produced by sunlight could be the link that ties sunlight to memory.
How the researchers conducted the experiment
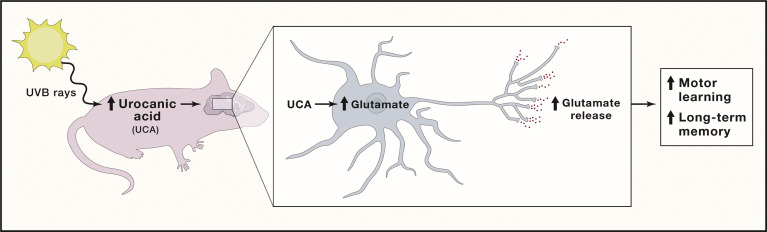
After exposing rats to low-dose UVB exposure (similar to sunlight or sunbed exposure), they observed increased UCA levels in the serum. Moreover, they observed the same increase in UCA levels within the neurons (nerve cells) of the cerebrospinal fluid. Furthermore, they were able to produce the same increases in UCA brain levels by intravenous injection of UCA. This suggests that UCA may cross the blood/brain barrier and enter brain neurons. The authors of the above-cited research stated that UCA is an intermediate part of a conversion of histidine to glutamate. The following graph describes the sunlight>UCA>glutamine>memory connection. (from the authors)
Glutamate, as mentioned, excites neurons in the brain. What better way to improve memory?
To test their hypothesis with “mouse memory,” the investigators assessed the ability of the animals to stay on a moving device called a rotarod. In addition, they observed that administration of both UCA and UV exposure enhanced the performance of the animals.
The bottom line regarding sunlight and brain function
Sun exposure improves memory, and UCA (with glutamate) appears to be one of the mechanisms responsible for that improvement.
Happy sunning!
For more information on the health benefits of sunlight, visit the Sunlight Institute and read the book, Embrace the Sun.
Latitude, sunlight, and covid-19 by Marc Sorenson, EdD
Latitude, when compared to disease and disability, is an attention catcher. First of all, why would latitude be important? Is it because latitude itself creates disease? Is it because different latitudes lead to different temperatures? Could it be different distances from the magnetic poles are involved in human physiology? No, none of those answers is correct, yet, there is a simple answer to the link between latitude and disease. That answer is sunlight and vitamin D. Low latitudes (closer to the equator) receive much more sunlight, and sunlight is more direct much of the year.
A study of latitude backs the efficacy of sunlight, and possibly vitamin D, on reducing the risk of Covid-19. This was a large, study, drawing reliable data from 88 countries. The researchers compared the countries for Covid-19 death rates and then compared them for the latitude.
The results of Covid-19 death rates compared to latitude.
Highly significant, positive correlations were found between lower mortality rates from Covid-19 and a country’s proximity to the equator. The researchers stated that their evidence suggested a direct correlation between sun exposure and reduced mortality. They also assumed that vitamin D was the photoproduct of sunlight that lowered the risk of Covid-19.
This was a good, timely study in that it established sunlight as a prophylactic for covid-19. Many studies had previously mentioned vitamin D as the primary blood measure to reduce risk of the Covid-19, but none has mentioned latitude as a factor to furnish proof. In addition, neither does this study really furnish proof. That is because the only study that will prove the relationship would be a vitamin D-supplement study.
Other research,which links vitamin D levels to reduced Covid-19 mortality, but does not mention latitude as a factor.
Another recent study on the association of vitamin D levels to covid-19 survival shows promise for vitamin D. It states that fourteen observational studies show that high D levels inversely correlate with the incidence or severity of Covid-19. Yet, we should always remember that sun exposure on skin produces 90% of the vitamin D levels in most populations. Furthermore, 20 minutes of full-body summer sun exposure at midday produces up to 20,000 IU of vitamin D.
Finally, a word about sunbeds (tanning beds)
Finally, realize that sunbeds (tanning beds) produce vitamin D and enhance health. In addition, it is likely they would also reduce Covid-19. Sunbeds produce vast quantities of vitamin D. People in Canada who use sunbeds have the highest levels of vitamin D in the country, especially in winter. Moreover, a 20-year study demonstrated that both sun exposure and sunbed exposure reduced the risk of death. Women who used sunbeds were 23% less likely to die from any cause than women who did not use them. Another advantage is that latitude does not matter with sunbed use.
From the available research, it is evident that sunlight and vitamin D are protective against Covid-19. Sunlight exposure at midday, or sunbed use, are always the best sources, since sunlight exposure produces many health benefits beyond vitamin D.
For more information on the benefits of sunlight, visit Sunlight Institute, and read Dr. Marc Sorenson’s book, Embrace the Sun.
Vitamin B3, other lifestyle factors and skin cancer, by Marc Sorenson, EdD
Vitamin B3 is not a topic I expected to find while checking out the latest on nutrition and skin cancer. Consequently, it surprised me that research showed an impressive effect of vitamin B3 on protection against non-melanoma skin cancers (NMSC). NMSC are also known as squamous and basal cell carcinomas (SCC and BCC). The protection occurs against UV (ultraviolet) light, which researchers claim is the prime factor causing squamous and basal cell cancers. In the aforementioned study, treatment with vitamin B3, 24 hours before exposure of skin to UV, reduced oxidative stress significantly. It also had the ability to repair DNA damage. This is another study demonstrating that sunlight is not the enemy. Rather, NMSC is due to a combination of factors, including environmental toxins, poor habits of hygiene, smoking, and poor nutrition.
When the skin lacks protection, which is too often the case, then excessive sun exposure can cause damage and pain.
However, that is not what happens in a well-adjusted and well-cared-for life. Protection, whether by vitamin B3 or other additional healthful factors, can stop the damage. This may render sun exposure one of God’s greatest gifts to human health and wellbeing. Sun exposure is really only a minor factor in NMSC.
Here are factors beyond sunlight (and vitamin B3) that make a difference in this skin cancer:
Smoking predicts a higher risk of squamous cell carcinoma (SCC). After adjustment for sun exposure, age and sex, smoking predicts a doubling of the risk for SCC. In addition, there is a dose/response relationship between the number of cigarettes smoked and the risk of SCC. Such a relationship also exists among those whose diets lack green, leafy vegetables and whose consumption of meat and fat are very high. Vitamin B3 could be a nutritional factor related to low vegetable consumption and high meat and fat consumption.
Obesity is also an important risk factor for NMSC.
One study suggests that being obese changes the tumor microenvironment, due to the chronic inflammatory state that generally accompanies obesity. Furthermore, Cancer mortality maps also indicate that NMSC mortality is highest in regions with the highest obesity (https://www.cdc.gov/obesity/data/prevalence-maps.html). However, this is not true of regions with the highest sunlight exposure.
The message:
Lack of Vitamin B3 is a factor for an increased number of NMSC and probably for other cancers. Yet, it is only one of many factors that protect the skin. When poor nutrition and other deleterious lifestyle habits disappear, the risk of NMSC decreases. Let us not blame the sun! 
Happy sunning!
For more information on sunlight and health, visit sunlightinstitute.org and read the book, Embrace the Sun.
IQ, vitamin D and sunlight by Marc Sorenson, Ed.D
IQ and vitamin D levels piqued my interest many years ago. This was because research had demonstrated that animals with low vitamin D levels had poorer neurocognitive function. For example, rats born to vitamin D-deficient mothers have profoundly altered brains at birth. The cortex is longer, the lateral ventricles enlarged the cortex thinner, and there is more cell proliferation. Furthermore, there are also reductions in brain content of nerve growth factor. In addition, similar results manifested themselves with older rats born to vitamin D-deficient mothers.
Other research indicates IQ, vitamin D and sunlight have a connection to cognitive function:
Here are more reasons to believe brain and cognitive function associate closely with IQ, as well as vitamin D and sunlight. The book Embrace the Sun. covers the following facts thoroughly:
- Alzheimer’s disease (AD) and non-Alzheimer’s dementia associate with low vitamin D levels and insufficient sun exposure.
- Autism associates with low vitamin D levels. Bipolar disorder associates with both sun exposure and low vitamin D levels.
- In addition, a study of cognitive abilities as they relate to vitamin D levels shows a considerable difference in vitamin D deficient people. Thus, persons with lowest levels are twice as likely cognitively impaired compared to those with highest levels. Remember that sun exposure raises and optimizes vitamin D levels.
- Another study showed twice as many patients with intellectual disabilities showed D deficiency when compared to normal controls.
Back to IQ
Despite the aforementioned facts and research, I had never seen research that associated IQ in humans to sunlight. Consequently, I searched the literature for years, and have now found my research. A most interesting article on IQ, vitamin D and sunlight recently appeared in the Journal of Nutrition. In this study, the researchers assessed pregnant women for vitamin D levels and then assessed their subsequent offspring for IQ.
The researchers assessed these women’s vitamin D levels in the second trimester of pregnancy.
Offspring of women with low vitamin D levels had lower IQs at the age of 4-6 years. The researchers concluded thusly: “Second-trimester maternal vitamin D positively associated with IQ at 4–6 y, suggesting that gestational vitamin D status may be an important predictor of neurocognitive development. These findings may help inform prenatal nutrition recommendations and may be especially relevant for Black and other dark-skinned women at high risk of vitamin D deficiency.
The bottom line regarding IQ.
Pregnant mothers need to optimize their vitamin D levels, preferably by sun exposure to the skin. It will ensure that both they and their offspring will be healthier and smarter. This is vitally important to black women and other women of color, who have large quantities of skin melanin. This inhibits vitamin D production and may be dangerous for their offspring. IQ, vitamin D and sunlight are important to well-being and happiness. Nevertheless, the researchers observed no IQ differences based on race, but only on vitamin D Levels.
For more information on the health benefits of sunlight and vitamin D, visit Sunlight Institute and read the book, Embrace the Sun. 
Happy sunning!