What do you know about melanoma?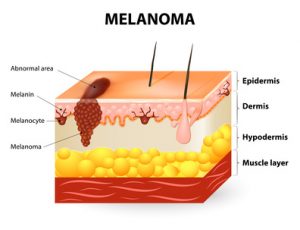
May is Melanoma Awareness Month, Therefore, we will discuss some truths to be aware of:
- First of all, seventy-five percent of these cancers occur on areas of the body that are seldom or never exposed to sunlight.[1] For example, research has shown that melanomas in women occur primarily on the upper legs, and in men more frequently on the back—areas of little sun exposure.
- Most noteworthy, in the U.S., sun exposure has decreased by about 90% since 1935. In the same time, melanoma incidence has increased by 3,000%! [2] [3] [4]
Dr. Diane Godar furnishes this exceptionally important melanoma information:[5]
- The same as in the US, while sun exposure in Europe has profoundly decreased, there has been a spectacular increase in the disease.
- Men who work outdoors have about half the risk as men who work indoors. Hence, sun exposure could not be the cause.
- in addition, outdoor workers, while receiving 3-9 times the sun exposure as indoor workers, have had no increase in melanoma since before 1940, whereas the incidence in indoor workers has increased steadily and exponentially.
- Especially relevant is that sunscreen invention, along with its steadily increasing use, has not reduced the risk of melanoma. Rather, the disease has increased as sunscreen use has increased.
- Increasing melanoma incidence significantly correlates with decreasing personal annual sunlight exposure.
- Also, outdoor workers get many sunburns but still have dramatically lower risk of contracting the disease.
So, since melanoma increases as sun exposure decreases, should we continue to blame the sun?
Here are more facts you should know about the causes of melanoma:
- First of all, people in the highest quintile (fifth) of alcohol consumption have a 65% increase in risk.[6]
- Weekly meat consumption increases the risk of melanoma by 84% and daily fruit consumption reduces the risk by nearly 50%.[7]
- Furthermore, those with the highest levels of blood PCBs have 7-times the risk compared to those with the lowest levels.[8]
- Recent use of Viagra is associated with an 84% increase in risk, and long-term use of the drug is associated with a 92% risk increase.[9]
- Finally, there is a positive association between melanoma and obesity.[10]
Furthermore, Dr. Adele Green found that the strongest risk factor for both limb and trunk melanoma was moles. The presence of more than 10 moles on the arm predicted a 42-times increased risk.[11]
Therefore, please stop blaming the sun. Safely embrace the non-burning sun and reduce your risk of melanoma.
References:
[1] Crombie IK. Distribution of malignant melanoma on the body surface.Br J Cancer. 1981 Jun;43(6):842-9.
[2] Melanoma International Foundation, 2007 Facts about melanoma. Sources: National Cancer Institute 2007 SEER Database, American Cancer Society’s 2007 Facts and Figures, The Skin Cancer Foundation, The American Academy of Dermatology.
[3] Ian D. Wyatt and Daniel E. Hecker. Occupational changes in the 20th century. Monthly Labor Review, 2006 pp 35-57: Office of Occupational Statistics and Employment Projections, Bureau of Labor Statistics.
[4] US Congress, Office of Technology Assessment, Catching Our Breath: Next Steps for Reducing Urban Ozone, OTA-O-412 (Washington, DC: US Government Printing Office, July 1989).
[5] Stephen J Merrill, Samira Ashrafi, Madhan Subramanian & Dianne E Godar. Exponentially increasing incidences of cutaneous malignant melanoma in Europe correlate with low personal annual UV doses and suggests 2 major risk Factors. Dermato-endocrinology 2015;7:1
[6] Millen AE, Tucker MA, Hartge P, Halpern A, Elder DE, Guerry D 4th, Holly EA, Sagebiel RW, Potischman N. Diet and melanoma in a case-control study. Cancer Epidemiol Biomarkers Prev. 2004 Jun;13(6):1042-51.
[7] Gould Rothberg BE, Bulloch KJ, Fine JA, Barnhill RL, Berwick M. Red meat and fruit intake is prognostic among patients with localized cutaneous melanomas more than 1 mm thick. Cancer Epidemiol. 2014 Oct;38(5):599-607.
[8] Gallagher RP, Macarthur AC, Lee TK, Weber JP, Leblanc A, Mark Elwood J, Borugian M, Abanto Z, Spinelli JJ. Plasma levels of polychlorinated biphenyls and risk of cutaneous malignant melanoma: a preliminary study. Int J Cancer. 2011 15;128(8):1872-80.
[9] Li WQ, Qureshi AA, Robinson K, Han J. Sildenafil use and increased risk of incident melanoma in US men: a prospective cohort study. JAMA Intern Med. 2014 Jun;174(6):964-70C
[10] Karimi K, Lindgren TH, Koch CA, Brodell RT. Obesity as a risk factor for malignant melanoma and non-melanoma skin cancer. Rev Endocr Metab Disord. 2016 Sep;17(3):389-403.
[11] Green AC, Siskind V. Risk factors for limb melanomas compared with trunk melanomas in Queensland. Melanoma Res. 2012 ;22(1):86-91.
