Bone, vitamin D supplements, and sunlight By Marc Sorenson, EdD.
Bone and vitamin D are connected, yet, it may not be in the way you think. It is probably common knowledge that vitamin D is necessary for bone strength, particularly rickets. Yet, beyond rickets, it is not settled science that supplements significantly improve bone strength.
To prove this point, and to cause thoughtful consideration, I call your attention to a meta-analysis of 23 studies. The research assessed change in bone density (BD) from measurement inception to completion of each experiment. The bone densities measured the lumbar spine, femoral neck, total hip, trochanter, total body, or forearm. In addition, all participants took vitamin D supplements. There was little observable change in BD, so the results were disappointing. Thus, the researchers reported, in conclusion, “Continuing widespread use of vitamin D for osteoporosis prevention in community-dwelling adults without specific risk factors for vitamin D deficiency seems to be inappropriate.” Yet, before you give up on vitamin D for bone, let us consider the weakness of the research.
Does bone require much more than 800 IU per day to increase bone strength?
In 10 of the 23 studies cited above, the vitamin D dosage was less than 800 IU per day. This is rather like throwing a packet of food coloring into the sea and expecting the sea to turn red. Direct full-body sunlight during 10-15 minutes can stimulate the skin to produce up to 20,000 IU of vitamin D. Sunlight is the natural way to obtain vitamin D and numerous other healthful photoproducts. A minuscule dose of 800 IU will probably do little for bone strength. Yet, if the researchers had found studies using 3,000 and 5,000 IU, I could have more easily believed their conclusions. However, I could easily have been wrong, as you will see.
So are there other studies that make contradictory conclusions?
No. Most of the research using high-dose vitamin D supplements also had poor results. They usually resulted in much higher fracture risk for those taking the supplements. This was especially true in those who took large, intermittent doses and or intermittent intramuscular injections. Other data showed that doses of more than 4,000 IU daily are associated with more falls and fractures. In addition, research from the Journal of the American Medical Association showed an alarming trend. First of all, treatment with vitamin D for 3 years (4000 IU) day was counterproductive. Thus, it resulted in statistically significant lower bone mineral density (BMD) in certain bones. Furthermore, the same was true for 10,000 IU per day.
Are there better ways to keep bone strong?
Another factor to consider: vitamin D supplements may not be the same as vitamin D made by the human body. The skin always makes natural vitamin D for humans during exposure to sunlight and other sources of UVB light. Irradiating sheep’s lanolin produces the Vitamin D for supplements. Therefore, although 20,000 IU of vitamin D in 20 minutes is possible from sun exposure, the results are very different. Skin-produced vitamin D from sun exposure does not result in increased fracture risk and lower BMD.
The Spanish study on bone and sunlight
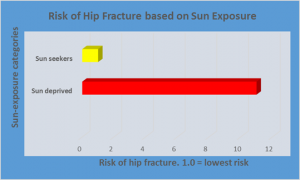
An important study from Spain shows that those who actively sought sun exposure had only 1/11 the risk of hip fracture compared to those who were not sun seekers! In this case, the sun-seeking people must have produced remarkable quantities of vitamin D. They also they increased bone strength remarkably. In addition, we know that the high vitamin D levels certainly caused no problem with bone density and bone strength! How can this be if high doses of vitamin D supplements lead to increased fracture rates? The difference, in my opinion, is the source.
Lessons learned, and conclusions
Therefore, we may take away important lessons from this treatise. First, vitamin D produced by sunlight is not the same as vitamin D from a pill. Moreover, vitamin D is a primary photoproduct of sun exposure. There is an exceptional difference between a pill produced from lanolin and a photoproduct produced in response to sunlight. If sun exposure can produce up to 20,000 IU of vitamin D, and it increases bone strength, something is awry with vitamin supplements, which decrease bone strength. We have produced evidence that show vitamin D supplements may increase bone fragility. It is time to accept the sun or other source of light as the major source of bone strength. That other source could be sunlamps or tanning beds.
A synopsis on bone and sunlight.
Finally, we must realize that sun exposure produces many photoproducts beyond vitamin D. Serotonin, endorphin, nitric oxide; brain-derived-neurotropic factor (BDNF) and dopamine are some of those photoproducts. All of them are vital to human health. Who is to say that these photoproducts do not form a synergistic relationship with sun-produced vitamin D to create the miracle of hip-fracture reduction? Do not neglect your regular, non-burning sun exposure. It may save your bones and your life.
Read more by visiting the Sunlight Institute, and read the book by Sorenson and Grant, Embrace the Sun. Happy Sunning!
UV index. Vita min D and health. By Marc Sorenson, EdD
min D and health. By Marc Sorenson, EdD
The UV index is a measure of the intensity of ultraviolet radiation B (UVB) from the sun. It is expressed as a number on a scale of 0-11. A higher number indicates a higher sunlight intensity. Exposure to the ultraviolet B (UVB) portion of sunlight is necessary to cause the skin to produce vitamin D. Nevertheless, unless the body is deeply tanned or naturally very dark, a very high UV index can cause sunburn, so caution is necessary.
A low UV index is also problematic.
However, if the UV index is very low, it cannot stimulate the production of vitamin D in the skin. Vitamin D production is essential for human health. Thus, lack of vitamin D may be a major reason that flu-like diseases occur primarily during winter, when there is little or no vitamin D production. This, of course varies according to latitude.
A List of vitamin D benefits from Business Insider.
A recent article from Business Insider (a Philippines online paper) discussed various health effects of vitamin D and sun exposure. Here are some of their salient points, not all of which are correct.
- The primary cause of vitamin D deficiency is sun deprivation (correct).
- Vitamin D helps keep the immune system, so deficiency could be the reason for frequent flu (correct).
- You can get more vitamin D by spending at least 5 to 10 minutes outside 3 times a week without sunscreen (correct).
How much vitamin D does a person need?
- The most incorrect statement of the article is this. The average adult needs around 600 international units (IU) of vitamin D a day (not correct). For reference, a serving of salmon contains roughly 400 IU (not correct). 20 minutes of full-body, unobstructed sunlight can cause the skin to produce up to 20,000 IU of vitamin D. If 600 IU were the only source of vitamin D, one would produce a level of six ng/ml, which would be woefully inadequate. 600 IU is only slightly better than nothing.
- Fifteen minutes of non-burning midday sun (without sunscreen) would optimize vitamin D levels in a few days. Dark-skinned individuals would need much more exposure, up to an hour.
-
Getting more frequent colds or respiratory infections could be a symptom of vitamin D deficiency (correct). However, it is even more likely to be a sign of sunlight deprivation.
- Colds and flu nearly disappear in the summer when the sun is direct. During this time of the coronavirus epidemic, everyone on earth needs daily direct or indirect sun exposure. Those who do not tan can obtain plenty of sunlight from being outdoors under an umbrella or even in the shade near where the sun is shining.
-
Bone diseases, vitamin D and sunlight.
- Vitamin D deficiency can cause Osteomalacia and Osteoporosis, conditions where your bones become less dense (correct). Sun exposure produces about 90% of the body’s serum levels of vitamin D. In addition, not all vitamin D supplement studies have produced stronger bones.
Sunlight is king for increasing bone strength.
- However, sun exposure, or exposure to sunbeds (tanning beds) produces marvelous results. For example, a Spanish study showed that women in Spain—those who regularly enjoyed sun exposure—had about one-eleventh the risk of hip fractures as women who had little exposure. Women who use sunbeds also have profoundly higher bone mass than women who do not use them. Their vitamin D levels are also remarkably higher.
-
Mental problems due to a low UV index and subsequent vitamin D deficiency.
- Vitamin D has some links to depression (correct). Nevertheless, that link in my opinion is 100% due to to sun deprivation. Dr. Gavin Lambert and his colleagues in Australia measured serotonin levels in response to varying degrees of bright light. To do so, they drew blood samples from the internal jugular veins of 101 men and compared the serotonin concentrations of the blood to weather conditions and seasons. The results were remarkable: Men measured on a very bright day produced eight times more serotonin than those measured on a cloudy, dismal day.
More on the UV index and “solar noon.”
When meteorologists report UV index, the emphasis usually warns against the maximum UV level. That level generally occurs around “solar noon.” Solar noon is a four-hour period stretching from 10:00 AM to 2:00 PM. As you have probably noticed, forecasters constantly warn us to avoid the 10:00 to 2:00 hours. Avoiding intense UV radiation is their watchword. Many of them say, “Get sun exposure in the early morning or late afternoon to produce vitamin D.” They should know that the UV index must be over 3 to produce vitamin D.
These reporters do not understand how low UV index hinders vitamin D production.
They do not comprehend that UV index is so weak in the morning that it produces absolutely no vitamin D. The same is true in the evening. Therefore, the closer to solar noon you plan your outdoor time, the more vitamin D you will produce. Vitamin D produced in the skin from solar UVB exposure does not lead to vitamin D toxicity and is safe, as the body limits its own production.
Another method to measure the efficacy of sunlight for vitamin D is to stand in the sun at any time of day and observe your shadow. If your shadow is shorter than your height, you are producing vitamin D. This, the shorter the shadow, better.
Caveats regarding the UV index and vitamin D. Morning sun is still very healthful.
Early morning sun exposure, when the UV index is very low, (under 3) has remarkable health effects. These include resetting the circadian rhythm, increasing production of serotonin, lowering blood pressure through nitric-oxide production and assisting weight loss. Nevertheless, vitamin D stimulation in the skin is not one of the health effects of early morning light.
So safely soak up the sun at any time of day and reap the health benefits. Never burn.
Happy sunning!
For more information: http://sunlightinstitute.org/ and read the book, Embrace the Su n.
n. 
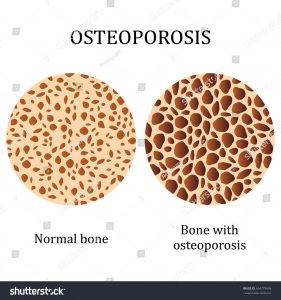 Bone needs vitamin D
Bone needs vitamin D
Bone is deteriorating in our society. Why? Since the year 2000, there has been an 8,300% increase in vitamin D deficiency in children. Insufficient time playing outdoors and/or sunscreen use are the causes of this disaster.[1] It is especially relevant to know that the skin produces vitamin D when it is touched by ultraviolet light (UV). (UV, of course, is a spectrum of sunlight, and of tanning beds and sunlamps.) And, the artificially-lighted environments that most children (and adults) live in, produce no vitamin D for bones. Vitamin D is critical for preventing osteoporosis, a fact that is most noteworthy for this discussion. Without vitamin D, weak bones develop in adults and rickets can develop in children.
Bone strength in children: Rickets is making a comeback.
Rickets is a horrible, disfiguring children’s bone disease. And, before the population became terrified of sun exposure, rickets was at one time considered to be eradicated. Hence, people are surprised to find out that the bones of children are deteriorating. Hence, rickets is making a frightening comeback,[2] it is rearing its ugly head even in sun drenched southern states. That is probably because the children are inside, avoiding the sun and concentrating on their technology. Of course, disuse of the body during this sedentary state also causes loss of calcium, thus causing weakness.
Can “sun supplementation” stop or reverse bone loss?
Therefore, the latest research on UV supplementation is exceptionally important in this world of indoor artificial light. First of all, rats exposed to long–term low-dose ultraviolet irradiation showed an increase in bone formation rate. Furthermore, there was a decrease in resorption (bone breakdown). And, there was an improvement in bone mass content and bone mineral density without any adverse effects on skin.[3] Consequently, this research shows that the concept of ultraviolet light causing skin cancer is incorrect. Also, it corroborates how effective ultraviolet light is in maintaining and increasing bone mass. For example, a Spanish study shows that women who are sun-seekers are protected from bone loss. They have only one/11 the risk of hip fracture as those who avoid the sun.[4]
Bring the UV light inside to protect bone and enhance wellbeing.
In conclusion, this research demonstrated a concept that had never occurred to me. If we can’t bring the children (or adults) out into the sunlight, perhaps we can bring the sunlight inside to them. Also, it seems like a great idea to use low-intensity ultraviolet light indoors for northern climes where sunlight is scarce in the winter. I guarantee that it will also improve moods, reduce seasonal affective disorder and otherwise enhance the health. So remember regular, non-burning sun exposure when you consider a healthful lifestyle.
[1] Basatemur E, Horsfall L, Marston L, Rait G, Sutcliffe A. Trends in the Diagnosis of Vitamin D Deficiency. Pediatrics. 2017 Mar;139(3).
[2] Weisberg P, Scanlon KS, Li R, Cogswell ME. Nutritional rickets among children in the United States: review of cases reported between 1986 and 2003. Am J Clin Nutr 2004;80(6 Suppl):1697S-705S.
[3] Guo R, Du Y, Zhang S, Liu H, Fu Y. The effects of ultraviolet supplementation to the artificial lighting on rats’ bone metabolism, bone mineral density, and skin. J Photochem Photobiol B. 2018 Aug 27;188:12-18.
[4] Larrosa M, Casado E, Gómez A, Moreno M, Berlanga E, Ramón J, Gratacós J. Vitamin D deficiency and related factors in patients with osteoporotic hip fracture. Med Clin (BARC) 2008;130:6-9.
Sun exposure and health… by Dr. Marc Sorenson, Sunlight Institute…
Lack of vitamin D, which is produced by sun exposure, leads to rickets, osteoporosis, osteomalacia and other bone diseases. In addition, research well after the first discovery of vitamin D has shown that vitamin D deficiency and sunlight deprivation also lead to many cancers, heart disease and multiple additional maladies. Now, as the world has modernized, the population is moving indoors, and even in the areas that are sunny throughout the year, sunlight exposure and vitamin D deficiency is increasing, both in rural and urban populations. The bones become so weakened without regular sun exposure, that the slightest movement may cause a fracture. As an example, the mother of an acquaintance of mine—a woman who avoided the sun—turned over in bed one night and broke her hip. Osteoporosis often destroys all quality or life for those who suffer it.
The importance of the sun in maintaining and producing strong bones has been known since antiquity. Dr. Richard Hobday, author of The Healing Sun, writes the following comments along with a history in an online article.[1] “Traditionally, sunlight deprivation has been linked with weak or brittle bones. One of the earliest references to this was made more than two thousand years ago by the Greek historian Herodotus (480-425 BC), who noted a marked difference between the remains of the Egyptian and Persian casualties at the site of battle of Pelusium which took place in 525 BC:
‘At the place where this battle was fought I saw a very odd thing, which the natives had told me about. The bones still lay there, those of the Persian dead separate from those of the Egyptian, just as they were originally divided, and I noticed that the skulls of the Persians were so thin that the merest touch with a pebble will pierce them, but those of the Egyptians, on the other hand, are so tough that it is hardly possible to break them with a blow from a stone. I was told, very credibly, that the reason was that the Egyptians shave their heads from childhood, so that the bone of the skull is indurated by the action of the sun — this is why they hardly ever go bald, baldness being rarer in Egypt than anywhere else. This, then, explains the thickness of their skulls; and the thinness of the Persian’s skulls rests upon a similar principle: namely that they have always worn felt skull -caps, to guard their heads from the sun.’
Herodotus, ‘The Histories’”
And here is a perhaps the transcendent study on hip fracture and sun exposure: research in Spain showed that women who were sun seekers had only about one-eleventh the risk of hip fracture as those who stayed indoors[2] (See the chart below).
That is very powerful evidence of the efficacy of sun in preventing weak bones. In stark contrast to this research are studies done on women who completely avoid the sun and suffer from osteomalacia. Osteomalacia is a soft-bone disease known as adult rickets, resulting from severe vitamin D deficiency, which deficiency prevents bone from properly mineralizing. Women who seldom go outdoors, or who are nearly always fully covered with clothing, have an extremely high incidence of osteomalacia at a very young age, even if they live in geographical areas with abundant sunlight.[3] [4] If one is never exposed to the available sun, the sun will not be able to produce its beneficial effects on the body, so one may as well live at the North Pole.
Sunbed use also is associated with stronger bones and higher vitamin D levels. An excellent study compared 50 people who used sunbeds regularly with 106 who did not.[5] The sunbed group had 90% higher vitamin D, significantly higher bone density and lower PTH levels (high PTH levels are associated with lower bone mass). The users had healthful vitamin D levels of 46 ng/ml [115 nmol/L] compared to only 24 ng/ml [60 nmol/L] for those who did not regularly use sunbeds.
Scientists at one time believed that sunlight and vitamin D were good only for preventing rickets, osteoporosis and other bone weaknesses. That belief has been supplanted by myriad research studies that show the efficacy of both sun exposure and vitamin D repletion on protection against numerous additional diseases. Nevertheless, we should never forget the extraordinary, never-changing value of sun exposure to maintaining a strong skeleton well into old age.
[1]Richard Hobday. The Healing sun: Sunlight, Brittle Bones, and Osteoporosis. http://sunlightenment.com/the-healing-sun-sunlight-brittle-bones-and-osteoporosis/. (accessed February 5, 2016)
[2] Larrosa M, Casado E, Gómez A, Moreno M, Berlanga E, Ramón J, Gratacós J. Vitamin D deficiency and related factors in patients with osteoporotic hip fracture. Med Clin (BARC) 2008;130:6-9.
[3] Sahibzada AS, Khan MS, Javed M. Presentation of osteomalacia in Kohistani women. J Ayub Med Coll Abbottabad 2004;16:63-5
[4] Al-Jurayyan NA, El-Desouki ME, Al-Herbish AS, Al-Mazyad AS, Al-Qhtani MM. Nutritional rickets and osteomalacia in school children and adolescents. Saudi Med J 2002;23:182-85.
[5] Tangpricha V, Turner A, Spina C, Decastro S, Chen TC, Holick MF. Tanning is associated with optimal vitamin D status (serum 25-hydroxyvitamin D concentration) and higher bone mineral density. Am J Clin Nutr. 2004 Dec;80(6):1645-9.
By Marc Sorenson, EdD, Sunlight Institute
After coming across some research having to do with sun exposure and the seasonality of fractures, I thought it wise to share it with my readers.
In high latitude areas, which have far less sun availability than lower latitude areas, we would expect rates of hip fracture to be high, and such is the case. Sweden is a country that has large differences in latitude, and in research performed there it was shown that the higher the latitude and the lesser the sun exposure, the greater was the risk of hip fracture.[1] In other words, significantly more hip fractures occurred in the northern part of the country compared to the middle and southern parts. Another Swedish investigation demonstrated that in men, hip fracture risk was 37.5% lower in summer than winter. Women had a 23.5% reduced risk in summer.[2]
Research from Norway showed similar results. Hip fracture risk in men was 40% higher in winter than summer, and in women the risk was 25% higher.[3]These fluctuations in seasonal hip fractures indicate a loss of bone mass during periods of low sun exposure (winter) and an increase in bone mass during periods of high sun exposure (summer). In other words, sun exposure is able to reverse bone loss, or osteoporosis. Other studies show similar patterns of bone strength based on sun exposure or lack thereof.[4]
The importance of sunlight in maintaining and producing strong bones has been known since antiquity. Dr. Richard Hobday, author of The Healing Sun, writes the following comments and a history in an online article.[5] “Traditionally, sunlight deprivation has been linked with weak or brittle bones. One of the earliest references to this was made more than two thousand years ago by the Greek historian Herodotus (480-425 BC), who noted a marked difference between the remains of the Egyptian and Persian casualties at the site of battle of Pelusium which took place in 525 BC:
‘At the place where this battle was fought I saw a very odd thing, which the natives had told me about. The bones still lay there, those of the Persian dead separate from those of the Egyptian, just as they were originally divided, and I noticed that the skulls of the Persians were so thin that the merest touch with a pebble will pierce them, but those of the Egyptians, on the other hand, are so tough that it is hardly possible to break them with a blow from a stone. I was told, very credibly, that the reason was that the Egyptians shave their heads from childhood, so that the bone of the skull is indurated by the action of the sun — this is why they hardly ever go bald, baldness being rarer in Egypt than anywhere else. This, then, explains the thickness of their skulls; and the thinness of the Persian’s skulls rests upon a similar principle: namely that they have always worn felt skull-caps, to guard their heads from the sun.’ Herodotus, ‘The Histories’”
The message is this: Don’t hide yourself from the sun; rather, embrace it in a safe manner, and that will protect your bones.
[1] Nilson F, Moniruzzaman S, Andersson R. A comparison of hip fracture incidence rates among elderly in Sweden by latitude and sun exposure. Scand J Public Health. 2014 Mar;42(2):201-6.
[2] Odén A, Kanis JA, McCloskey EV, Johansson H. The effect of latitude on the risk and seasonal variation in hip fracture in Sweden. J Bone Miner Res. 2014 Oct;29(10):2217-23.
[3] Solbakken SM1, Magnus JH, Meyer HE, Emaus N, Tell GS, Holvik K, Grimnes G, Forsmo S, Schei B, Søgaard AJ, Omsland TK.
[4] Grønskag AB1, Forsmo S, Romundstad P, Langhammer A, Schei B. Incidence and seasonal variation in hip fracture incidence among elderly women in Norway. The HUNT Study. Bone. 2010 May;46(5):1294-8.
[5] Richard Hobday. The Healing sun: Sunlight, Brittle Bones, and Osteoporosis. http://sunlightenment.com/the-healing-sun-sunlight-brittle-bones-and-osteoporosis/. (accessed February 5, 2016)
.Marc Sorenson, EdD, Sunlight Institute
While perusing the medical and scientific literature for research that would be pertinent for my upcoming book on the value of sunlight exposure, I found a most interesting paper on sunlight exposure and bone strength.[i] The researchers searched the literature on three groups of patients, Alzheimer’s, Parkinson’s and Stroke which correlated to very high fracture rates among patients suffering from those diseases. They then found three randomized, controlled studies that determined the efficacy of sunlight exposure for reducing the risk of hip fractures in patients with these diseases.
In each study, there was a control group that did not receive the exposure and an experimental group that received regular sunlight exposure to a small part of the body daily for a year. The results were impressive: For Alzheimer’s patients, the reduction in hip fractures was 78% compared to the controls who stayed inside; for Parkinson’s patients, 73%; for stroke patients, 83%. Overall, the risk of the hip fracture was reduced by 77% in the sunlight exposed groups. Bone mass also increased in each sunlight-exposed group, so osteoporosis was obviously reversed. Did you even realize that such a thing was possible? You probably knew it only if you have been reading the Sunlight Institute blogs. There is an even more impressive study that I always mention when writing about sunlight and osteoporosis. For example, an investigation from Spain in 2008 concluded that women who actively participated in sun exposure had one-eleventh the chance of a hip fracture as those who stayed indoors.[ii] It appears from the materials on the different disease groups mentioned above, that reversibility is a reality, but how much more important is it to prevent the disease in the first place? The women in Spain did exactly that.
The National Osteoporosis Foundation estimates that osteoporosis was responsible for more than 2 million fractures in 2005, including 297,000 hip fractures, 547,000 vertebral fractures, 397,000 wrist fractures, 135,000 pelvic fractures and 675,000 fractures at other sites. The foundation also estimates that the number of osteoporotic fractures is expected to rise to more than 3,000,000 by 2025, and that an average 24 % of hip-fracture patients aged 50 and over die within one year following the occurrence of their fracture.[iii] If we take 24% of just the hip fractures that cause death we see that osteoporosis kills at least 71,280 people per year. Larrosa, M. Vitamin D deficiency and related factors in patients with osteoporotic hip fracture. Med Clin (BARC) 2008;130:6-9.
Do you believe that it might be worth a daily sunbath to save the lives of 70,000 people per year? Do you believe that it would be worth daily exposure (unprotected by sunscreen) to the sun (when possible) to reduce your own risk of fracture? Then why don’t we know about these statistics and the marvelous prophylactic effects of sunlight? That answers are simple: (1) it doesn’t sell any Fosamax or Boniva. (2) It doesn’t sell any noxious, deadly sunscreens. (3) It would be unthinkable for most dermatologists to admit that soaking up a little sun each day might be good for us. It has been said, “And ye shall know the truth and the truth shall make you free.”[iv] Now you have boned up on bone strength and sunlight, and you know the truth.
My fervent hope is that all may be free from the deceptions of those who would ignore the truth in favor of making another dollar.
[i] Iwamoto J, Takeda T, Matsumoto H. Sunlight exposure is important for preventing hip fractures in patients with Alzheimer’s disease, Parkinson’s disease, or stroke. Acta Neurol Scand. 2012 Apr;125(4):279-84
[ii] Larrosa, M. Vitamin D deficiency and related factors in patients with osteoporotic hip fracture. Med Clin (BARC) 2008;130:6-9.
[iii] National Osteoporosis Foundation, Fast Facts on Osteoporosis. Accessed Nov. 20, 2009 at http://www.nof.org/osteoporosis/diseasefacts.htm
[iv] John 8:32 (KJV)
The Indian Menopause Society (IMS), is an organization whose motto is to keep women fit at 40, active at 60 and independent at 80. One of their suggestions is that women stop soaking up sunscreen and start getting outside at peak sunlight time–for at least 15 minutes daily. The idea is to use the most natural manner possible to optimize vitamin D levels and thereby reduce the risk of osteoporosis and other bone diseases.
It is gratifying to see that there are women’s health organizations that understand the life-saving importance of sunlight. India is to be congratulated for cutting past the anti-sun nonsense and leading the world back to enlightenment. This is an excellent article from the Times of India.
The evidence has been mounting for some time that sunlight exposure can halt osteoporosis in its tracks. For example, an investigation from Spain in 2008 concluded that women who actively participated in sun exposure had one-eleventh the chance of a hip fracture as those who stayed indoors.[1] There is no bone drug that can create such dramatic results, and neither has vitamin D supplementation been able to create such results, although vitamin D was doubtlessly a major factor in the results of the Spanish research.
The beauty of sunlight exposure is the fact that it is irrefutably capable of reversing osteoporosis. A study from Japan furnishes the proof: Over twelve months, 129 elderly, hospitalized women were exposed to regular sunlight and another 129 stayed received no sunlight. The results were impressive. In these sedentary women, the sunlight group increased bone mass by an average 3.1%; in the non-sunlight-exposed group, it decreased by 3.3%.[2] More importantly, the women who had the benefit of sunlight had only one bone fracture in their group. The sunlight-deprived group had six fractures! Sunlight reversed osteoporosis. Vitamin D produced by the skin in response to sunlight likely played a large role in the reversal; blood levels increased by nearly 400% during the year. Nevertheless, the women remained vitamin D deficient, reaching levels of about 19 ng/ml. This may mean that something beyond vitamin D production—perhaps another photoproduct produced by the skin in response to sunlight—made a difference. Certainly, no study using vitamin D supplements alone has produced such results.
The aforementioned studies conclusively demonstrate that sunlight is the key to strong, healthy bones; nevertheless, corroborating information continues to emerge. Recently published research from Sweden showed the results of an investigation regarding the correlations among fracture rates, latitude and UV radiation[3] (the light spectrums of sunlight that stimulate the skin to produce vitamin D and other photoproducts such as nitric oxide, endorphins, etc.). The higher the latitude, the lower is the exposure to UV radiation. The investigators showed that there were statistically significant correlations between hip-fracture rates and latitude as well as UV radiation in Sweden. Obviously, this is another instance of sunlight exposure preventing osteoporosis and fracture.
Osteoporosis, like many other degenerative diseases, is an absolutely unnecessary malady. Plenty of sunshine and a healthful nutrition program can prevent and even reverse these illnesses.
[1] Larrosa, M. Vitamin D deficiency and related factors in patients with osteoporotic hip fracture. Med Clin (BARC) 2008;130:6-9.
[2] Sato, Y. Metoki N, Iwamoto J, Satoh K. Amelioration of osteoporosis and hypovitaminosis D by sunlight exposure in stroke patients. Neurology 2003;61:338-42.)
[3] Nilson F, Moniruzzaman S, Andersson R. A comparison of hip fracture incidence rates among elderly in Sweden by latitude and sunlight exposure. Scand J Public Health. 2013 Nov 21. [Epub ahead of print].
By: Marc Sorenson, Sunlight Institute–
In 1997, Dr. Y Sato and colleagues showed that sunlight deprivation (due to being hospitalized) in Parkinson’s patients resulted in compensatory hyperparathyroidism, which in turn led to reduced bone mass and excessive hip fractures.[1] In 1998, he made the same observation regarding elderly women with Alzheimer’s disease.[2] Then, in 2003, he reported that sunlight deprivation was also a cause of hip fractures in elderly women who suffered from stroke.[3] This time, however, he studied the effects of sunlight—or the lack thereof—on the bone mass of elderly women who were either exposed to sunlight or were kept inside a care facility. Over twelve months, 129 women were exposed to regular sunlight and another 129 received no sunlight exposure. The results were startling: in these sedentary women, the sunlight group increased bone mass by an average 3.1%; in the non-sunlight-exposed group, it decreased by 3.3%, a swing of 6.4%.
Of course, one might ask why a small increase in bone density in one group and a loss of bone density in the other makes any difference; the real question is whether it prevented hip fractures. Now consider this: as proof of the efficacy of improving bone mass, the women who had the benefit of sunlight had only one bone fracture in their group. The sunlight-deprived group had six fractures! This is obviously a reversal of osteoporosis and a reversal of fracture risk.
Sato was not through with his research; in 2005, he and his colleagues exposed a group of Alzheimer’s patients to sunlight for one year, and another was kept in a typical indoor hospital setting.[4] In the sunlight group a 220% increase in vitamin D levels was found, and bone mass increased by 2.7%. In the indoor group, bone mass decreased by 5.6%. That is a difference of 7.3% in only one year! The final proof, of course, is with fractures. In the sunlight group, there were three fractures; in the sunlight-deprived group there were eleven, or 3.7 times more.
Finally, in 2011, Dr. Sato and his group did a similar study on elderly patients with Parkinson’s disease.[5] A two-year program of sunlight exposure was compared to a two-year program of continued sunlight deprivation. This time, the sunlight group experienced an increase of 3.8% bone mass, whereas the sunlight-deprived group lost 2.6% bone mass. The sunlight group experienced three fractures and the sunlight deprived group, eleven fractures, as in the aforementioned study.
One more thought: An investigation in Spain concluded that women who actively participated in sun exposure had one-eleventh the chance of a hip fracture as those who stayed indoors.[6]
The conclusion: sunlight exposure not only prevents, but can also reverse osteoporosis and fractures. Every physician who treats this disease should have sunlight exposure as his number-one treatment protocol. But is anyone listening?
[1] Sato Y, Kikuyama M, Oizumi K. High prevalence of vitamin D deficiency and reduced bone mass in Parkinson’s disease. Neurology. 1997 Nov;49(5):1273-8.<?xml:namespace prefix = o />
[2] Sato Y, Asoh T, Oizumi K. High prevalence of vitamin D deficiency and reduced bone mass in elderly women with Alzheimer’s disease. Bone. 1998 Dec;23(6):555-7.
[3] Sato, Y. Amelioration of osteoporosis and hypovitaminosis D by sunlight exposure in stroke patients. Neurology 2003;61:338-42.
[4] Sato Y, Iwamoto J, Kanoko T, Satoh K. Amelioration of osteoporosis and hypovitaminosis d by sunlight exposure in hospitalized, elderly women with Alzheimer’s disease: a randomized controlled trial. J Bone Miner Res. 2005;20:1327-33.
[5] Sato Y, Iwamoto J, Honda Y. Amelioration of osteoporosis and hypovitaminosis D by sunlight exposure in Parkinson’s disease. Parkinsonism Relat Disord 2011;17(1):22-6.
[6] Larrosa, M. Vitamin D deficiency and related factors in patients with osteoporotic hip fracture. Med Clin (BARC) 2008;130:6-9.