Fishermen receive skin protection through sun exposure and vitamin D, by Marc Sorenson, EdD.
Fishermen in Brazil spend plenty of time on the sea and have healthy skin. Furthermore, they soak up vast quantities of direct sun exposure. Thus, should we expect them to succumb to incredibly high rates of skin cancer? No! Does this seem like a paradox? It should not. It is the perfectly natural outcome of plenty of non-burning sun exposure. This will seem clear to you if you have read my book, Embrace the Sun.
Recent research from Brazil produced some large and fascinating surprises. In addition, it changed a few minds regarding knowledge of sunlight’s healthful qualities. First of all, it illuminated sunlight’s protective effects against skin cancer, particularly in fishermen.
So how much sunlight do fishermen in Brazil soak up daily?
Due to their profession, commercial fishermen chronically expose themselves to sunlight. So, in this research, they had soaked up Brazilian sunlight for more than 15 years. The average exposure time was 21 to 28 hours weekly! Consequently, these fishermen received a sunlight dose 6-8 times higher than indoor workers did. Therefore, you might surmise that they used lots of sunscreen. Yet they did not. It is especially relevant that 62% of this population of fishermen used none. Must we therefore conclude that they suffered exceptionally high skin cancer risk? No. The frequency of skin-cancer diagnoses was 2.7% of the study population of 174 fishermen (and fisher women). The researchers stated, “There was a low prevalence of diagnosed skin cancer among the fishermen when compared to the general population.”
So there you have it. The general population, with comparatively little sun exposure, suffers from a high skin cancer risk.
Yet, fishermen practically bake in the sun every day, and have a minuscule risk of skin cancer. This paradox should be easily understood. Sun exposure is a superb prophylactic against skin cancer and most other cancers if used regularly and safely without burning. Remember that it causes the body to produce vitamin D, which may also provide protection against skin cancer.
For more information on sunlight and health, visit sunlightinstitute.org and read the book, Embrace the Sun.
HAPPY SUNNING!
Chemical sunscreen is toxic and hazardous. By Marc Sorenson, EdD

Chemical sunscreen has been mentioned in new medical and scientific papers lately, and the research is alarming. Yet, many governments and medical associations have not gotten the message. Consequently, I lately blogged about the idea being promoted in Australia and New Zealand, that sunscreen use is absolutely indispensable. Due to this promotion, a major Australian newspaper stated, “Make it like brushing your teeth.” That seems like a terrific slogan to line the pockets of chemical sunscreen manufacturers, no? But, it is most noteworthy that sunscreen use may lead to disability and even death.
A dermatology journal study takes chemical sunscreens to task.
But maybe the dermatology profession is starting to catch on. And Surprisingly, one of the best treatises on chemical sunscreen was written by dermatologists. It is rather interesting that they were strongly questioning the wisdom of chemical sunscreens. Furthermore, the study was published by the Clinical Dermatology Research Journal and was entitled, Should We Use Products Containing Chemical UV Absorbing Sunscreen Actives on Children?[1] This is amazing, because most dermatologists are loath to say anything about sunscreen that is not positive.
The salient points on chemical sunscreens from this research paper:
- A 2018 report from the American Cancer Society demonstrated the following: after 40 years of sunscreen use (1975-2014) melanoma increased 4 fold in men and 3 fold in women. (So how does that information lead to the usual mantra that we should always be covered in sunscreen?)
- Also, all six sunscreen chemicals (chemical UV absorbers) considered in this paper are known to be endocrine disrupting chemicals (EDCs). And oxybenzone, one of the worst offenders, has been shown to cause a significant decrease in sperm density. (Since sperm counts have dropped rapidly in the past few decades among men, could it be due to chemical sunscreen use?)
More facts about chemical sunscreens:
- Also, environmental exposure to chemical sunscreen in adolescent boys (ages 12-19) was associated with significantly lower total serum testosterone. Therefore, these chemicals would, as mentioned, produce lower sperm density.
- In addition, chemical sunscreen passes through human skin. (About 8% of Oxybenzone finds its way through the skin. It seems like using these noxious products is something most of us would want to avoid!)
Other research on chemical sunscreens that may interest you:
Another important study demonstrates that chemical sunscreen does not help prevent melanoma, and, it could be a cause. [2] Rather surprising, no? Most of all, the researchers’ goal was to determine the efficacy of sunscreens in preventing melanoma. Hence, they compared melanoma rates with sales in 24 countries in Europe, during the period of 1997-1999 to 2008 and 2012. They thus found that higher income people had significantly higher melanoma incidence. And, increased use of chemical sunscreens had not prevented higher income populations from being at higher risk of melanoma. Consequently, we see this equation: Higher sunscreen use=higher melanoma risk and therefore higher melanoma death risk!
But does chemical sunscreen prevent skin cancer?
So, the following research probably deflated the egos of chemical sunscreen manufacturers. A meta-analysis of 20 studies showed what many probably not expect. Because, both melanoma and non-melanoma skin cancers were not prevented by chemical sunscreens.[3] It is especially relevant that they were associated with a slight increase in risk, though this increase was not considered significant. We could probably say, from the information presented, that sunscreens are worthless at best, and dangerous at worst. So, who benefits? The manufacturers and distributors. And who suffers? The people, because they use the noxious products.
Does chemical sunscreen even prevent sunburns?
And now, another recent scientific study corroborates this conclusion (worthless at best, dangerous at worst) regarding chemical sunscreen.[4] The authors expected a different outcome—an outcome exactly opposite of what they found. The goal was to discover which sun-protection behavior was most effective in preventing sunburn. Hence, they designed a cross-sectional investigation using a nationally representative sample of about 32,000 US adults.
Excellent research method on chemical sunscreens
The researchers interviewed each participant, and they did it in person. This is especially relevant when attempting to achieve the most accurate results possible. We can conclude, therefore, that their findings regarding sunscreen use and other “sun-protective” behaviors have validity. The measured behaviors (beyond sunscreen use) were seeking shade, wearing a hat or visor, and wearing long sleeves and/or pants.
Results of the sunburn and chemical sunscreen study.
In addition, the researchers identified the subjects as sun-sensitive individuals or non-sun-sensitive individuals. Fifty-four percent of the subjects were women, and 15,992 of all individuals were considered sun-sensitive (fair skinned). Those who used only sunscreen had the highest sunburn likelihood (62.4%). The group with lowest likelihood of sunburn did not use chemical sunscreen but engaged in the other protective behaviors (24.3% sunburned).
A surprising conclusion that using chemical sunscreens was the worst choice!
In addition, among 12,566 non–sun-sensitive individuals, those engaged in all 4 protective behaviors had the lowest sunburn risk (6.6%). The highest likelihood of sunburn was among those who only used sunscreen (26.2%). Dr. Kasey Morris, the study leader, was stunned. She made the following statement: “The most surprising and counterintuitive finding was that regular sunscreen use, in the absence of other protective behaviors, was associated with the highest likelihood of sunburn.”[5]
The bottom line regarding chemical sunscreen and sunburns
So, you should now understand this fact: chemical sunscreen use associates closely with sunburning. [3] That fact has actually been known since 2014.[6] Therefore, sunscreen is not a good product. Of course, we should protect ourselves from overexposure to sunlight. But, we should do it the way God (or Mother Nature, if you prefer) intended it: 1. Cover up with clothing when you start to redden, 2. Seek shade. 3. Go indoors for awhile. And remember that good health depends on obtaining regular, non-burning sun exposure. Happy sunning!

Read more on sunscreens and toxicity in my new book, Embrace the Sun, available at Amazon. https://www.amazon.com/Embrace-Sun-Marc-B-Sorenson/dp/069207600X

[1] DiNardo JC and Downs CA, Should We Use Products Containing Chemical UV-Absorbing Sunscreen Actives on Children? Clin Dermatol Res J 2019, 4:1.
[2] Williams SN, Dienes KA. Sunscreen Sales, Socio-Economic Factors, and Melanoma Incidence in Northern Europe: A Population-Based Ecological Study. SAGE Open October-December 2014: 1–6.
[3] Elizabet saes da SILVA, Roberto TAVARES, Felipe da silva PAULITSCH, Linjie ZHANG. Eur J Dermatol 2018; 28(2): 186-201.
[4] Kasey L. Morris, PhD; Frank M. Perna, EdD, PhD. Decision Tree Model vs Traditional Measures to Identify Patterns of Sun-Protective Behaviors and Sun Sensitivity Associated With Sunburn. JAMA Dermatol. Published online June 27, 2018.
[5] https://www.reuters.com/article/us-health-sunburns/sun-sensitive-people-need-more-than-sunscreen-to-avoid-sunburn-idUSKBN1K02RB
[6] https://www.webmd.com/beauty/news/20110714/sunscreen-users-more-likely-burn#1
Sunscreens are not toothpaste. By Marc Sorenson, EdD.
Sunscreens, in Australia and New Zealand, are being touted as absolutely indispensable to prevent of skin cancer. And, this has been the mantra for decades. So, experts from the two countries convened to obtain opinions and produce a statement regarding use of sunscreens.[1] Much as I expected, they concluded people should apply sunscreen daily when the UV index reaches 3. And for much of Australia, that means every day.
Thus, as a result of this declaration, a major Australian newspaper weighed in. They stated “Make it like brushing your teeth:”[2] https://www.brisbanetimes.com.au/national/queensland/make-it-like-brushing-your-teeth-experts-urge-daily-sunscreen-use-20190124-p50thn.html. Rather convenient for those who produce sunscreens, no? If this advice is taken to heart by the people, sunscreen manufacturers and their stockholders will make a fortune. However, I guarantee that the people will suffer.
Increasing use of sunscreens and skin cancer through Slip, Slop, Slap.
It is especially relevant that Australians have been using a campaign called Slip, Slop Slap for decades. The campaign pushes everyone to avoid the sun and use sunscreens. And, according to Cancer Council Australia (the biggest manufacturer of sunscreens in Australia and New Zealand), it is remarkably effective.[3] Thus they state, “The Slip Slop Slap slogan has become institutionalized as the core message of Cancer Council’s SunSmart program.” And, they say the campaign has played a key role in the shift in sun protection behavior over two decades. (The program has actually been used for about three decades.) Because of this program, Australians and New Zealanders use more sunscreens than any other countries on earth, and the use of sunscreens continues to rise. But as a result of this sunscreen use, has skin cancer diminished?
How are the sunscreens promotions working for the health of the Australian people?
First of all, this is not new information; it has been known for decades. Dr. David Myers, a dermatologist, thus wrote an article that contains this statement: “The Australian experience provides the first clue. The rise in melanoma has been exceptionally high in Queensland where the medical establishment has long and vigorously promoted the use of sunscreens. Queensland now has more incidence of melanoma per capita than any other place. Worldwide, the greatest rise in melanoma has been experienced in countries where chemical sunscreen have been heavily promoted.”[4] [5]
And Dr. Cedric Garland echoed that statement, saying that Queensland, Australia has vigorously promoted sunscreens for decades. And he also says that Queensland now has one of highest rates of melanoma in the world.[6] [In addition, the rate of vitamin D deficiency there is becoming critical.[7]]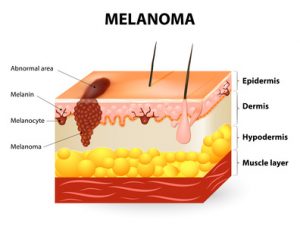
Does the Australian sunscreen declaration run up against some inconvenient truths?
So, we have a declaration suggesting that we should use sunscreens regularly like toothpaste. The declaration obviously implies that sunscreens are protective against skin cancer in Australia. It is hard to explain that conclusion. Why? Because the long-term, exponentially increasing use of sunscreens has been accompanied by an exponential increase in skin-cancer incidence. Therefore, if sunscreens are protective against skin cancer, there is something very wrong with that history.
And, unfortunately, skin cancer also continues to rise. Hence, Australia and New Zealand have more skin cancer than any other country on earth.[8] [9] It seems like this emphasis on sunscreens has not worked. So we come up with this new formula. More use of sunscreens over the years=higher risk of skin cancer. And, it appears that they want to continue using this formula!
But of course, the “experts’” solution is to ignore the historical facts and promote the use of more sunscreens. It seems like these people have not heard the old saying: “Doing the same thing over and over, and expecting different results, is the definition of insanity.” So, shall we be as dedicated to sun screen use as we are to brushing our teeth? Shall we make the use of sunscreens like the use of toothpaste? I have a secret for the people who promote sunscreens: Sunscreens are nothing like toothpaste, because toothpaste may actually accomplish something.
Should North America adopt this Australian recommendation of daily use?
First of all, according to the main research used for this recommendation, the answer is a big NO. One of the Australian researchers, Adele Green, made this statement: “Although the results are directly relevant to people who live in sunny climates like Australia’s and who receive relatively high levels of ambient sun exposure as a matter of course, they also have implications for white people living in temperate climates in North America and Europe who are at increased risk of melanoma because of increased solar UV exposure caused by the predilection for holidays in sunny places.” So they are saying sunscreens are NOT required unless on sunny holidays or if you have a sunburning risk. This doesn’t sound like a recommendation for daily use in North America. And, as European research demonstrated, it is certainly not a useful recommendation for Europe. (See the heading below regarding Europe.)
North American research on sunscreens and skin cancer
Another piece of research[10] looked at sunscreen use in North America and stated the following; “In contrast, for people who live at higher latitudes where UV radiation is weaker and less constant, regular sunscreen use may provide less protection against skin cancer, or even increase the risk of carcinogenesis.” The paper goes on to say “While the current evidence suggests no increased risk of skin cancer related to sunscreen, this systematic review and meta-analysis does not confirm the expected protective benefits of sunscreen use against skin cancer in the general population.” So again, this is NOT a recommendation for daily use of sunscreens. And, it indicates they may do more harm than good.
Are sunscreens counterproductive?
So it appears, based on what has been written so far, that sunscreens may be worthless at best and dangerous at worst. Another recent scientific study on sunscreens and sunburns corroborates this conclusion.[11] The authors of this study expected an outcome opposite of the facts. The goal was to discover which sun-protection behavior, including use of sunscreens, was most effective in preventing sunburn. Hence, they designed a cross-sectional investigation using a nationally representative sample of about 32,000 U.S. adults. And, those conducting the research interviewed each participant in person. This is especially relevant when attempting to achieve the most accurate results possible. We can conclude, therefore, that their findings regarding sunscreen use and other “sun-protective” behaviors have validity. Those other sun-protective behaviors included seeking shade, wearing a hat or visor, and wearing long sleeves and pants.
Sunscreens and sunburn results
In addition, the subjects were identified as sun-sensitive individuals or non-sun-sensitive individuals. Fifty-four percent of the subjects were women, and 15,992 of all individuals were considered sun-sensitive. It is most noteworthy that among sun-sensitive individuals, those who used only sunscreens had the highest sunburn likelihood (62.4%). The group with lowest likelihood of sunburn did not use sunscreens but engaged in the other protective behaviors (24.3% sunburned). In addition, among 12,566 non–sun-sensitive individuals, those engaged in all 4 protective behaviors had the lowest sunburn risk (6.6%). And in that group, the highest likelihood of sunburn was among those who only used sunscreen (26.2%). According to Dr. Kasey Morris, who led the study, “the most surprising and counterintuitive finding was that regular sunscreen use, in the absence of other protective behaviors, was associated with the highest likelihood of sunburn.”[12]
What do dermatologists believe about sunscreen and sunburn?
I have never heard of a dermatologist who didn’t believe that sunburns led to skin cancer. And I have only seldom heard of dermatologists who didn’t believe that sunscreens prevented sunburns. This research turns their beliefs about sunscreen upside down.
I have also been told that the reason sunburn occurs with the use of sunscreens, is this: People get a false sense of safety while using sunscreens. Consequently, they stay out in the sun for excessively long times. To me that doesn’t matter. If sunscreen leads to sunburn, which leads to skin cancer, who cares what the reason is? When using a poison, does it matter what the mechanism of poisoning is if the patient dies? Why use a product that causes harm?
Other sunburn results with sunscreens
Finally, it has been known since 2014 that sunscreen use associates closely with sunburning.[13] Therefore, sunscreens are not good products. We should protect ourselves from overexposure to the sun the way God (or Mother Nature, if you prefer) intended it. 1. Cover up when you start to redden, 2. seek shade or 3. go indoors. And remember that good health depends on obtaining regular, non-burning sun exposure.
Another reason to avoid sunscreens
The state of Hawaii has now banned this noxious product. This is because of the destruction of the coral reefs caused by certain ingredients in this chemical soup. In addition, we know that since the first sunscreens were introduced, the risk of melanoma skin cancer has increased. How much? By about 3,000%. And yes, you read that correctly. If you have other questions, read the sunscreen section of my new book, Embrace the Sun,.https://www.amazon.com/Embrace-Sun-Marc-B-Sorenson/dp/069207600X
Use of sunscreens in Europe
Another important study demonstrates that sunscreens do not help prevent melanoma.[14] The researchers’ goal was to determine the efficacy of sunscreens in preventing melanoma. Hence, they compared melanoma rates with sales in 24 countries in Europe, during the period of 1997-1999 to 2008 and 2012. They found that higher income people had significantly higher melanoma incidence. And, increased sunscreen use had not prevented higher income populations from being at higher risk of melanoma. Consequently, we see this equation again: Higher sunscreen use=higher melanoma risk! One of the reasons for this little-known relationship is most noteworthy. Up to 99% of vitamin D production is stopped by sunscreen.[15] Therefore, many of the health benefits of sun are voided.
Summary on sunscreens and sunlight:
The best sunscreen, when you need it, is covering your skin with clothing, or going indoors. Stay away from the noxious chemicals. Be sure to obtain some non-burning sunlight whenever possible.
Happy sunning!
[1] David C. Whiteman, Rachel E. Neale, Joanne Aitken, Louisa Gordon, Adele C. Green, Monika Janda, Catherine M. Olsen, H. Peter Soyer, on behalf of the Sunscreen Summit Policy Group. When to apply sunscreen: a consensus statement for Australia and New Zealand. When to apply sunscreen: a consensus statement for Australia and New Zealand.
[2] https://www.theage.com.au/national/queensland/make-it-like-brushing-your-teeth-experts-urge-daily-sunscreen-use-20190124-p50thn.html
[3] https://www.cancer.org.au/preventing-cancer/sun-protection/campaigns-and-events/slip-slop-slap-seek-slide.html
[4] http://www.yourhealthbase.com/sunscreens.htm
[5] Garland, Cedric F., et al. Could sunscreens increase melanoma risk? American Journal of Public Health, Vol. 82, No. 4, April 1992, pp. 614-15
[6] Garland CF, Garland FC, Gorham ED. Could sunscreens increase melanoma risk? American Journal of Public Health, Vol. 82, No. 4, il 1992, pp. 614-15.
[7] Van der Mei IA, Ponsonby AL, Engelsen O, Pasco JA, McGrath JJ, Eyles DW, Blizzard L, Dwyer T, Lucas R, Jones G. A high vitamin D insufficiency across Australian populations and latitude. Environmental Health Perspect 2007;115:1132-39.
[8] https://www.rightdiagnosis.com/news/skin_cancer_rate_increasing_in_australia.htm.
[9] https://www.sciencelearn.org.nz/resources/1329-nz-skin-cancer-statistics
[10] Elizabet saes da SILVA, Roberto TAVARES, Felipe da silva PAULITSCH, Linjie ZHANG. Use of sunscreen and risk of melanoma and non-melanoma skin cancer: a systematic review and meta-analysis. Eur J Dermatol 2018; 28(2): 186-201.
[11] Kasey L. Morris, PhD; Frank M. Perna, EdD, PhD. Decision Tree Model vs Traditional Measures to Identify Patterns of Sun-Protective Behaviors and Sun Sensitivity Associated With Sunburn. JAMA Dermatol. Published online June 27, 2018
[12] https://www.reuters.com/article/us-health-sunburns/sun-sensitive-people-need-more-than-sunscreen-to-avoid-sunburn-idUSKBN1K02RB
[13] https://www.webmd.com/beauty/news/20110714/sunscreen-users-more-likely-burn#4
[14] Williams SN, Dienes KA. Sunscreen Sales, Socio-Economic Factors, and Melanoma Incidence in Northern Europe: A Population-Based Ecological Study. SAGE Open October-December 2014: 1–6.
[15] Matsuoka LY, Ide L, Wortsman J, MacLaughlin JA, Holick MF. Sunscreens suppress cutaneous vitamin D3 synthesis. Journal of Clinical Endocrinology & Metabolism 1987; 64:1165-68.
Antioxidants: power against skin cancer. Marc Sorenson, EdD
Antioxidants can quench (eliminate) free radicals.
Antioxidants are popular as supplements, and they are found many foods, but especially in fruits and vegetables. Because they are critical to good nutrition, let’s first consider what they do to a prevent cancer. First of all, what are they? They are substances that eliminate free-radical atoms and molecules. These radicals are formed by combining oxygen with stable atoms, hence the term “oxidation.” Therefore, we must also understand the free radical in order to understand the antioxidant’s importance.
Antioxidants and the notorious free radical 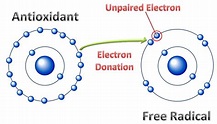
A free radical is a highly unstable atom capable of independent existence and having at least one unpaired electron in its outer shell.[1] So, when an atom loses an electron, it becomes unstable in an attempt to reestablish balance. Because this atom “craves” to have its balance restored, it will “steal” an electron from another atom to achieve stability. Therefore, the atom from which the electron is stolen becomes another free radical. The first atom now becomes stable because it has snatched an electron. Consequently, however, the atom from which the electron is snatched becomes another free radical.
So this process repeats innumerable times.[2] And this chain reaction cannot cease until another substance, with an extra electron to “give away,” steps in. That substance finally furnishes the electron that produces stability. That substance, of course, is an antioxidant. 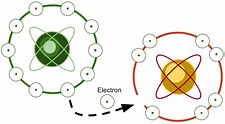 Thus, antioxidants can furnish electrons to stabilize free radicals without causing damage. Hence, they are like the hero who gives his life for the team and then passes on.
Thus, antioxidants can furnish electrons to stabilize free radicals without causing damage. Hence, they are like the hero who gives his life for the team and then passes on.
Oxygen in free-radical formation
As mentioned, the process of free-radical formation is known as oxidation, because free radicals are usually formed due to oxygen molecules, which are unstable. This is possible because oxygen easily combines with other substances. Oxygen gives us life, but its byproducts, if not controlled, can quickly end life. As an iron pipe rusts, it is because it succumbing to the free-radical attack of oxidation. When anything burns, free radicals form. Due to oxidation, a single cigarette creates about one quadrillion free-radical attacks.[3] Cooking creates massive quantities of free radicals. Breathing, heart beat and exercise also create oxidation. It is most noteworthy to understand that without antioxidants, our metabolic processes would shortly kill us because of oxidation.
Antioxidants and skin cancer
Oxidation damages DNA, and unchecked, it causes cancer. Therefore, the fact that smoking kills so many people attests to an obvious reality. Because smokers have insufficient levels of antioxidants to handle the free-radical load, they succumb to cancer. In fact, smoking is a major cause of non-melanoma skin cancers (NMSC); the greater the number of cigarettes smoked, the greater is the risk of skin cancer.[4] So, how important are antioxidants to cancer prevention, especially non-melanoma skin cancer? The research on antioxidants and skin cancer expatiates on this subject.[5]
More important research on antioxidants and Basal Cell Carcinoma (BCC)
The research just mentioned tells us that NMSC accounts for more that half of all diagnoses of cancer. And basal cell skin cancer (BCC) accounts for 70-80% of skin tumors. So, the researchers set out to determine the influence of antioxidants on NMSC. They tested 84 individuals and divided them into two groups: 1. a control group of healthy people, and 2. a case group of those who were undergoing surgery for BCC. In addition, they measured the blood of each group for free-radical markers, and then they compared the two groups. Also, they assessed the usual dietary intake of the subjects. As a result they discovered that the case group had significantly higher markers of oxidative stress compared with controls. While these results were impressive, there were other interesting results:
Other results regarding antioxidants
- Especially relevant was that antioxidants from foods were more pronounced in the control group. It seems like antioxidants from food must have been protective against BCC. Why? Because the intake of foods containing antioxidants showed their influence in reducing oxidative stress. Most of all, vitamins A and E were more prevalent among the non-diseased subjects.
- Also, the dietary concentrations of antioxidants minerals such as zinc, copper and selenium in the case group were significantly lower than healthy controls.
The power of fruits and veggies. 
Vegetables and fruits rich in antioxidants are protective against various diseases. We know this due to a plethora of research and observations. This research adds more information indicating that we should stop blaming the sun for skin cancer and clean up our diets. See sunlightinstitute.org for more information on skin cancer and nutrition, And to learn more about the benefits of sunlight, read my book, Embrace the Sun, available at Amazon. https://www.amazon.com/Embrace-Sun-Marc-B-Sorenson/dp/069207600X 
Also, search sunlightinstitute.org: http://sunlightinstitute.org/protect-skin-nutrition-sun-exposure/
Happy sunning!
[1] Karlsson, J. Introduction to nutraology and radical formation. In: Antioxidants and Exercise. Illinois: Human Kinetics Press 1997:1-143. Goldfarb, A. et al. Nutritional antioxidants as therapeutic and preventive modalities in exercise-induced muscle damage. Can. J. Appl. Physiol 1999;24:249-266.
[2] Goldfarb, A. et al. Nutritional antioxidants as therapeutic and preventive modalities in exercise-induced muscle damage. Can. J. Appl. Physiol 1999;24:249-266.
[3] Rahman, I. et al. Role of antioxidants in smoking- induced lung disease. Free Rad Biol Med 1996;21:669-681.
[4] De Hertog, S. et al. Relation between smoking and skin cancer. J Clin Oncol 2001;19:231-238.
[5] Freitas Be, de Castro LL, Aguiar JR, de Araújo CG, Visacri MB, Tuan BT, Pincinato Ede C, Moriel P. Antioxidant capacity total in non melanoma skin cancer and its relationship with food consumption of antioxidant nutrients. Nutr Hosp. 2015 Apr 1;31(4):1682-8.
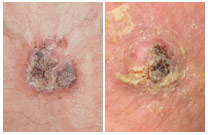 Skin cancer is rampant. In an earlier blog, evidence was presented that a common drug for erectile dysfunction, sildenafil (Viagra), had a nasty side effect: Its use was associated with an increased risk of melanoma.[1]
Skin cancer is rampant. In an earlier blog, evidence was presented that a common drug for erectile dysfunction, sildenafil (Viagra), had a nasty side effect: Its use was associated with an increased risk of melanoma.[1]
Now, another study from Denmark demonstrates that a popular drug for high blood pressure is dangerous. It substantially raises the risk of non-melanoma skin cancer (NMSC).[2] The NMSC specifically studied was squamous cell carcinoma (SCC), which is easily treated and has a low mortality rate. Nevertheless, it is something we should try to avoid. Hydrochlorothiazide is the drug. It is popular in both the U.S. and Western Europe. Approximately 10% of all cases of squamous cell carcinoma may be caused by Hydrochlorothiazide. Especially relevant is this fact: In Denmark, the risk of developing squamous cell carcinoma is up to seven times greater for users of Hydrochlorothiazide.[3] However, It should be noted that other types of blood-pressure medication did not show the same effects in promoting skin cancer.
Why do we post this information on skin cancer?
The reason for posting this information? To try to halt the idea that sun exposure is the cause of all skin cancers. In fact, there is a plethora of evidence against that idea. Furthermore, regular, non-burning sun exposure is protective against melanoma in most people. In previous blogs for Sunlight Institute, we have offered evidence that lack of foods such as nuts, seeds, tomatoes, greens and fruits increase skin cancer risk. Meat consumption has also been shown to increase the risk of melanoma. So has alcohol consumption. PCB exposure also increases the risk. Being obese is another risk factor. Hence, Hydrochlorothiazide has many partners in promoting skin cancer.
In conclusion: When you see that someone has a skin cancer, think! Is it due to drugs? Is it due to poor nutrition? While sunlight may have an influence on squamous cell carcinoma, we should definitely not immediately determine that it is caused by our friend, the Sun. 
[1] Li WQ, Qureshi AA, Robinson K, Han J. Sildenafil use and increased risk of incident melanoma in US men: a prospective cohort study. JAMA Intern Med. 2014 Jun;174(6):964-70C.
[2] Arnspang S, Gaist D, Johannesdottir Schmidt SA, Hölmich LR, Friis S,
Pottegård A, Hydrochlorothiazide use and risk of non-melanoma skin cancer: A nationwide case-control
study from Denmark, Journal of American Dermatology (2017), doi: 10.1016/j.jaad.2017.11.04
[3] Popular blood pressure medicine linked with increased risk of skin cancer. Medical Express News, Nov. 5, 2017. https://medicalxpress.com/news/2017-12-popular-blood-pressure-medicine-linked.html;
In an impressive mouse study,[1] it was shown that in animals that were exposed to high doses of radiation during a 35-week program, those that were fed a pre-radiation dose of tomato powder or tangerine powder had a higher level of the antioxidant lycopene than mice who were not fed the powders (control group). Lycopene is a potent antioxidant found in tomatoes, tangerines, watermelon and other fruits and vegetables.
Interestingly, the animals that consumed the tangerine powder had higher levels of lycopene than those consuming the tomato powder, but the results were not as impressive. The number of cancerous tumors that developed in the tomato-fed mice was about half the number that developed in the control group. Tomatoes obviously have anti-skin cancer attributes, but remember that lycopene may not be as effective as the whole tomato powder in reducing that disease. Whole foods are nearly always superior to the nutrients extracted from them, as all of the nutrients work in concert to help health whether for mice or men. There may be hundreds of nutrients besides lycopene in tomatoes, all having a positive effect in protecting against cancer. Why just take one nutrient from the tomato and put it in a pill? I’ll tell you why: It is a way to make money. In this case, the researchers discovered that important substances called glycoalkaloids were significantly higher in the skin after the ingestion of tomato powder, and seem to believe that these substances were responsible for the reduced risk of skin cancer.
It has actually been known for some time that some of the best skin protectants are tomatoes. One investigation showed that among individuals who consumed forty grams of tomato paste daily for ten weeks, sunburn-resistance time increased by 40%,[2] and other research demonstrated that eating different tomato-based products correlated to significantly reduced risk of sunburn after exposure to ultraviolet radiation from sunlamps.[3] It is also known that individuals with the lowest intake of alpha-carotene, beta-carotene, cryptoxanthin, lutein, and lycopene (all carotenoid antioxidants found in such vegetables such as carrots and tomato) had a 50% increased risk for melanoma.[4]
There are several other scientific investigations demonstrating that high fruit and vegetable consumption predict a lesser risk of skin cancer.[5],[6],[7], [8]
There are few foods that taste better than a ripe, field-grown tomato. Eat your fill and enjoy some regular, non-burning sun.
[1] Cooperstone JL, Tober KL, Riedl KM, Teegarden MD, Cichon MJ, Francis DM, Schwartz SJ, Oberyszyn TM. Tomatoes protect against development of UV-induced keratinocyte carcinoma via metabolomic alterations. Sci Rep. 2017 Jul 11;7(1):5106.
[2] Stahl W, Heinrich U, Wiseman S, Eichler O, Sies H, Tronnier H. Dietary Tomato Paste Protects against Ultraviolet Light–Induced Erythema in Humans. J Nutr 2001;131:1449-51.
[3] Aust O, Stahl W, Sies H, Tronnier H, Heinrich U. Supplementation with tomato-based products increases lycopene, phytofluene, and phytoene levels in human serum and protects against UV-light-induced erythema. Int J Vitam Nutr Res 2005;75:54-60.
[4] Millen AE, Tucker MA, Hartge P, Halpern A, Elder DE, Guerry D 4th, Holly EA, Sagebiel RW, Potischman N. Diet and melanoma in a case-control study. Cancer Epidemiol Biomarkers Prev 2004;13:1042-51
[5] Afaq F, Katiyar SK. Polyphenols: skin photoprotection and inhibition of photocarcinogenesis.Mini Rev Med Chem. 2011 Dec;11(14):1200-15.
[6] Afaq F, Katiyar SK. Skin photoprotection by natural polyphenols: Anti-inflammatory, anti-oxidant and DNA repair mechanisms. Arch Dermatol Res 2010;302:71.
[7] Stahl W, Heinrich U, Wiseman S, Eichler O, Sies H, Tronnier H. Dietary Tomato Paste Protects against Ultraviolet Light–Induced Erythema in Humans. J Nutr 2001;131:1449-51.
[8] Meyskens FL Jr, Farmer PJ, Anton-Culver H. Diet and melanoma in a case-control study. Cancer Epidemiol Biomarkers Prev 2004;13:1042-51.
By Marc Sorenson, EdD for sun exposure and health…
The Vitamin D Society of Canada has just released one of the best articles on the relationship of sun exposure and its potential for vitamin D production. Sun exposure is the natural way to obtain your essential vitamin D, and of course provides other essential photoproducts such as nitric oxide, serotonin, endorphin and BDNF.
Here is the press release from the Vitamin D Society, in full:
NEWS RELEASE
For Immediate Distribution
TORONTO, Ont (April 4, 2017) – The daylight hours are getting longer, the sun is getting stronger and summer is just around the corner. Make this the year that you optimize your vitamin D levels through effective sun exposure. Enjoy the health benefits and disease prevention from optimal vitamin D levels and learn to control your risks from sun exposure.
Vitamin D is made naturally in your body when UVB rays from the sun convert cholesterol in your skin to pre-vitamin D3. We make about 90% of our vitamin D from UVB sun exposure. UVB rays are short and only reach the earth when the sun is directly above us. We can’t make vitamin D in the winter in Canada because the sun is at too low of an angle and the UVB rays are absorbed in the atmosphere.
You make vitamin D in Canada between the months of May and October. The best time for exposure is around midday, between 10am and 2pm, when the UV index is above 3 and your shadow is shorter than your height. The further you get from noon, the lower the amount of vitamin D you’ll make. The sun’s visible light may penetrate through glass, but UVB light will not; therefore you will not make vitamin D.
Full body sun exposure at non-burning levels can create between
10,000-25,000 IU of vitamin D in your skin. You can never get too much vitamin D from the sun as your skin self regulates, whereas ingesting vitamin D does not have the same control. In addition, vitamin D that you make from the sun lasts twice as long in your body as vitamin D taken through supplements or food.
Statistics Canada reports that Canadian vitamin D levels have dropped by 10% over the past six years. The root cause of this decrease is lower sun exposure. People are just not getting outside around midday in the summer and making vitamin D, and when they are outside they are using sunscreen, which if applied correctly prevents 95%+ of vitamin D production.
In Canada, 12 million Canadians (35%) have vitamin D blood levels below the recommendations from Health Canada. This puts these people at a higher risk for several diseases, including cardiovascular disease, cancer, osteoporosis, diabetes, multiple sclerosis, Alzheimer’s disease and many more. In fact, a study completed in 2016 reported that if Canadians increased their vitamin D levels to the recommended level of 100 nmol/L, we would save $12.5B in healthcare costs and 23,000 premature deaths annually.
A recent study reported that women who avoided the sun have twice the risk of all cause death. The authors said that “avoidance of sun exposure is a risk factor for death of a similar magnitude as smoking.”
Skin cancer is a concern and risk of sun exposure must be managed and balanced with the benefits from vitamin D and other photoproducts. Research has shown that people with higher sun exposure such as outdoor workers, who have 3-10 times the sun exposure as indoor workers, have a lower incidence of melanoma. The National Cancer Institute reports that
melanoma risk is increased as a result of intermittent acute sun
exposure leading to sunburn. People who are a skin type 1, with white or very pale skin colour, red or blonde hair colour and who always burn and never tan, should severely limit their sun exposure.
The Vitamin D Society offers the following tips:
– Know your own skin and skin type. Don’t burn. Never overexpose yourself.
– Acclimatize or condition your skin for sun exposure by gradually
building or lengthening exposure times as your skin begins to tan to reduce your risk of burning
– Prevent burning and overexposure when required through the use of hats, clothing, shade and sunscreens.
– For vitamin D, get sun exposure at midday, between 10 am and 2 pm, when the UV index is above 3 and your shadow is shorter than your height.
– Expose more skin for a shorter period of time to generate more vitamin D while reducing your risk of overexposure.
It’s important to manage the risk and enjoy the rewards of moderate sun exposure for good health. Cancer Research UK, through the Consensus Vitamin D Position Statement, offers the following recommendation:
“Enjoying the sun safely, while taking care not to burn, can help provide the benefits of vitamin D without unduly raising the risk of skin cancer.”
“This advice may go against what current health organizations
recommend,” says Perry Holman, Executive Director of the Vitamin D Society. “They typically recommend you stay out of the sun at midday and use sunscreen when outdoors. But this would reduce your potential vitamin D production and does not consider the benefits as well as the risks of sun exposure on overall health. You need to have balance.”
About the Vitamin D Society:
The Vitamin D Society is a Canadian non-profit group organized to increase awareness of the many health conditions strongly linked to vitamin D deficiency; encourage people to be proactive in protecting their health and have their vitamin D levels tested annually; and help fund valuable vitamin D research. The Vitamin D Society recommends people achieve and maintain optimal 25(OH)D blood levels between 100 –
150 nmol/L (Can) or 40-60 ng/ml (USA).
To learn more about vitamin D, please visit www.vitamindsociety.org
For more information, please contact:
Melissa Andrade, Enterprise Canada 905-346-1230
mandrade@enterprisecanada.com.
THIS PRESS RELEASE CONTAINS MUCH OF WHAT YOU NEED TO KNOW ABOUT VITAMIN D, SUN EXPOSURE AND HEALTH. Please read it carefully, as it could save your life.
Marc Sorenson.
By Marc Sorenson, EdD, for sun exposure…
A new research paper on sun exposure and cancer has some interesting observations and some errors.[1] It is entitled, Does Sunlight protect us from cancer? Here is the abstract of the article, verbatim.
“The Ultraviolet (UV) radiation contained in sunlight is a powerful mutagen and immune suppressant which partly explains why exposure to solar UV is the biggest risk factor for the development of cutaneous tumors. Evidence is building that sunlight may be protective against some internal malignancies. Because patients with these tumors are often vitamin D deficient, this has led some to propose that vitamin D supplementation will be beneficial in the treatment of these cancers. However, the results from already completed trials have been disappointing which has given weight to the argument that there must be something else about sunlight that explains its cancer-protecting properties.”
The first sentence, of course, is false. The idea, that sun exposure is the biggest risk factor for skin cancer, is erroneous. We have presented materials many times, proving that melanoma is not caused by sun exposure, and that sun exposure is protective against that disease. And as regards common skin cancers, we have shown that high-fat nutrition, lack of antioxidants, meat consumption and alcohol intake are all risk factors. Search the blogs on this site to read the different articles.
The statement is correct, of course, that sunlight is protective against many internal cancers. Dr. Bill Grant and I are finishing our book, Embrace the Sun, where we present nearly all of the research on the protective influence of sun exposure against cancer.
The statement that vitamin D research has been disappointing is both true and false. Randomized controlled studies (RCTs) have shown the vitamin D supplements do have a protective effect against internal cancers, contrary to the statement by the researchers.
Finally, let’s look at the statement that there is something beyond vitamin D that explains the cancer-protecting properties of sun exposure. That is partially true. Beyond vitamin D, the sun causes the production of nitric oxide, serotonin, endorphin and BDNF, all of which are vital to human health, and may have their own cancer-protective properties.
The bottom line? Eat correctly (avoid junk), REGULARLY soak up some sun around midday and get plenty of exercise. That advice will be a boon to your health in myriad ways.
UVB exposure benefits by Marc Sorenson, EdD. Sunlight Institute…
UVB is a spectrum of sunlight that is responsible for stimulation of vitamin D production in the skin. It also has many other effects, including the suppression of inflammation in the skin, and thus has been used to very successfully treat skin diseases such as psoriasis and eczema.[1] [2] [3] [4]
Since inflammation is also necessary to produce the condition of atherosclerosis (arterial plugging or occlusion) in arteries, it would be interesting to know whether UVB light might also have the same anti-inflammatory effects in those arteries. If so, the UVB effect could inhibit or eliminate atherosclerosis, and by so doing provide an entirely new treatment for heart disease and other vascular events such as stroke and intermittent claudication.
The idea that UVB could prevent atherosclerosis by reducing inflammation in arteries was recently studied by Japanese researchers.[5] [6] Using a mouse model, they demonstrated that UVB light irradiation, once weekly for 14 weeks, leads to an increase in the action of T-regulatory cells that inhibit inflammation. In addition, UVB exposure also reduced the production of another type of T-cell that is pro-inflammatory, and thereby proatherogenic (leading to the production of atherosclerosis). These two effects of UVB light reduce the development and progression of atherosclerosis. Or stated differently, the research shows that sun exposure is critically-important therapy to reduce and prevent heart and other vascular diseases.
Protect your heart by being sure to obtain sufficient non-burning UVB light from sun exposure or other sources such as the UVB lamps used by the researchers. It is important to note that neither skin cancer nor skin inflammation were observed following UVB exposure.
This is another breakthrough study that emphasizes the necessity of sun exposure for human health.
[1] National Psoriasis Foundation web site Oct. 2005.
[2] Yelverton CB, Kulkarni AS, Balkrishnan R, Feldman SR. Home ultraviolet B phototherapy: a cost-effective option for severe psoriasis. Manag Care Interface 2006;19:33-36, 39.
[3] Situm M, Bulat V, Majcen K, Dzapo A, Jezovita J. Benefits of controlled ultraviolet radiation in the treatment of dermatological diseases. Coll Antropol. 2014 Dec;38(4):1249-53.
[4] Gupta A, Arora TC, Jindal A, Bhadoria AS. Efficacy of narrowband ultraviolet B phototherapy and levels of serum vitamin D3 in psoriasis: A prospective study. Indian Dermatol Online J. 2016 Mar-Apr;7(2):87-92.
[5] Naoto Sasaki, Tomoya Yamashita, Kazuyuki Kasahara, Atsushi Fukunaga, Tomoyuki Yamaguchi, et al. UVB Exposure Prevents Atherosclerosis by Regulating Immunoinflammatory Responses. Arterioscler Thromb Vasc Biol. 2016;36:00-00.
DOI: 10.1161/ATVBAHA.116.308063.)
[6] Hafid Ait-Oufella, Andrew P. Sage. Editorial. The Sunlight. A New Immunomodulatory Approach of Atherosclerosis. (Arterioscler Thromb Vasc Biol. 2017;37:7-9. DOI: 10.1161/ATVBAHA.116.308637.)
By Marc Sorenson, EdD, Sunlight Institute…..
Before proceeding with the discussion on sunlight addiction, it is important to review the truth about sunlight and melanoma, to understand why sunlight addiction may be a good thing.
A recent report on ultraviolet light and addiction[1] is obviously meant to be a hit piece regarding sunlight exposure and tanning, as seen in the opening statement: “Despite widespread awareness that UV exposure is a major risk factor for all common cutaneous malignancies, skin cancer incidence relentlessly increases by ~3% per year.”
The “all common cutaneous malignancies” portion of this statement, of course, is patently false. Whereas the relatively benign common skin cancers are increased by exposure to sunlight, melanoma is increased by avoiding the sun. If the dramatic increase in melanoma over the past century were due to sunlight exposure, then sunlight exposure must also have increased dramatically during that time. To determine whether that has happened, we analyzed data from the Office of Occupational Statistics and Employment Projections, Bureau of Labor Statistics, (BLS) to determine if there was an increase or decrease in human sunlight exposure during the years from 1910 to 2,000.[2] The statistics showed that indoor occupations such as “professional, managerial, clerical, sales, and service workers grew from one-quarter to three-quarters of total employment between 1910 and 2000.” BLS also stated that during the same period, the outdoor occupation of farming declined from 33% to 1.2% of total employment, a 96% reduction. The data also showed an approximately 66% decline in the occupation of farmers and 50% of the decline in the occupation of farm laborers.
The Environmental Protection Agency also determined that as of 1986, about 5 percent of adult men worked mostly outside, and that about 10 percent worked outside part of the time. The proportion of women who worked outside was thought to be even lower.[3] These data demonstrate a dramatic shift from outdoor, sun-exposed activity to indoor, non-sun-exposed activity during the mid-to-late 20th Century.
Despite these facts, the Melanoma International Foundation (MIF) has stated that melanoma has increased by 30 times (3,000%) just since 1935! Here is the statement by the MIF: “Melanoma is epidemic: rising faster than any other cancer and projected to affect one person in 50 by 2010, currently it affects 1 in 75. In 1935, only one in 1,500 was struck by the disease.”[4] Indeed, the American Cancer Society in 2014 reported that one in 50 now contracts the disease.[5] That exponential increase in melanoma has been accompanied by a profound decrease in sunlight exposure, yet sunlight or other UV exposure is blamed for the melanoma increase—a totally counterintuitive argument! I submit that not only is sunlight not responsible for the exponential increase in melanoma, but that the decrease in sun exposure may be a major cause of that increase.
Here are other facts that belie the idea that melanoma is caused by sunlight exposure:
- Outdoor workers, while receiving 3-9 times the UVR exposure as indoor workers,[6] [7] have had no increase in melanoma since before 1940, whereas melanoma incidence in indoor workers has increased steadily and exponentially.
- Most melanomas occur on areas of the body that are seldom or never exposed to the sunlight.[8] [9] [10]
- The use of sunscreen, which has increased steadily, has not resulted in a decrease in melanoma.[11] In fact, melanoma has increased as sunscreen use has become more widespread. Since sunscreens block sunlight, it is evident that at best they are a waste of money and at worst may be contributing to the increase in melanoma.
Now, let’s discuss the research on the aforementioned addiction to sunlight. The researchers conducted various experiments on mice that showed behavior choices, such as desiring lighter rather than darker environments, were increased by regular exposure. These behavior choices were mediated by β-endorphins, peptide hormones which are similar to opiates. So is this all bad? This marvelous product, β-endorphin, is one of the feel-good hormones that decreases pain and increases a sense of well-being. The case the researchers make regarding addiction to sunlight is compelling, and why not? Sunlight exposure causes vitamin D production in the skin, which is essential to human health; it also stimulates the production of nitric oxide, which relaxes our vessels and lowers our blood pressure; it stimulates the production of serotonin in the brain, which is another feel-good hormone necessary for a happy mood and wellbeing. And considering the myriad additional effects of sunlight on health, including the prevention of cancer, the prevention and reversal of bone diseases and the reduction of heart disease, could it not be part of God’s (or Nature’s) master plan to develop a positive addiction to sunlight so than our health could be enhanced? I am a sunlight addict, and expose myself to it regularly for two reasons: (1) It marvelously improves my mood and (2) it protects me from disease and weakness. I am a light-skinned, blue-eyed Caucasian who has spent much of my seven decades on this earth seeking the sun. Yet, there have been no melanomas or even common skin cancer.
Nevertheless, the researchers summarize their paper on sun addiction with the following: “While primordial UV addiction, mediated by the hedonic [pertaining to pleasure] action of β-endorphin and anhedonic effects of withdrawal, may theoretically have enhanced evolutionary vitamin D biosynthesis, it now may contribute to the relentless rise in skin cancer incidence in man.”
That summary statement is claptrap, as can be seen by the research on melanoma and sunlight presented above. If sunlight is addictive and helps me to avoid melanoma, heart disease, bone loss and other maladies, I can only say, “hooray for the addiction!”
[1] Gillian L. Fell, Kathleen C. Robinson, Jianren Mao, Clifford J. Woolf, and David E.
Fisher. Skin β-endorphin mediates addiction to ultraviolet light. Cell. 2014 June 19; 157(7): 1527–1534.
[2] Ian D. Wyatt and Daniel E. Hecker. Occupational changes in the 20th century. Monthly Labor Review, March 2006 pp 35-57: Office of Occupational Statistics and Employment Projections, Bureau of Labor Statistics
[3] U.S. Congress, Office of Technology Assessment, Catching Our Breath: Next Steps for Reducing Urban Ozone, OTA-O-412 (Washington, DC: U.S. Government Printing Office, July 1989).
[4] Melanoma International Foundation, 2007 Facts about melanoma. Sources: National Cancer Institute 2007 SEER Database, American Cancer Society’s 2007 Facts and Figures, The Skin Cancer Foundation, The American Academy of Dermatology.
[5] American Cancer Society. Melanoma Skin Cancer Overview 9/16/2014. Accessed on 9/23/2014 at http://www.cancer.org/cancer/skincancer-melanoma/overviewguide/melanoma-skin-cancer-overview-key-statistics
[6] Godar D. UV doses worldwide. Photochem Photobiol 2005;81:736–49.
[7] Thieden E, Philipsen PA, Sandby-Møller J, Wulf HC. UV radiation exposure related to age, sex, occupation, and sun behavior based on time-stamped personal dosimeter readings. Arch Dermatol 2004;140:197–203.
[8] Garland FC, White MR, Garland CF, Shaw E, Gorham ED. Occupational sunlight exposure and melanoma in the USA Navy. Arch Environ Health 1990; 45:261-67.
[9] Rivers, J. Is there more than one road to melanoma? Lancet 2004;363:728-30.
[10] Crombie, I. Racial differences in melanoma incidence. Br J Cancer 1979;40:185-93.
[11] Phillippe Autier. Do high factor Sunscreens offer protection from melanoma? West J Med. 2000 Jul; 173(1): 58.



