Major factors for Covid-19. By Marc Sorenson, EdD
Major factors in Covid-19 and death go far beyond age, lung disease, obesity and heart disease. Two newer studies show that diabetes and Parkinson’s disease are also associated with death among Covid-19 patients. Although scientists commonly accept diabetes as a risk factor for death from Covid, the Parkinson’s information is new and surprising. The Parkinson’s study involved 80,000 patients and the University of Iowa Health Care Center. It showed that Parkinson’s patients with Covid-19 had a 30% greater risk of mortality (death) due to Covid. Of course, that was when compared to patients who did not have Parkinson’s disease. Thus, the researchers found 5.5% (4,290 of 78,355) of Covid-19 patients without Parkinson’s disease died compared to 21.3% patients with Parkinson’s disease.
What is the answer to preventing Parkinson’s disease and therefore reducing the risk of death from Covid-19?
First, the answer is not a drug. Rather, the answer is sun exposure. Parkinson’s is a neurologic disease caused by brain cell deterioration, which decreases dopamine and other major factors. Thus, it results in tremors, (especially of the hands) muscle rigidity, shuffling gait and slow speech. It also closely associates with depression, bipolar disorder and chronic fatigue, and that is not surprising, considering the physical and mental difficulty involved. Sufficient dopamine is essential to proper brain function.
Parkinson’s patients do not have sufficient dopamine. In addition, they have far too little BDNF.
That chemical is brain-derived neurotropic factor (BDNF). It is another major factor, because it helps to promote the survival of dopamine neurons. It is especially relevant that exercise tends to increase BDNF. Another major factor in Parkinson’s is serotonin, the body’s major natural “upper” and a major factor in depression. Finally, depression itself is a major factor in Parkinson’s.
So how does sun deprivation become one of the major factors in the link between Parkinson’s and Covid-19?
Greater amounts of dopamine, serotonin, endorphin and brain-derived neurotropic factor (BDNF) associate with regular sun exposure. Depression also inversely associates with sun exposure. In addition, the onset of bipolar disorder associates with increased hours of daylight at the birth location. If these things were true, we would expect a lower risk of Parkinson’s disease to accompany regular sun exposure. Thus it is. A meta-analysis from Medical Science Monitor showed that people with high sun exposure levels had only 1/50 the risk of contracting Parkinson’s!
An incredible association between sun exposure and Parkinson’s
High sun exposure associates so closely with low risk of Parkinson’s disease that it practically eliminates it. It also associates very closely to the aforementioned major factors for Parkinson’s disease listed above. In addition, we have established that having Parkinson’s increases the death risk from Covid -19 by 30%. It seems like common sense that sunlight would also have a protective effect on Covid-19.
The bottom line regarding major factors for reducing Parkinson’s and Covid-19.
Sun exposure, therefore, is one of the major factors in reducing risk of Parkinson’s, and Parkinson’s is a major factor in death from Covid-19. Do not neglect regular, non-burning sun exposure.
For more information on Covid 19, Parkinson’s disease and related causes, visit https://sunlightinstitute.org/ and read the book, Embrace the Sun.
 Parkinson’s disease prevented by sunlight. By Marc Sorenson, EdD
Parkinson’s disease prevented by sunlight. By Marc Sorenson, EdD
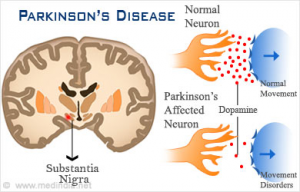 Parkinson’s disease is a common nerve disease, and it is caused by deterioration of brain cells that produce dopamine. It is characterized by tremors, muscle rigidity, shuffling gait, slow speech, and a mask-like facial expression. In addition, even simple movements may become difficult for the person suffering from the disease. And, the disease is a killer that takes the lives of 14,593 per year.[1] So how do we prevent it? In this blog, I will explain the disease, show what the research says about sunlight, and make recommendations for prevention.
Parkinson’s disease is a common nerve disease, and it is caused by deterioration of brain cells that produce dopamine. It is characterized by tremors, muscle rigidity, shuffling gait, slow speech, and a mask-like facial expression. In addition, even simple movements may become difficult for the person suffering from the disease. And, the disease is a killer that takes the lives of 14,593 per year.[1] So how do we prevent it? In this blog, I will explain the disease, show what the research says about sunlight, and make recommendations for prevention.
Research points out that Sun exposure is the key to prevention of Parkinson’s disease.
Several studies have shown that there is a close association between sunlight exposure, blood  vitamin D levels and Parkinson’s. First of all, one paper showed that when vitamin D levels are low, there is a tripling of the risk.[2] Another study from China demonstrated that persons with highest levels of blood vitamin D had a 48% decrease in risk. And, that same research demonstrated that those receiving the greatest sun exposure had about a 47% decrease in risk.[3] So, based on those findings, one might think that vitamin D supplements could prevent the disease. Yet, that thought is erroneous. Sun exposure is the direct key for preventing this debilitating disease.
vitamin D levels and Parkinson’s. First of all, one paper showed that when vitamin D levels are low, there is a tripling of the risk.[2] Another study from China demonstrated that persons with highest levels of blood vitamin D had a 48% decrease in risk. And, that same research demonstrated that those receiving the greatest sun exposure had about a 47% decrease in risk.[3] So, based on those findings, one might think that vitamin D supplements could prevent the disease. Yet, that thought is erroneous. Sun exposure is the direct key for preventing this debilitating disease.
Vitamin D supplements do not stop Parkinson’s, so how can that be?
Recent research, a systematic review and meta-analysis, is most noteworthy. And it explains this interesting paradox.[4] It showed that sun exposure was significantly associated with a reduced risk of Parkinson’s. Especially relevant is the fact that those persons with plenty of sun exposure had only 1/50 the risk of Parkinson’s. That is an astounding figure! However, although vitamin D supplements were effective in raising vitamin D levels, they had no significant benefits for Parkinson’s disease.
Vitamin D and sun exposure are not the same.
While sun exposure and supplements both raise vitamin D levels, supplements are no help to Parkinson’s sufferers. Hence, we must look beyond vitamin D for an answer. Sun exposure leads to the production of vitamin D, but it also leads to the production of dopamine. Dopamine, as previously mentioned, is a vital chemical for the brain as regards Parkinson’s. Vitamin D is a marvelous, vital photoproduct and is due to sun exposure. It is vital for human health. However, it appears that vitamin D does nothing for Parkinson’s. Most of all, we must remember that sun exposure produces many essential photoproducts beyond vitamin D.
Vitamin D blood levels, in the case of Parkinson’s and some other diseases, are simply surrogate measurements of sun exposure. We simply cannot substitute a vitamin D pill for sun exposure and expect to reap all the benefits of sunlight. The “holistic” sun will never be supplanted by a capsule. The sun stimulates the production of vitamin D, dopamine, nitric oxide, serotonin, endorphins, brain-derived neurotropic factor (BDNF) and other photoproducts. And, all of these photoproducts play their roles in human health. For some diseases, vitamin D is vital for prevention. In others such as Parkinson’s, it is just along for the ride.
The takeaway regarding sun exposure and Parkinson’s.
To help prevent this disease, be sure to obtain plenty of non-burning sunlight. And In lieu of that, when there is no sunlight available, use a low-pressure sunbed (tanning bed) in a salon. Always remember not to burn. For more information, read my new book, Embrace the Sun, available at Amazon: https://www.amazon.com/Embrace-Sun-Marc-B-Sorenson/dp/069207600X 
Happy sunning!
[1] ttps://www.rightdiagnosis.com/p/parkinsons_disease/deaths.htm
[2] Knekt P, Kilkkinen A, Rissanen H, Marniemi J, Sääksjärvi K, Heliövaara M. Serum vitamin D and the risk of Parkinson disease. Arch Neurol. 2010 Jul;67(7):808-11.
[3] Wang J, Yang D, Yu Y, Shao G. Wang Q. Vitamin D and Sunlight Exposure in Newly-Diagnosed Parkinson’s Disease. Nutrients 2016;8:142.
[4] Zhou Z, Zhou R, Zhang Z, Li K. The Association between Vitamin D Status, Vitamin D Supplementation, Sunlight Exposure, and Parkinson’s disease: A Systematic Review and Meta-Analysis. Med Sci Monit. 2019 Jan 23;25:666-674.
By Marc Sorenson, EdD, Sunlight Institute…
A new investigation from Chinese researchers demonstrates that sun exposure is dramatically protective against Parkinson’s disease (PD).[1] The paper reported a study in which 201 newly diagnosed patients were compared with 199 controls who were free of PD. Data on vitamin D intake, blood vitamin D levels and sun exposure were obtained in both groups by using a self-report questionnaire.
For blood vitamin D levels, those who had the highest levels had a 48% lowered risk of PD; for sun exposure, those receiving the greatest exposure had about 47% reduced risk of PD.
Whereas a significant positive correlation existed between blood levels of vitamin D and sun exposure, vitamin D intake from supplements, food, etc. did not correlate to blood levels of vitamin D.
This is a particularly interesting study in that it demonstrates that vitamin D should be raised by exposure to the sun when possible rather than dietary intake. It appears that dietary intake the amounts most people receive is not effective for raising those levels.
The evidence for a protective effect of sun exposure against PD has been building for some time. In 1988, it was observed that when four northern census regions of the U.S. were compared with three southern regions, death rates for PD were significantly higher in the northern regions,[2] indicating a possible protective effect of sun exposure. Later research corroborated those findings, demonstrating a strong north-south decreasing gradient for PD among whites.[3]
There are several more studies indicative of a positive effect of sun on PD, and these will be included in the book on sunlight that Dr. William Grant and I are writing, and which we hope to have published in May. Stay tuned, and safely embrace the sun!
[1] Juan Wang, Deyu Yang, Yu Yu, Gaohai Shao and Qunbo Wang 2. Vitamin D and Sunlight Exposure in Newly-Diagnosed Parkinson’s Disease. Nutrients 2016;8:142.
[2] Kurtzke JF, Goldberg ID. Parkinsonism death rates by race, sex, and geography. Neurology. 1988 Oct;38(10):1558-61.
[3] Lanska DJ. The geographic distribution of Parkinson’s disease mortality in the United States. J Neurol Sci. 1997 Sep 1;150(1):63-70.
.Marc Sorenson, EdD, Sunlight Institute
While perusing the medical and scientific literature for research that would be pertinent for my upcoming book on the value of sunlight exposure, I found a most interesting paper on sunlight exposure and bone strength.[i] The researchers searched the literature on three groups of patients, Alzheimer’s, Parkinson’s and Stroke which correlated to very high fracture rates among patients suffering from those diseases. They then found three randomized, controlled studies that determined the efficacy of sunlight exposure for reducing the risk of hip fractures in patients with these diseases.
In each study, there was a control group that did not receive the exposure and an experimental group that received regular sunlight exposure to a small part of the body daily for a year. The results were impressive: For Alzheimer’s patients, the reduction in hip fractures was 78% compared to the controls who stayed inside; for Parkinson’s patients, 73%; for stroke patients, 83%. Overall, the risk of the hip fracture was reduced by 77% in the sunlight exposed groups. Bone mass also increased in each sunlight-exposed group, so osteoporosis was obviously reversed. Did you even realize that such a thing was possible? You probably knew it only if you have been reading the Sunlight Institute blogs. There is an even more impressive study that I always mention when writing about sunlight and osteoporosis. For example, an investigation from Spain in 2008 concluded that women who actively participated in sun exposure had one-eleventh the chance of a hip fracture as those who stayed indoors.[ii] It appears from the materials on the different disease groups mentioned above, that reversibility is a reality, but how much more important is it to prevent the disease in the first place? The women in Spain did exactly that.
The National Osteoporosis Foundation estimates that osteoporosis was responsible for more than 2 million fractures in 2005, including 297,000 hip fractures, 547,000 vertebral fractures, 397,000 wrist fractures, 135,000 pelvic fractures and 675,000 fractures at other sites. The foundation also estimates that the number of osteoporotic fractures is expected to rise to more than 3,000,000 by 2025, and that an average 24 % of hip-fracture patients aged 50 and over die within one year following the occurrence of their fracture.[iii] If we take 24% of just the hip fractures that cause death we see that osteoporosis kills at least 71,280 people per year. Larrosa, M. Vitamin D deficiency and related factors in patients with osteoporotic hip fracture. Med Clin (BARC) 2008;130:6-9.
Do you believe that it might be worth a daily sunbath to save the lives of 70,000 people per year? Do you believe that it would be worth daily exposure (unprotected by sunscreen) to the sun (when possible) to reduce your own risk of fracture? Then why don’t we know about these statistics and the marvelous prophylactic effects of sunlight? That answers are simple: (1) it doesn’t sell any Fosamax or Boniva. (2) It doesn’t sell any noxious, deadly sunscreens. (3) It would be unthinkable for most dermatologists to admit that soaking up a little sun each day might be good for us. It has been said, “And ye shall know the truth and the truth shall make you free.”[iv] Now you have boned up on bone strength and sunlight, and you know the truth.
My fervent hope is that all may be free from the deceptions of those who would ignore the truth in favor of making another dollar.
[i] Iwamoto J, Takeda T, Matsumoto H. Sunlight exposure is important for preventing hip fractures in patients with Alzheimer’s disease, Parkinson’s disease, or stroke. Acta Neurol Scand. 2012 Apr;125(4):279-84
[ii] Larrosa, M. Vitamin D deficiency and related factors in patients with osteoporotic hip fracture. Med Clin (BARC) 2008;130:6-9.
[iii] National Osteoporosis Foundation, Fast Facts on Osteoporosis. Accessed Nov. 20, 2009 at http://www.nof.org/osteoporosis/diseasefacts.htm
[iv] John 8:32 (KJV)