Parkinson’s disease prevented by sunlight. By Marc Sorenson, EdD
Parkinson’s disease prevented by sunlight. By Marc Sorenson, EdD
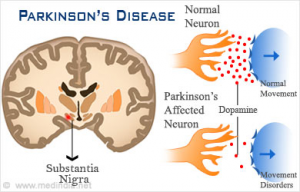 Parkinson’s disease is a common nerve disease, and it is caused by deterioration of brain cells that produce dopamine. It is characterized by tremors, muscle rigidity, shuffling gait, slow speech, and a mask-like facial expression. In addition, even simple movements may become difficult for the person suffering from the disease. And, the disease is a killer that takes the lives of 14,593 per year.[1] So how do we prevent it? In this blog, I will explain the disease, show what the research says about sunlight, and make recommendations for prevention.
Parkinson’s disease is a common nerve disease, and it is caused by deterioration of brain cells that produce dopamine. It is characterized by tremors, muscle rigidity, shuffling gait, slow speech, and a mask-like facial expression. In addition, even simple movements may become difficult for the person suffering from the disease. And, the disease is a killer that takes the lives of 14,593 per year.[1] So how do we prevent it? In this blog, I will explain the disease, show what the research says about sunlight, and make recommendations for prevention.
Research points out that Sun exposure is the key to prevention of Parkinson’s disease.
Several studies have shown that there is a close association between sunlight exposure, blood 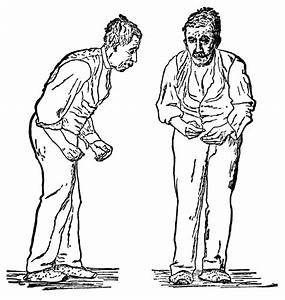 vitamin D levels and Parkinson’s. First of all, one paper showed that when vitamin D levels are low, there is a tripling of the risk.[2] Another study from China demonstrated that persons with highest levels of blood vitamin D had a 48% decrease in risk. And, that same research demonstrated that those receiving the greatest sun exposure had about a 47% decrease in risk.[3] So, based on those findings, one might think that vitamin D supplements could prevent the disease. Yet, that thought is erroneous. Sun exposure is the direct key for preventing this debilitating disease.
vitamin D levels and Parkinson’s. First of all, one paper showed that when vitamin D levels are low, there is a tripling of the risk.[2] Another study from China demonstrated that persons with highest levels of blood vitamin D had a 48% decrease in risk. And, that same research demonstrated that those receiving the greatest sun exposure had about a 47% decrease in risk.[3] So, based on those findings, one might think that vitamin D supplements could prevent the disease. Yet, that thought is erroneous. Sun exposure is the direct key for preventing this debilitating disease.
Vitamin D supplements do not stop Parkinson’s, so how can that be?
Recent research, a systematic review and meta-analysis, is most noteworthy. And it explains this interesting paradox.[4] It showed that sun exposure was significantly associated with a reduced risk of Parkinson’s. Especially relevant is the fact that those persons with plenty of sun exposure had only 1/50 the risk of Parkinson’s. That is an astounding figure! However, although vitamin D supplements were effective in raising vitamin D levels, they had no significant benefits for Parkinson’s disease.
Vitamin D and sun exposure are not the same.
While sun exposure and supplements both raise vitamin D levels, supplements are no help to Parkinson’s sufferers. Hence, we must look beyond vitamin D for an answer. Sun exposure leads to the production of vitamin D, but it also leads to the production of dopamine. Dopamine, as previously mentioned, is a vital chemical for the brain as regards Parkinson’s. Vitamin D is a marvelous, vital photoproduct and is due to sun exposure. It is vital for human health. However, it appears that vitamin D does nothing for Parkinson’s. Most of all, we must remember that sun exposure produces many essential photoproducts beyond vitamin D.
Vitamin D blood levels, in the case of Parkinson’s and some other diseases, are simply surrogate measurements of sun exposure. We simply cannot substitute a vitamin D pill for sun exposure and expect to reap all the benefits of sunlight. The “holistic” sun will never be supplanted by a capsule. The sun stimulates the production of vitamin D, dopamine, nitric oxide, serotonin, endorphins, brain-derived neurotropic factor (BDNF) and other photoproducts. And, all of these photoproducts play their roles in human health. For some diseases, vitamin D is vital for prevention. In others such as Parkinson’s, it is just along for the ride.
The takeaway regarding sun exposure and Parkinson’s.
To help prevent this disease, be sure to obtain plenty of non-burning sunlight. And In lieu of that, when there is no sunlight available, use a low-pressure sunbed (tanning bed) in a salon. Always remember not to burn. For more information, read my new book, Embrace the Sun, available at Amazon: https://www.amazon.com/Embrace-Sun-Marc-B-Sorenson/dp/069207600X 
Happy sunning!
[1] ttps://www.rightdiagnosis.com/p/parkinsons_disease/deaths.htm
[2] Knekt P, Kilkkinen A, Rissanen H, Marniemi J, Sääksjärvi K, Heliövaara M. Serum vitamin D and the risk of Parkinson disease. Arch Neurol. 2010 Jul;67(7):808-11.
[3] Wang J, Yang D, Yu Y, Shao G. Wang Q. Vitamin D and Sunlight Exposure in Newly-Diagnosed Parkinson’s Disease. Nutrients 2016;8:142.
[4] Zhou Z, Zhou R, Zhang Z, Li K. The Association between Vitamin D Status, Vitamin D Supplementation, Sunlight Exposure, and Parkinson’s disease: A Systematic Review and Meta-Analysis. Med Sci Monit. 2019 Jan 23;25:666-674.
Sun avoidance for children. By Marc Sorenson, EdD.
Sun avoidance or sun protection?
Sun avoidance is deadly. And, no one would disagree that sun protection (covering up and seeking shade—not sunscreen use) is essential when one has reached sufficiency, further exposure could cause burning and thereby damage the skin. So, the operative phrase should always be, “protect against sun exposure when one has had enough.” Most noteworthy, however, is the fact that we abuse both our children and ourselves when we demand sun avoidance. This is not to say that the abuse is deliberate, since parents and health professionals alike may have their hearts in the right place. They are simply misinformed and lacking in knowledge.
Is sun avoidance as dangerous as water avoidance?
As a result of withholding water, a child (or adult) will quickly develop multiple organ failures and die. The results with sun avoidance might not be quite so dramatic, yet the same scenario occurs. Much as water deprivation leads to catastrophe, sun deprivation leads to multiple maladies, life-threatening or otherwise. And unfortunately, the term “sun protection,” as used by many dermatologists, means staying out of the sun at all costs. Hence, we could call it sun avoidance. To suggest or promote that idea is not really protective; rather, it might be considered abusive, no?
First of all, the vital need for safe sun exposure in children has been firmly established by research. Therefore, we should review the facts:
- Do we love our little girls? Consider this: those who have the greatest sun exposure have a 35% reduced risk of breast cancer as adults. So sun avoidance, aka “sun protection” may lead to breast cancer.[2] Requiring sun avoidance of girls could be child abuse, no?
- Also, sun exposure in expectant mothers reduces the risk of leukemia and other cancers in their children.[3] Therefore, could encouraging sun avoidance end up as child abuse?
- In addition, children also benefit from sun exposure’s protection against Non-Hodgkin’s-lymphoma (NHL) risk. Sun exposure is associated with a 40% reduced risk.[4] Therefore, could advocating for sun avoidance be child abuse?
More outcomes of sun avoidance in children: prostate cancer, blood pressure, multiple sclerosis and asthma.
- Another point is this: men exposed to high quantities of sunlight as children have one-fifth the risk of contracting prostate cancer.[5] So, is demanding childhood sun avoidance a form of child abuse?
- It is most noteworthy that in children, blood pressure is higher in winter than summer.[6] This is probably due to nitric oxide production by sun exposure to the skin. It is especially relevant to remember that vitamin D is only one of many vital photoproducts stimulated by sun exposure. Therefore, could it be that promoting sun avoidance is child abuse, due to the fact that it may lead to heart disease?
- In addition, adults who experienced low childhood sun-exposure are three times more likely to develop multiple sclerosis (MS).[7] So, does it seem like promulgating sun avoidance could be child abuse?
- Also, living in rooms without sunlight is associated with a 930% increase in the risk of childhood asthma.[8] Hence, could sun avoidance be like child abuse?
Are childhood pneumonia, lower respiratory infection, autism and rickets predicted by sun avoidance?
- First of all, each one-hour increase in sun exposure per day lowers a child’s risk of contracting pneumonia by about 33%.[9] And, pneumonia kills many children. Does promoting sun avoidance seem like child abuse to you? So here is another question: should you also limit your child to only an hour per day outside?
- Another fact is that children with very low blood vitamin D levels are ten times more likely to contract acute lower respiratory infection (ALRI).[10] That is, compared with children with the highest levels. Especially relevant is the fact that about 90% of vitamin D in serum is produced by sun exposure to the skin.[11] Therefore, this study really shows the benefits of sun exposure for children. And, does it also establish that suggesting sun avoidance could be a form of abuse?
- Finally, urban children have significantly higher rates of both rickets and autism when compared to rural children. Lack of sunlight, of course, is the reason.[12] Is this another reason to define sun avoidance as child abuse?
Other disorders associated with sun avoidance in children: bipolar disorder, eczema, myopia, anaphylaxis and rickets.
- Increased number of hours of daylight at the location of birth during the first three months of life are associated with a significantly older age of onset of bipolar disorder.[13] Babies need sunlight, so be sure to carefully provide them substantial, non-burning sun exposure. Why? Because regular sun avoidance for babies might be considered abusive.
- Children with low sun exposure also have a significantly increased risk of eczema.[14] Could sun avoidance, therefore, be considered a form of child abuse?
- Children who spend most of their lives indoors also have 9.5 times the risk of developing myopia compared to children who spend their lives outdoors! So, sun avoidance may lead to blindness in children. Does that constitute child abuse?
- Anaphylaxis is much more prevalent in countries with low sunlight availability.[15] Anaphylaxis can kill. So could sun avoidance, especially in countries that already have low sun exposure, be considered abusive?
- Rickets is returning to the U.S.[16] This can only be due to the lack of sufficient sunlight to produce vitamin D, either in the expectant mother or in the child itself. Therefore, could promoting sun avoidance for these children be considered a form of abuse?
Growth rates, brain cancer and melanoma in children: are they associated with sun avoidance?
- Children’s growth is accelerated in seasons of greater sunlight exposure.[17] Does retarding a child’s growth, through promoting sun avoidance, seems like a good idea to you?
- Children born in seasons of little sunlight have a greater risk of developing brain cancer.[18] Do you really want your children to avoid the sun? That seems like a form of abuse to me.
- Children who engage in outdoor activities are less likely to develop melanoma than those who do not.[19] Since 1935, sun exposure has decreased by 90%. Melanoma has increased by 3,000%. So, promoting sun avoidance seems abusive to me. How about you?
Sun avoidance predicts poor outcomes for dental health in boys.
• Boys (and probably girls) growing up with high sunlight exposure have 40% fewer dental caries than boys who grow up with low exposure. So sun avoidance, aka “sun protection” obviously has a detrimental effect on dental health.[1] Hence, could requiring sun avoidance of boys be child abuse?
No sun avoidance in my youth
As a youngster, I spent most of my days on the farm working in the sunlight. No illnesses developed in the summer. And, I never had a skin cancer later in life. How can that be? I am a blue-eyed, light skinned Caucasian, and yet skin cancer never materialized. So did sun exposure protect me? Probably. I was never subjected to sun avoidance, the abuse that is so prevalent today.
Caution! Remember that at no time should you burn yourself. People who cannot tan need to stop sun exposure to the skin at the first sign of redness. Work into a few minutes of sunlight over days or weeks if necessary. And, one way for light-skinned non-tanners to obtain sun is to be under a beach umbrella in a bathing suit. Nevertheless, do not burn. Watch for reddening and cover up immediately if it occurs.
Words of caution regarding sunscreens
Caution! Don’t think that sunscreens will help you avoid damage. That is because they are not sun protection. First of all, the latest research, a meta-analysis, shows that sunscreen use does not make any difference in skin-cancer risk.[20] Secondly, other late research also shows that people who use sunscreens are much more likely to experience sunburns than non-users.[21] As a result, those who used sunscreens were about two-and-one-half-to-four-times more likely to sunburn compared to those who used other methods to prevent excessive exposure. Hence, covering up with clothing or seeking shade is a far better method of protection than sunscreens, which are no protection at all. Could the use of sunscreens with children constitute sun avoidance and be another form of abuse?
Embrace the Sun, but do it carefully, and please do not engage in the abusive practice known as sun avoidance.
Read more about sun avoidance and children’s diseases in my new  book, Embrace the Sun, available at Amazon. https://www.amazon.com/Embrace-Sun-Marc-B-Sorenson/dp/069207600X
book, Embrace the Sun, available at Amazon. https://www.amazon.com/Embrace-Sun-Marc-B-Sorenson/dp/069207600X
Also, read hundreds of blogs on sunlight at http://sunlightinstitute.org/
[1] McBeath, E. The role of vitamin D in control of dental caries in children. J Nutr 1938;15:547.
[2] Knight JA, Lesosky M, Barnett H, Raboud JM, Vieth R. Vitamin D and reduced risk of breast cancer: a population-based case-control study. Cancer Epidemiol Biomarkers Prev 2007;16(3):422-9.
[3] Christina Lombardi, Julia E. Heck, Myles Cockburn, and Beate Ritz. Solar UV Radiation and Cancer in Young Children. Cancer Epidemiol Biomarkers Prev 2013;22:1118-1128.
[4] Petridou ET, Dikalioti SK, Skalkidou A, Andrie E, Dessypris N, Trichopoulos D. Sun exposure, birth weight and childhood lymphomas: a case control study in Greece. Cancer Causes Control. 2007 Nov;18(9):1031-7.
[5] Moon SJ, Fryer AA, Strange RC. Ultraviolet radiation: effects on risks of prostate cancer and other internal cancers. Mutat Res 2005;571(1-2):207-19.
[6] Polat M, Akil I, Yuksel H, Coskun S, Yilmaz D, Erguder I, Onag A. The Effect of seasonal changes on blood pressure and urine specific gravity in children living in Mediterranean climate. Med Sci Monit 2006;12:CR186-90.
[7] van der Mei IA, Ponsonby AL, Dwyer T, Blizzard L, Simmons R, Taylor BV, Butzkueven H, Kilpatrick T. Past exposure to sun, skin phenotype, and risk of multiple sclerosis: case-control study. BMJ 2003;327:316-321.
[8] Kamran A, Hanif S, Murtaza G. Risk factors of childhood asthma in children attending Lyari General Hospital. J Pak Med Assoc 2015 Jun;65(6):647-50.
[9] Paynter S, Weinstein P, Ware RS, Lucero MG, Tallo V, Nohynek H, Barnett AG, Skelly C, Simões EA, Sly PD, Williams G; ARIVAC Consortium. Sunshine, rainfall, humidity and child pneumonia in the tropics: time-series analyses. Epidemiol Infect. 2013 Jun;141(6):1328-36.
[10] Wayse V, Yousafzai A, Mogale K, Filteau S. Association of subclinical vitamin D deficiency with severe acute lower respiratory infection in Indian children under 5 y. Eur J Clin Nutr 2004;58:563-7.
[11] Reichrath J. The challenge resulting from positive and negative effects of sun: how much solar UV exposure is appropriate to balance between risks of D deficiency and skin cancer? Prog Biophys Mol Biol 2006;92(1):9-16.
[12] Williams JG, Higgins JP, Brayne CE. Systematic review of prevalence studies of autism spectrum disorders. Arch Dis Child 2006;91:8-15
[13] Bauer M, Glenn T, Alda M, Andreassen OA, Angelopoulos E, Ardau R, Baethge C, Bauer R et al. Influence of light exposure during early life on the age of onset of bipolar disorder. J Psychiatr Res. 2015 ;64:1-8.
[14] Rueter K, Jones AP, Siafarikas A, Lim EM, Bear N, Noakes PS, Prescott SL, Palmer DJ. Direct infant UV light exposure is associated with eczema and immune development. J Allergy Clin Immunol. 2018 Oct 15. [Epub ahead of print]
[15] Mullins RJ, Camargo CA. Latitude, sun, vitamin D, and childhood food allergy/anaphylaxis. Curr Allergy Asthma Rep. 2012 ;12(1):64-71.
[16] Weisberg P, Scanlon KS, Li R, Cogswell ME. Nutritional rickets among children in the United States: review of cases reported between 1986 and 2003. Am J Clin Nutr 2004;80(6 Suppl):1697S-705S
[17] Marshall WA. Evaluation of growth rate in height over periods of less than one year. Arch Dis Child. 1971;46:414–420.
[18] Heuch JM, Heuch I, Akslen LA, Kvåle G. Risk of primary childhood brain tumors related to birth characteristics: a Norwegian prospective study. Int J Cancer 1998;77:498-503.
[19] Kaskel P, Sander S, Kron M, Kind P, Peter RU, Krähn G. Outdoor activities in childhood: a protective factor for cutaneous melanoma? Results of a case-control study in 271 matched pairs.Br J Dermatol. 2001 Oct;145(4):602-9.
[20] Silva ESD, Tavares R, Paulitsch FDS, Zhang L. Use of sunscreen and risk of melanoma and non-melanoma skin cancer: a systematic review and meta-analysis. Eur J Dermatol. 2018 Apr 1;28(2):186-201.
[21] Kasey L. Morris, PhD; Frank M. Perna, EdD, PhD. Decision Tree Model vs Traditional Measures to Identify Patterns of Sun-Protective Behaviors and Sun Sensitivity Associated With Sunburn. JAMA Dermatol. Published online June 27, 2018
 An innate need for sunlight exists within the human body and soul.
An innate need for sunlight exists within the human body and soul.
First of all, consider the opening line of a recent article in the New York Times: “Let there be light. Please.” And, the article states that people in New York City (NYC) love to seek apartments with sunlight. It is also especially relevant that such apartments demand premium prices. But sun seekers have a problem because of the continuous building of new high rises. Consequently, they must look at the city’s future building plans before they fulfill their innate need for sunlight. This is because new buildings may be built that block whatever sunlight is available.
Problems encountered in fulfilling the innate need for sunlight in NYC.
Therefore, it is a difficult situation to satisfy the innate need for sunlight in NYC. And no wonder people in the southern states have lower cancer rates, despite their atrocious eating habits.[1] Why? Because they have one of the best cancer fighters: sunlight.
An example of the rather impressive anti-cancer power of sunlight: Iranian research demonstrated the innate need for sunlight. Women who avoided sun exposure had 10 times the breast cancer risk.[2] That is, of course, when they were compared to women who were able to obtain regular sunlight. This is because the innate need for sunlight was being ignored among women forced to avoid sun.
What other diseases are manifest when we ignore our innate need for sunlight?
Lack of sun exposure increases the risk of 16 other cancers, heart disease, vitamin D deficiency, multiple sclerosis, hip fractures, depression and myriad others. (See my book, Embrace the Sun, for a full discussion.) The innate need for sunlight manifests itself in higher rates of these “killer” diseases worldwide.
According to the NYT article, “there are those who view light as an elemental need, one that trumps everything else, including location, closets, level floors, an elevator, a doorman and proximity to Trader Joe’s.” Obviously, the people recognize, at a visceral level, their innate need for sunlight.
Do the Chinese have an innate need for sunlight?
Another article also emphasized the innate need for sunlight.[3] And, this one came from halfway around the world, in Shanghai. It seems like the Chinese should know about sun healing, since their experience in healing goes back thousands of years. Hence, they would not need to read this article to appreciate the innate need for sunlight. A real-estate developer there had to pay a family the equivalent of $15,650.00 for robbing them of their sun. One of the developer’s skyscrapers exceeded the legal height, and partially blocked the sun to their apartment. Consequently, this prevented the family from obtaining their government-mandated sun allotment. The allotment was two hours per day, and the skyscraper allowed only 1-2 hours of sun.
A judge who understands the innate need for sunlight
The judge in the case said, “We can’t live without sunshine” and told the developers they had to respect the rights of the people to enjoy the sun. Due to this judge’s understanding of the innate need for sunlight, justice was done.
Why is the innate need for sunlight not recognized in the U.S? Good question!
The Chinese experience is in stark contrast with the US. First of all, in the 1990s, a president of the American Academy of Dermatology (AAD) made this statement. “In some vision as I grow older I see us moving to more shelters and perhaps underground living because of these hazards” (meaning sun exposure).[4] Also, she stated that melanoma would cause more cancer deaths than any other cancer by about 2010. Since it is now 2018, and we are not yet living underground, she was ridiculously wrong. In addition, melanoma is nowhere near the top of the cancer-deaths charts. It kills far less people than most major cancers like lung, breast, colon and prostate. However, it will probably increase in incidence as more people are convinced by the ADD to avoid their innate need for sunlight.
When it comes to the innate need for sunlight, the Chinese have more smarts!
It appears that the Chinese are a whole lot smarter than the AAD regarding the innate need for sunlight! Therefore, the AAD’s insistence on sun avoidance is likely to destroy public health. And, soaking up some safe, unobstructed, regular sunlight will enhance health. The AAD’s insistence on sun avoidance is much more likely to destroy the health of the American public than soaking up some unobstructed sunshine. So please, PLEASE enjoy some safe, non-burning sun, winter and summer, while you improve your health! And remember that sunscreens inhibit 95% of vitamin D production. Therefore, when you have had enough sun exposure, cover up with clothing or seek shade. Those who use sunscreens have far more sunburns than those who do not use it.[5] Think about it, and read my book, Embrace the Sun so that you can be comfortable while attending to your innate need for sunlight. https://www.amazon.com/Embrace-Sun-Marc-B-Sorenson/dp/069207600X 
[1] Sorenson, M. Vitamin D3 and Solar Power. Chapter 8. 2008.
[2] Bidgoli SA, Azarshab H. Role of vitamin D deficiency and lack of sun exposure in the incidence of premenopausal breast cancer: a case control study in Sabzevar, Iran. Asian Pac J Cancer Prev. 2014;15(8):3391-6.
[3] http://www.shanghaidaily.com/national/Sun-suit-Family-wins-payout/shdaily.shtml
[4] Dr. Wilma Bergfeld, then-president of the American Academy of Dermatology at Derm Update, the AAD’s 1996 annual media day, Nov. 13, 1996.
[5] Silva ESD, Tavares R, Paulitsch FDS, Zhang L. Use of sunscreen and risk of melanoma and non-melanoma skin cancer: a systematic review and meta-analysis. Eur J Dermatol. 2018 Apr 1;28(2):186-201.
Vitamin D levels: sufficient for winter? By Marc Sorenson, EdD
 Vitamin D levels and sunshine are exceptionally important to human health, and therefore we should be aware of vitamin D science. The Vitamin D Society of Canada is always at the forefront of the research on vitamin D levels and sunlight. And, they deliver press releases to keep people from Canada (and the world) apprised of new and important findings. Hence, I would like to comment on the salient points of their latest release. As I do so, it is especially relevant to note that vitamin D levels are surrogate measures for sun exposure.
Vitamin D levels and sunshine are exceptionally important to human health, and therefore we should be aware of vitamin D science. The Vitamin D Society of Canada is always at the forefront of the research on vitamin D levels and sunlight. And, they deliver press releases to keep people from Canada (and the world) apprised of new and important findings. Hence, I would like to comment on the salient points of their latest release. As I do so, it is especially relevant to note that vitamin D levels are surrogate measures for sun exposure.
The relationship of vitamin D to sun exposure
Ninety percent of vitamin D levels in the blood is due to sun exposure.[1] The UVB portion of sunlight stimulates vitamin D production in skin. Therefore, a UVB light source, which produces vitamin D levels, is the best source in winter. Remember also that the press release information is true for the world, not just Canada.
Salient points about vitamin D levels and sunlight: breast cancer
- First of all, consider a breast-cancer study published in the scientific journal, Plos One.[2] It showed that women with the highest vitamin D levels had a reduced breast-cancer risk. Most noteworthy, women with levels > 60 ng/ml had 82% reduced risk, compared to those with levels < 20 ng/ml. Furthermore, there was a dose-response decrease. For each increase in vitamin D levels, there was a concomitant decrease is breast-cancer risk.
Vitamin D levels and Breast Cancer
- Since we mentioned that vitamin D is produced by sun exposure, we should mention an Iranian sunlight-breast cancer study. In Iran, among women who totally avoid sun exposure, there is a 10-fold increase breast cancer risk.[3] That is an especially relevant fact for women who believe they should avoid the sun! And remember, melanoma is also reduced in those who are regularly exposed to sunlight.[4]
Another Vitamin D levels- and sunlight-deficiency cancer
- It seems like if breast cancer is reduced by high vitamin D levels, the same relationship could exist for other cancers. Hence, the press release mentioned colorectal cancer as the second disease associated to low vitamin D levels or low sun exposure. And, it mentioned another important piece of research.[5] Participants with vitamin D levels below 12 ng/ml had a 31% higher risk of colorectal cancer. Those with levels above 30 ng/ml had a 27% reduced risk.
Other disorders associated with vitamin D levels
In addition, the press release mentions four other disorders where higher vitamin D levels reduce risk or improve the condition. The disorders: diabetes (81% reduced risk), multiple sclerosis (45% reduced risk), preterm birth (62% reduced risk) and poor cognitive function. As to cognitive function, those who spent the most time outdoors with the least sun protection, had better cognitive function.
Finally, this is an excellent press release regarding vitamin D levels and sunlight. I strongly suggest you read it. http://www.vitamindsociety.org/press_release.php?id=60 Also, see the previous blog regarding the vitamin D Society and vitamin D levels: http://sunlightinstitute.org/vitamin-d-canada-warning/
Vitamin D and sunlight are sine qua nons for health, and so are proper nutritional habits. Happy health! Be sure to read my book, Embrace the Sun, available at Amazon. 
[1] Reichrath J. The challenge resulting from positive and negative effects of sun: how much solar UV exposure is appropriate to balance between risks of vitamin D deficiency and skin cancer? Prog Biophys Mol Biol 2006;92(1):9-16
[2] McDonnell SL, Baggerly CA, French CB, Baggerly LL, Garland CF, Gorham ED, Hollis BW, Trump DL, Lappe JM. Breast cancer risk markedly lower with serum 25-hydroxyvitamin D concentrations ≥60 vs <20 ng/ml (150 vs 50 nmol/L): Pooled analysis of two randomized trials and a prospective cohort. PLoS One. 2018 Jun 15;13(6).
[3] Bidgoli SA, Azarshab H. Role of vitamin D deficiency and lack of sun exposure in the incidence of premenopausal breast cancer: a case control study in Sabzevar, Iran. Asian Pac J Cancer Prev. 2014;15(8):3391-6.
[4] Vågero D, Ringbäck G, Kiviranta H. Melanoma and other tumors of the skin among office, other indoor and outdoor workers in Sweden 1961–1979. Brit J Cancer 1986;53:507–12.
[5] McCullough ML, Zoltick ES, Weinstein SJ, Fedirko V, Wang M, et al. Circulating Vitamin D and Colorectal Cancer Risk: An International Pooling Project of 17 Cohorts. J Natl Cancer Inst. 2018 Jun 14.
 Vitamin D is essential in Canada (and Ely). By Marc Sorenson, EdD.
Vitamin D is essential in Canada (and Ely). By Marc Sorenson, EdD.
I just received an excellent press release from my friend Perry Holman, who is touting the Canadian Vitamin D Day. Perry is the Executive Director of the Vitamin D Society. The Society is alarmed about the lack of sunlight and vitamin D production during the long Canadian winter. The points made in the press release, however, are also relevant for all areas of the U.S. that have long, cold winters. This would include Ely, Nevada, my high-school hangout. Therefore, this blog contains a couple of editorial comments regarding Ely and other points in the U.S. [Ely, Minnesota would certainly need this advice too.]
The current lack of vitamin D is due to of the position of the sun in the winter sky. All of the UVB light that stimulates vitamin D production (and many other essential photoproducts) is filtered out when the sun drops too close to the southern horizon.
Here are a few of the salient points made in the release:
- Vitamin D levels plummet this time of year, since the sun can no longer make vitamin D. [This is also true of Ely, NV, where most vitamin D production ceases on about October 1. It starts up again about March 1.]
- 93% of Canadians are vitamin D deficient. [For Ely, the number is probably closer to 50%, but for the Northern states in the U.S., the number is probably closer to 80%.
- This deficiency leads to 23,000 premature deaths yearly in Canada. See this link: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5129897/pdf/kder-08-01-1248324.pdf
- There are two primary sources of vitamin D Canadians should consider during the winter – artificial UVB exposure and vitamin D3 supplements.
- Artificial UVB exposure can be a surrogate for summer sunshine and is obtained from most sunbeds or through special UVB lamps designed for home use.
- A recent Canadian study found that regular use of sunbeds with UVB similar to outdoor summer sun significantly raised participants’ vitamin D levels to the optimal range. See this link: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5821157/
- Perry Holman states: “The current health policy limiting sun exposure may be causing more deaths and disease than its preventing. Vitamin D levels have been dropping and more people are becoming vitamin D deficient in Canada. We need a change in direction to encourage people to get moderate non-burning sun exposure to prevent vitamin D deficiency and reduce the risk of serious diseases.” [My comment here is that the research in my book shows the following: for every single death caused by diseases associated with sun exposure, there are approximately 328 deaths caused by diseases associated with sun deprivation.]
Whether you live in Canada, Ely, Nevada, or anywhere else where you either avoid the sun or have no availability of vitamin D-producing sunlight during the colder seasons, you should read this press release. http://www.vitamindsociety.org/press_release.php?id=59
Happy sunning, and as another of my Canadian friends says, “Have a D-lightful day!” And, read my new book, Embrace the Sun, available at Amazon: https://www.amazon.com/Embrace-Sun-Marc-B-Sorenson/dp/069207600X/ref=sr_1_1?ie=UTF8&qid=1540903899&sr=8-1&keywords=embrace+the+sun+sorenson
An infant breakthrough! Our babies need sunlight! By Marc Sorenson, EdD
An infant may return to the sun due to exciting new research from Australia.[1] The researchers surmised that vitamin D deficiency might explain the high rates of infant allergic diseases. They specifically measured infant eczema. Eczema and other allergic diseases are common in areas of industrialization and high latitudes. Thus, eczema could indicate low vitamin D levels. The researchers made this statement: “Suboptimal vitamin D levels during critical periods of immune development have emerged as an explanation for higher rates of allergic diseases associated with industrialization and residing at higher latitudes.” That seems like wisdom, yet, as you’ll see, they turned out to be wrong.
The infant study: UV light or vitamin D?
So, the researchers set out to determine the effects of early-life vitamin D supplementation on infant allergy prevention. In addition to supplementation, they also outfitted some infants with a dosimeter to also measure UV exposure. This group was compared to a placebo group. In addition, each infant was assessed from birth until age six months. This was done because about 90% of vitamin D is produced by sun exposure to the skin. Vitamin D is an important photoproduct of sunlight. And I opine that sun exposure is of much greater importance. Why? Because sun exposure and its UV light lead to the production of many essential photoproducts beyond vitamin D. Also, a high vitamin D level may simply be a surrogate measurement for sun exposure in some cases. Consequently, other photoproducts such as nitric oxide, serotonin, endorphins, dopamine, BDNF and many others may be the health givers. (For a list of more photoproducts, see my last blog, called Holistic Sun). An infant may need all that the sun can provide, including vitamin D.
The results for infant eczema risk
The results were surprising to the researchers but not to me, based on the facts stated in the above paragraph. So, infant vitamin D levels were greater for the supplemented group than the placebo group.at three and six months, That seems like an expected outcome. Most noteworthy, however, was that there was no difference in eczema incidence between infant groups. And also especially relevant was the fact that those who showed the most UV (sun) exposure had the least risk. In addition, the children with eczema had only a bit over half the UV exposure. Vitamin D simply made no difference to eczema.
The researchers’ conclusion regarding infant eczema
Therefore, the researchers wrote the following: “This study is the first to demonstrate an association between greater direct UV light exposures in early infancy with lower incidence of eczema and pro inflammatory immune markers by 6 months of age. Our findings indicate that UV light exposure appears more beneficial than vitamin D supplementation as an allergy prevention strategy in early life.”
In conclusion, UV exposure from sunlight, tanning lamps or tanning beds is far more important that vitamin D per se. And sun exposure also produces vitamin D in the way God (or nature if you prefer), intended. Why should we accept one pill containing vitamin D, when we can obtain the entire package of photoproducts with UV-containing sunlight? For more information on sunlight, eczema and psoriasis, read my new book, Embrace the Sun, Available at Amazon. Also read my previous blog, Holistic Sun.
[1] Rueter K, Jones AP, Siafarikas A, Lim EM, Bear N, Noakes PS, Prescott SL, Palmer DJ. Direct infant UV light exposure is associated with eczema and immune development. J Allergy Clin Immunol. 2018 Oct 15. [Epub ahead of print]
The term holistic, as used for this discussion
 The term holistic (my definition) derives from the word “whole.” Hence, the term incorporates the idea that in nutrition, a whole food functions better than any of its parts. And, it means that when we treat diseases, we should treat the whole person. As an example of holistic nutrition, consuming whole-grains associates with better health than consuming refined grains.[1] Probably, the poor results associated with refined white bread are due to the removal of nutrients during processing. As a result, the bread is no longer holistic. Furthermore, we can state that it is no longer a whole food. Stay with this discussion. Holistic sun will be discussed to sum up.
The term holistic (my definition) derives from the word “whole.” Hence, the term incorporates the idea that in nutrition, a whole food functions better than any of its parts. And, it means that when we treat diseases, we should treat the whole person. As an example of holistic nutrition, consuming whole-grains associates with better health than consuming refined grains.[1] Probably, the poor results associated with refined white bread are due to the removal of nutrients during processing. As a result, the bread is no longer holistic. Furthermore, we can state that it is no longer a whole food. Stay with this discussion. Holistic sun will be discussed to sum up.
Other examples: holistic foods and non-holistic supplements
Especially relevant is that whole rice strongly associates with protection against disease, whereas refined rice increases risk.[2] Another example is the case in which a nutrient from a plant is extracted and encapsulated. Since the nutrient is subtracted from a food, neither the nutrient nor the food remains holistic. And, such food manipulation is based on observations that high levels of the nutrient in the body is associated with better health. Therefore, we might expect this encapsulated product to produce healthful outcomes. And, in some cases it does produce positive results. However, the product may also be totally ineffective or counterproductive.
Holistic vegetables vs non-holistic beta carotene and vitamin E
An example of this is supplementation with beta carotene. Beta carotene is a nutrient found in carrots and other orange and yellow vegetables. Since people who consume large quantities of these vegetables seem to be healthier, a question emerges. Could concentrated beta carotene produce a health miracle?[3]
Testing the possibility: Can supplements beat holistic vegetables?
So to test that possibility, researchers gave one group of cancer patients beta carotene pills (not holistic). They gave other patients a placebo. Opposite from the researchers’ expectations, the cancer increased with beta carotene supplementation.[4] Consequently, these adverse results led to the discontinuation of the research. Furthermore, similar results have been shown with vitamin E supplementation.[5] While beta carotene and vitamin E are wonderful, they must work as part of the holistic team.
What about the health of those who eat holistic foods containing beta carotene?
And what about those who have high beta carotene levels due to a high intake of colorful vegetables? It is most noteworthy to again mention that high carotene levels still predict better health. These vegetables contain innumerable, healthful chemical compounds, only one of which is beta carotene. Hence, when beta carotene is part of the magnificent, holistic orchestra of nutrients, it helps to produce a beautiful health concert. In conclusion, whole foods—or holistic foods—will be better for human health than a single, isolated nutrient. And remember this. Junk foods are never holistic.
Is the sun holistic, or do we need only to take a vitamin D pill?
 So, can the sun be holistic? Yes! First of all, the idea of a holistic sun was the reason I wrote my latest book, Embrace the Sun. I had noted numerous studies where vitamin D, the major photoproduct of sun exposure, sometimes failed as a supplement. In other cases it seemed to work quite well. Yet, when sun exposure was tested for the expected result, that result was almost invariably positive. At this point, I must make it clear that there are many studies showing that vitamin D supplementation can produce terrific, healthful outcomes. This is especially true when vitamin D deficiency is present. But since sun exposure produces many other healthful photoproducts, why should we settle for just one? Beyond vitamin D, here are few additional photoproducts produced by sun exposure.
So, can the sun be holistic? Yes! First of all, the idea of a holistic sun was the reason I wrote my latest book, Embrace the Sun. I had noted numerous studies where vitamin D, the major photoproduct of sun exposure, sometimes failed as a supplement. In other cases it seemed to work quite well. Yet, when sun exposure was tested for the expected result, that result was almost invariably positive. At this point, I must make it clear that there are many studies showing that vitamin D supplementation can produce terrific, healthful outcomes. This is especially true when vitamin D deficiency is present. But since sun exposure produces many other healthful photoproducts, why should we settle for just one? Beyond vitamin D, here are few additional photoproducts produced by sun exposure.
Photoproducts that are part of the holistic sun’s health arsenal:
- Sun exposure increases nitric oxide production, which immediately lowers blood pressure and leads to a decrease in heart disease risk.[6] Taking a D pill does not produce this result.
- Sun exposure dramatically improves mood through the production of serotonin.[7] This result is nearly immediate and not triggered by vitamin D.
- Sun exposure increases the production of BDNF, part of a cascade of proteins promoting growth of neurons and preventing nerve death.[8] This result is not triggered by vitamin D. BDNF is a major player on the holistic sun’s team.
More holistic photoproducts:
- Sun exposure increases the production of endorphin, another mood enhancer.[9] This is a non-vitamin D response.
- UVB light from sun, sunlamps or sunbeds directly helps heal psoriasis.[10] This is not a vitamin D response.
- Sun exposure also leads to the production of several additional natural chemicals that enhance human health. Here are a few: Alpha melanocyte-stimulating hormone, Calcitonin gene-related peptide and Neuropeptide substance P. A full discussion of them here would become too cumbersome for this blog.
Summary: the importance of holistic sun
So, suffice it to say that the holistic sun has many benefits beyond the production of vitamin D. And remember, sunbeds and sunlamps can furnish the holistic effects of sun exposure when sunlight is not available. These include the production vitamin D, which, when combined with the other photoproducts, enhances health to a far greater extent than vitamin D alone. Hence, we might say that the photoproducts of sun exposure are synergistic—the holistic sun being far more effective than any of its individual parts. When major players are taken away from the orchestra, the concert is not as good. Don’t let that happen with your holistic sun. Be sure that all of the sun’s remarkable photoproducts are working for you, including vitamin D.
In conclusion, Embrace the Holistic Sun safely and reap the health benefits. Don’t burn and don’t use sunscreens, which take away one of the major players in your orchestra: vitamin D. Have a sunny week!
[1] Tayyem RF, Bawadi HA, Shehadah I, Agraib LM, Al-Awwad NJ, Heath DD, Bani-Hani KE. Consumption of Whole Grains, Refined Cereals, and Legumes and Its Association With Colorectal Cancer Among Jordanians. Integr Cancer Ther. 2016 Sep;15(3):318-25.
[2] Musa-Veloso K, Poon T, Harkness LS, O’Shea M, Chu Y. The effects of whole-grain compared with refined wheat, rice, and rye on the postprandial blood glucose response: a systematic review and meta-analysis of randomized controlled trials. Am J Clin Nutr. 2018 Oct 1;108(4):759-774
[3] Alpha-Tocopherol, Beta Carotene Cancer Prevention Study Group. The effect of vitamin E and beta carotene on the incidence of lung cancer and other cancers in male smokers. N Engl J Med. 1994 Apr 14;330(15):1029-35.
[4] Tanvetyanon T, Bepler G. Beta-carotene in multivitamins and the possible risk of lung cancer among smokers versus former smokers: a meta-analysis and evaluation of national brands. Cancer. 2008 Jul 1;113(1):150-7
[5] Alpha-Tocopherol, Beta Carotene Cancer Prevention Study Group. The effect of vitamin E and beta carotene on the incidence of lung cancer and other cancers in male smokers. N Engl J Med. 1994 Apr 14;330(15):1029-35.
[6] Weller R. The health benefits of UV radiation exposure through vitamin D production or non-vitamin D Pathways. Blood pressure and cardiovascular disease. Photochem. Photobiol. Sci. 2016.
[7] Lambert GW, Reid C, Kaye DM, Jennings GL, Esler MD. Effect of sun and season on serotonin turnover in the brain. Lancet. 2002 Dec 7;360(9348):1840-2.
[8] http://scicurious.scientopia.org/2010/12/13/bdnf-and-depression/
[9] Aubert PM, Seibyl JP, Price JL, Harris TS, Filbey FM, Jacobe H, Devous MD Sr Adinoff B. Dopamine efflux in response to ultraviolet radiation in addicted sunbed users. Psychiatry Res. 2016 30;251:7-14.
[10] National Psoriasis Foundation web site Oct. 2005.
Multiple sclerosis is a sunlight-deficiency disease. Another reason to embrace the sun. By Marc Sorenson, EdD
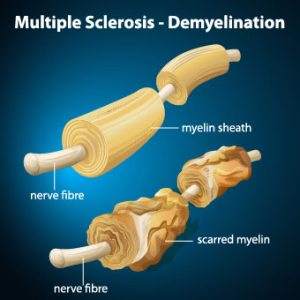 First of all, multiple sclerosis is a terrible autoimmune disease in which immune cells attack myelin, the protective nerve cover.[1], [2] Hence, this process, known as demyelination, leaves the nerves bare and susceptible to “short circuiting.” This results in a debilitating disease which is often characterized by severe neural and muscular impairments. It may also result in sensory losses, bladder dysfunction, pain and visual problems due to nerve damage.
First of all, multiple sclerosis is a terrible autoimmune disease in which immune cells attack myelin, the protective nerve cover.[1], [2] Hence, this process, known as demyelination, leaves the nerves bare and susceptible to “short circuiting.” This results in a debilitating disease which is often characterized by severe neural and muscular impairments. It may also result in sensory losses, bladder dysfunction, pain and visual problems due to nerve damage.
MS is a big problem!
And recent findings, from National MS Society, estimate 1 million people in the United States have multiple sclerosis. Furthermore, this is more double the last reported number, and the first national research on multiple sclerosis prevalence since 1975. Consequently, it is estimated that about 200 new cases are diagnosed each week in the United States.[3]
Multiple sclerosis and sun exposure: What does new research say?
While no one disputes the horror of an increasing MS rate, a new study reiterates the vital need for sun exposure to prevent MS. Also, we are not surprised about the latest research. Why? Because the new study is simply a reiteration of myriad research papers and opinions showing that more sunlight reduces the risk.
In this research, 151 MS patients defined their previous lifetime sun exposure in the different seasons by questionnaire. In addition, they were compared to 235 non-patients who answered identical questionnaires.[1] As a result, those living in high-UVB areas experienced a 45% lower risk of multiple sclerosis. Living in those areas at ages 5 to 15 years also was associated with a reduced risk of 51-52%. UVB, of course, is a spectrum of light that emanates from the sun and causes tanning. In addition, it is used in sunbeds and sun lamps.
The conclusion regarding MS and sunlight.
In conclusion to their research, the authors stated, “Living in high ambient UVB areas during childhood and the years leading up to MS onset was associated with a lower MS risk. High summer sun exposure in high ambient UVB areas was also associated with a reduced risk.”
While this research is impressive, there is a plethora of additional science. Most noteworthy are the studies that follow. And, all show the association of sun exposure to lowered risk of MS.
Multiple sclerosis and the Davenport study
Probably, the most important early study was from 1922 by Dr. Charles Davenport. He wrote a paper entitled, “Multiple Sclerosis from the standpoint of geographic distribution and race.”[2] He analyzed the multiple sclerosis rates of military draftees and compared it to their states of origin. As a result, he showed that the highest rates were found in men who grew up in Michigan, Wisconsin, and the extreme northwest. These areas, of course, have very low sun availability. There were only a few cases of MS among those who grew up in southern states, where sun availability is abundant. In addition, Dr. Davenport also noted that draftees from urban areas, and where sun availability is low, had 50% higher MS rates than those who came from rural areas. Similar studies confirm that relationship. [3],[4] In 1979, assessments of the MS rates of USA military personnel Produced nearly identical results.[5]
Reducing relapse of multiple sclerosis through sunlight and/or vitamin D.
Mowry and colleagues, in correlating serum vitamin D to the rate of disease relapse, have reported the following: For every increase in serum levels of 10 ng/ml [25 nmol/L], there is a 34% decrease in the risk of relapse in young people.[6] Especially relevant, however, is that 90% of serum levels is derived from sun exposure. And, we also know that sun exposure has protective effects on MS beyond vitamin D.[7] Also, in the aforementioned research on vitamin D, high levels may really be surrogate measures for sun exposure. Sunlight and vitamin D are not the same.
More hours of sun equal lower risk of multiple sclerosis.
Most noteworthy, among people living in geographical locations, where there are 3,000 hours of available sun yearly, multiple sclerosis rates are quite low. [8] The same relationship exists when latitudes are correlated with rates of MS: And, The risk of MS in far northern areas is more than 100 times greater than it is in equatorial areas, where sunlight is intense, and the rate of MS approaches zero.[9], [10]
Therefore, for all who would like to prevent MS or reduce its exacerbation, soak up some regular, non-burning, safe sunlight. In conclusion, this is another of the wonderful benefits of our magnificent sun. It seems like a good time to indulge before the winter comes.
Finally, for more information on multiple sclerosis, read my new book, Embrace the Sun, available at Amazon.
References and footnotes
[1] Helen Tremlett, PhD, Feng Zhu, MSc, Alberto Ascherio, MD, DrPH, and Kassandra L. Munger, ScD.
[2] Davenport, C. Multiple Sclerosis from the standpoint of geographic distribution and race. Arch Neurol Psychiatry 1922;8:
[3] Acheson ED, Bachrach CA, Wright FM. Some comments on the relationship of the distribution of multiple sclerosis to altitude, solar radiation and other variables. Acta Psychiat (Scand) 1960;35 (suppl 147):132-47.51-58
[4] Norman JE Jr, Kurtzke JF, Beebe GW. Epidemiology of multiple sclerosis in USA veterans: 2. Latitude, climate, and risk of multiple sclerosis. J Chron Dis 1983;36:551-59
[5] Kurtzke JF, Beebe GW, Norman JE Jr. Epidemiology of multiple sclerosis in USA veterans: 1. Race, sex, and geographic distribution. Neurology 1979;29:1228-35.
[6] Mowry EM, Krupp LB, Milazzo M, Chabas D, Strober JB, Belman AL, McDonald JC, Oksenberg JR, Bacchetti P, Waubant E. Vitamin D status is associated with relapse rate in pediatric-onset MS. Annals of Neurology 2010;10.1002.
[7] Pantazou V, Schluep M, Du Pasquier R. Environmental factors in multiple sclerosis. Presse Med. 2015 ;44(4 Pt 2):e113-20.
[8] Goldberg, P. Multiple sclerosis: vitamin D and calcium as environmental determinants of prevalence (a viewpoint). Part I: sun, dietary factors and epidemiology. Int J Environ Studies 1974;6:19–27.
[9] Alter M, Yamoor M, Harshe M. Multiple sclerosis and nutrition. Arch Neurol l974;31:267-72.
[10] Kurtkze, J. Geography in multiple sclerosis. J Neurol 1977;215:1-26.
[1] Racke, M. Immunopathogenesis of multiple sclerosis. Ann Indian Acad Neurol. 2009 Oct–Dec; 12(4): 215–220.
[2] Markovic-Plese S, McFarland HF. Immunopathogenesis of the multiple sclerosis lesion. Curr Neurol Neurosci Rep 2001;1:257-62
[3] https://www.healthline.com/health/multiple-sclerosis/facts-statistics-infographic#2
 Bone needs vitamin D
Bone needs vitamin D
Bone is deteriorating in our society. Why? Since the year 2000, there has been an 8,300% increase in vitamin D deficiency in children. Insufficient time playing outdoors and/or sunscreen use are the causes of this disaster.[1] It is especially relevant to know that the skin produces vitamin D when it is touched by ultraviolet light (UV). (UV, of course, is a spectrum of sunlight, and of tanning beds and sunlamps.) And, the artificially-lighted environments that most children (and adults) live in, produce no vitamin D for bones. Vitamin D is critical for preventing osteoporosis, a fact that is most noteworthy for this discussion. Without vitamin D, weak bones develop in adults and rickets can develop in children.
Bone strength in children: Rickets is making a comeback.
Rickets is a horrible, disfiguring children’s bone disease. And, before the population became terrified of sun exposure, rickets was at one time considered to be eradicated. Hence, people are surprised to find out that the bones of children are deteriorating. Hence, rickets is making a frightening comeback,[2] it is rearing its ugly head even in sun drenched southern states. That is probably because the children are inside, avoiding the sun and concentrating on their technology. Of course, disuse of the body during this sedentary state also causes loss of calcium, thus causing weakness.
Can “sun supplementation” stop or reverse bone loss?
Therefore, the latest research on UV supplementation is exceptionally important in this world of indoor artificial light. First of all, rats exposed to long–term low-dose ultraviolet irradiation showed an increase in bone formation rate. Furthermore, there was a decrease in resorption (bone breakdown). And, there was an improvement in bone mass content and bone mineral density without any adverse effects on skin.[3] Consequently, this research shows that the concept of ultraviolet light causing skin cancer is incorrect. Also, it corroborates how effective ultraviolet light is in maintaining and increasing bone mass. For example, a Spanish study shows that women who are sun-seekers are protected from bone loss. They have only one/11 the risk of hip fracture as those who avoid the sun.[4]
Bring the UV light inside to protect bone and enhance wellbeing.
In conclusion, this research demonstrated a concept that had never occurred to me. If we can’t bring the children (or adults) out into the sunlight, perhaps we can bring the sunlight inside to them. Also, it seems like a great idea to use low-intensity ultraviolet light indoors for northern climes where sunlight is scarce in the winter. I guarantee that it will also improve moods, reduce seasonal affective disorder and otherwise enhance the health. So remember regular, non-burning sun exposure when you consider a healthful lifestyle.
[1] Basatemur E, Horsfall L, Marston L, Rait G, Sutcliffe A. Trends in the Diagnosis of Vitamin D Deficiency. Pediatrics. 2017 Mar;139(3).
[2] Weisberg P, Scanlon KS, Li R, Cogswell ME. Nutritional rickets among children in the United States: review of cases reported between 1986 and 2003. Am J Clin Nutr 2004;80(6 Suppl):1697S-705S.
[3] Guo R, Du Y, Zhang S, Liu H, Fu Y. The effects of ultraviolet supplementation to the artificial lighting on rats’ bone metabolism, bone mineral density, and skin. J Photochem Photobiol B. 2018 Aug 27;188:12-18.
[4] Larrosa M, Casado E, Gómez A, Moreno M, Berlanga E, Ramón J, Gratacós J. Vitamin D deficiency and related factors in patients with osteoporotic hip fracture. Med Clin (BARC) 2008;130:6-9.